Concussion Recovery: You’ve been told the CT scan was clear. The MRI was clean. The neurologist couldn’t find anything wrong. The urgent care doctor cleared you to return to work, school, or sport days after your injury. And yet — weeks later, months later, sometimes years later — you are still not yourself.
The headaches won’t quit. The brain fog rolls in every afternoon. You can’t tolerate the lights at Publix. You feel dizzy walking down the cereal aisle. Your sleep is wrecked. Your patience is gone. You burst into tears over things that wouldn’t have fazed you before. You forget words mid-sentence. You feel anxious for no reason. Your heart races when you stand up. And every single person in your life — even the ones who love you the most — has slowly stopped asking how you’re feeling, because they’ve run out of things to say.
If any of that sounds familiar, please understand three things right now: You are not crazy. You are not exaggerating. And you are absolutely not alone.
Concussions are one of the most under-diagnosed, under-treated, and misunderstood injuries in modern medicine. Every single week, patients come into our office in Sarasota with stacks of normal imaging, “cleared to return” notes from urgent care, and a long list of life-disrupting symptoms that no provider has been able to explain. What we find — over and over and over again — is that the missing piece of the puzzle lives in a place almost nobody ever checks: the top two bones of the neck.
At Lavender Family Chiropractic / NeckWise North Sarasota, we are an upper cervical specialty office located at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243. Our team — Dr. Rusty Lavender, Dr. Jacob Temple— focuses exclusively on the precise, gentle correction of the atlas (C1) and axis (C2) vertebrae using 3D CBCT imaging and Tytron functional nervous system scans. We proudly serve patients throughout Sarasota, Bradenton, Lakewood Ranch, Venice, Osprey, Port Charlotte, Parrish, and Palmetto, along with the surrounding Southwest Florida communities.
This is the article we wish every concussion patient could read the day after their injury — and the article we want every person stuck in post-concussion syndrome to find before they give up hope.
Concussion Recovery: What a Concussion Actually Is (And What Most People Get Wrong)
A concussion is a mild traumatic brain injury (mTBI) caused by a sudden force that makes the brain move rapidly inside the skull. It does not require a direct blow to the head. It does not require loss of consciousness. It does not require a positive scan. In fact, the overwhelming majority of concussions show up as completely normal on CT and MRI — because concussions are a functional injury, not a structural one.
When your head whips, snaps, or rotates suddenly — from a car accident on I-75, a sports collision at Cardinal Mooney, a slip on wet tile at home, a fall off a paddleboard at Lido Key, a kid who headbutts you in the chin, an e-bike crash on the Legacy Trail — three things happen almost simultaneously:
- The brain shears against the inside of the skull, stretching neurons and disrupting their ability to fire normally.
- A metabolic cascade begins inside the brain — cells dump potassium, take on calcium, and burn through glucose at an enormous rate, leaving you in an energy crisis for days to weeks.
- The upper neck — particularly the atlas (C1) and axis (C2) — almost always shifts out of its normal alignment, because the head weighs 10–12 pounds and the muscles holding it in place are not designed for sudden whip-like forces.
That third point is the one almost everyone misses. You cannot concuss the brain without also injuring the neck. It is physically impossible. The same forces that shake the brain also strain, sprain, and shift the upper cervical spine. Yet most patients are evaluated only from the eyebrows up, sent home with a printout that says “rest, hydrate, avoid screens,” and left to wonder why they are still struggling six months later.
Even worse: many patients don’t even remember the concussion that started everything. We routinely see people whose post-concussion symptoms began after a fender-bender they walked away from, a fall they thought was nothing, a sports hit that “didn’t even ring my bell,” or a gymnastics tumble from when they were 12 years old. The brain remembers. The neck remembers. The nervous system remembers. And until the underlying mechanical issue is corrected, the body can’t fully move on.
The Symptoms You’re Probably Living With
Concussion symptoms are infamous for being vague, shifting, and easy to dismiss. The most common include:
- Headaches (especially at the base of the skull or behind the eyes)
- Dizziness, vertigo, or a constant feeling of being “off”
- Brain fog, difficulty concentrating, word-finding problems
- Sensitivity to light and sound
- Nausea
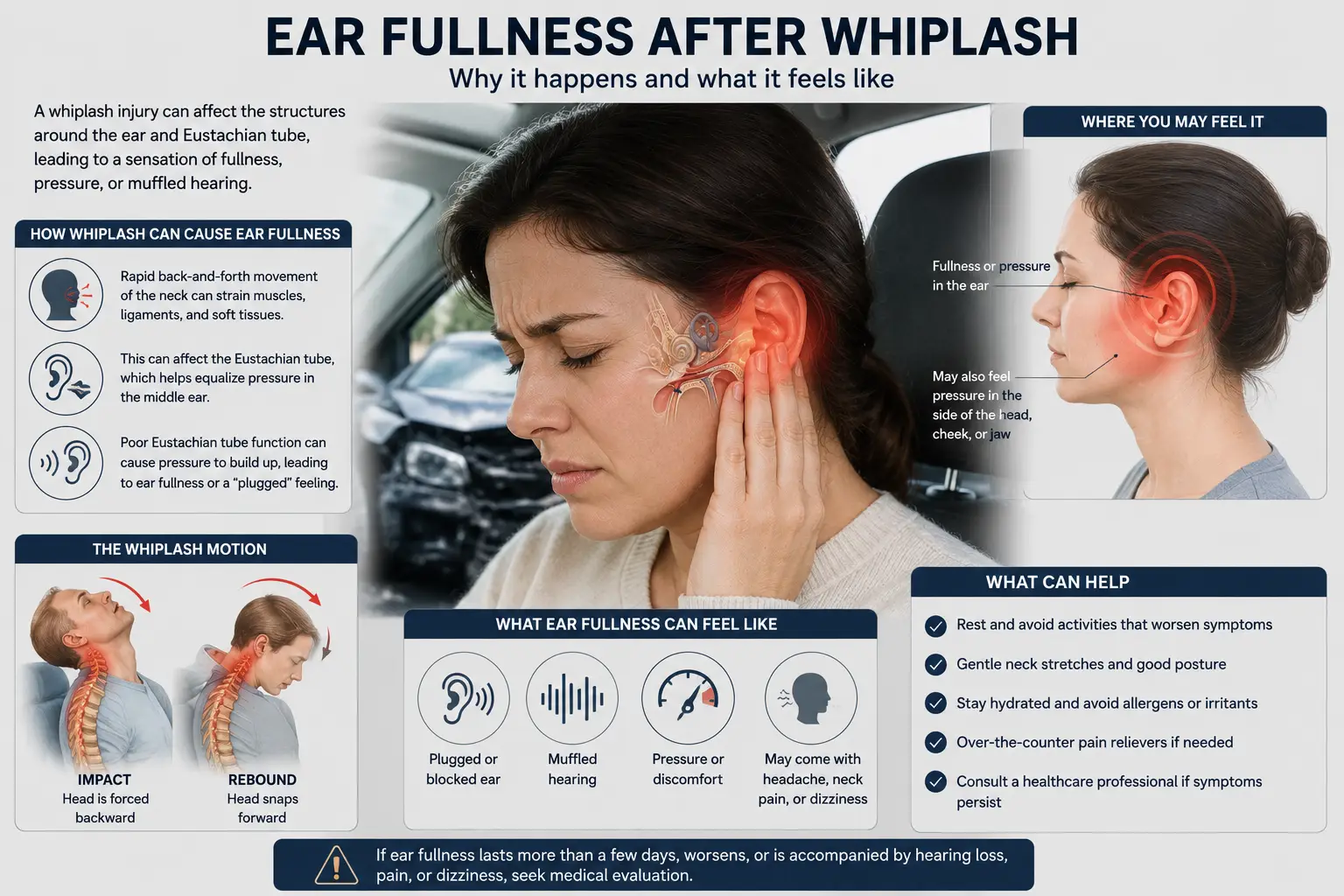
- Neck pain and stiffness
- Fatigue that doesn’t improve with rest
- Sleep disturbances — either insomnia or sleeping too much
- Anxiety, irritability, depression, or emotional lability
- Blurred vision, double vision, or eye strain
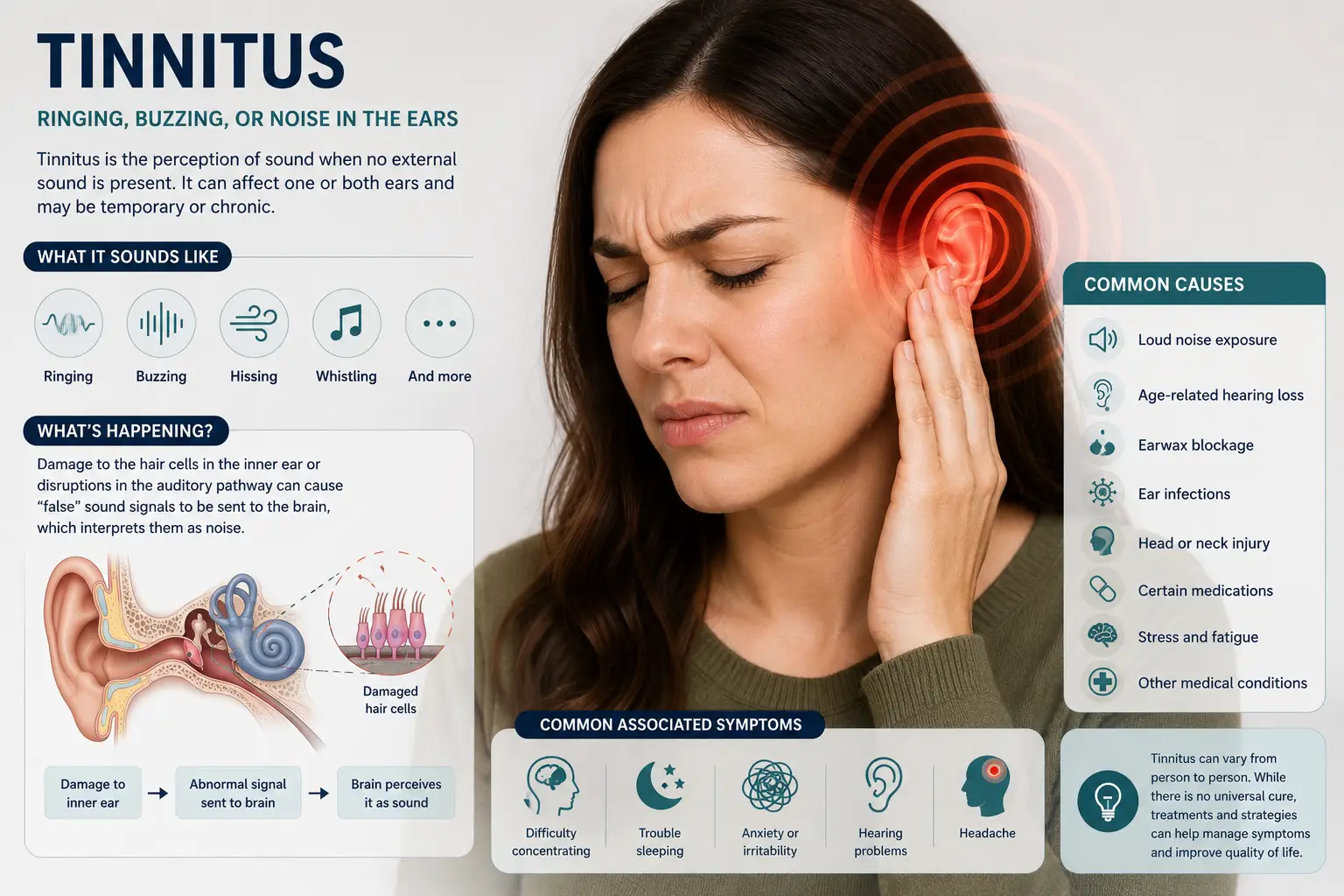
- Tinnitus (ringing in the ears)
- Heart rate that races when you stand up (POTS-like symptoms)
- Difficulty with balance and coordination
- Memory issues
- Feeling “not like yourself”
Most concussion symptoms resolve within 7–14 days for the average person. So why do an estimated 15–30% of people develop post-concussion syndrome (PCS) — where symptoms last for months, years, or even decades? Modern research is finally catching up to what upper cervical doctors have been seeing clinically for over 80 years: the neck is the missing link.
When patients come to us already exhausted from trying everything else — neurology consults, vestibular therapy, vision therapy, cognitive rehab, every supplement under the sun — and we image their upper cervical spine, the answer is almost always staring back at us in 3D. The atlas is misaligned. The brainstem is irritated. The nervous system is stuck in survival mode. And until that is corrected, no amount of downstream therapy can fully restore them.
Why the Upper Neck Is the Real Culprit in Most Concussion Cases
Your atlas (C1) is the very top vertebra of your spine. It is shaped like a ring, sits directly under the skull, and is the only vertebra in your entire body without a disc above or below it. It is held in place purely by ligaments and small muscles. The brainstem — the most critical piece of neurological real estate in your entire body — passes directly through this ring.
When the atlas is even a fraction of a millimeter out of position, several catastrophic things happen:
1. Brainstem irritation. The brainstem controls your autonomic nervous system, balance, eye movement, sleep, mood, heart rate, blood pressure, and digestion. Mechanical pressure or tension at this level produces nearly the entire concussion symptom list — which is why so many seemingly unrelated symptoms can stem from a single source.
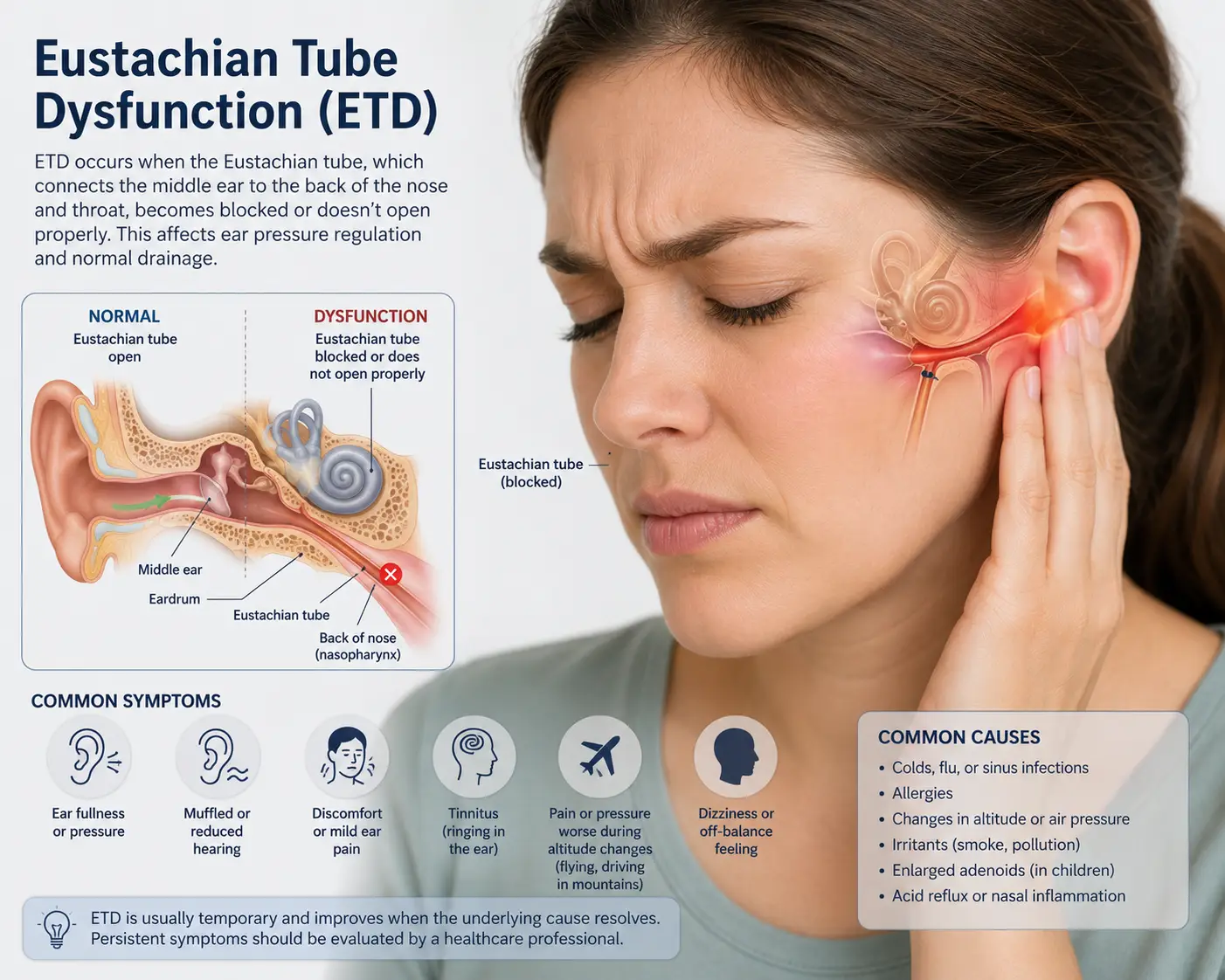
2. Cerebrospinal fluid (CSF) flow disruption. CSF is the fluid that bathes your brain and spinal cord, removes waste, and reduces pressure. The atlas sits at the exact location where CSF flows in and out of the skull. A misaligned atlas can disrupt this flow, leading to brain fog, headaches, intracranial pressure, and that classic “head full of cotton” feeling.
3. Vertebral artery compromise. Two arteries pass through the atlas on their way to feed the back half of your brain — the part that controls balance, vision, and coordination. Subtle restriction of blood flow here creates persistent dizziness, visual disturbances, and that “almost passing out” feeling when you turn your head.
4. Vagus nerve dysfunction. The vagus nerve exits the skull right next to C1. It controls your parasympathetic (“rest and digest”) nervous system. When it’s irritated, you live in fight-or-flight — anxiety, racing heart, poor digestion, and terrible sleep all become your new normal.
5. Proprioceptive chaos. Your upper neck contains more proprioceptive nerve endings per square inch than any other part of your body. These nerves tell your brain where your head is in space. When they fire incorrectly, your brain receives mismatched signals from your eyes, inner ears, and neck — producing dizziness, motion sensitivity, and visual problems that no amount of vestibular therapy alone can fix until the input is corrected.
This is why so many concussion patients never fully recover. They’ve been treated as if the problem is purely in the brain, when the actual driver of their lingering symptoms is a mechanical and neurological dysfunction in the upper neck that nobody has ever assessed.
If you’d like a deeper dive into how this specific style of care works and why it’s different from anything else you’ve likely tried, our Upper Cervical Chiropractic Care guide walks through the science, the diagnostics, and the patient experience step-by-step.
Post-Concussion Syndrome: When “Just Rest” Stops Working
The standard advice after a concussion is rest, hydration, avoiding screens, and gradually returning to activity. For about 70–85% of people, that’s enough — symptoms resolve within two weeks and life returns to normal.
But for the other 15–30%, the standard protocol fails. These are the patients who end up in our office months or years later, often saying some version of: “I was never the same after that car accident in 2019.” Or “My daughter played soccer through high school — she had three concussions, and now in college she can’t get out of bed.” Or “I fell off a ladder six months ago and I still can’t drive at night because of the dizziness.”
If this sounds like you, please understand: post-concussion syndrome is not a life sentence, and it is not in your head.It is almost always a sign that something mechanical has not been addressed — and in our experience, that something is almost always the atlas.
We’ve also written extensively about the conditions that frequently overlap with PCS — chronic migraines, vestibular migraines, occipital neuralgia, dizziness, balance problems, TMJ, ear pressure, and tinnitus. If you’re a Sarasota or Bradenton resident dealing with several of these conditions at once, there’s a very high chance they all stem from a single underlying problem at the top of your neck. Our team has seen this pattern thousands of times — which is why we’ve built our entire practice around it. You can read more about the comprehensive, individualized approach we take with complex cases like these in our Customized Treatment Plans guide.
Concussions and Vertigo: A Connection Almost No One Is Treating Correctly
Of all the post-concussion symptoms patients present with, dizziness and vertigo are arguably the most disabling and the most poorly addressed. Patients describe it as the room spinning, a constant sense of swaying, feeling drunk without drinking, or just being permanently “off.” They get diagnosed with BPPV, vestibular migraine, vestibular neuritis, MdDS, or PPPD. They get sent to vestibular therapy. They try Epley maneuvers, brand exercises, prescription meclizine. Some get partial relief. Many get none.
Here’s what’s happening: when your atlas is misaligned, your upper cervical spine sends faulty proprioceptive signals to your brain. Your inner ear is sending one signal. Your eyes are sending another. Your neck is sending a third. Your brain has to constantly reconcile these mismatched inputs — and the result is the chronic, low-grade, never-quite-resolves dizziness that defines so many post-concussion cases.
Vestibular therapy alone cannot fix this. It can train your brain to compensate, but until you correct the bad input from your neck, you are training your brain to work around a permanent error. Once we restore proper atlas alignment, vestibular therapy works dramatically better — and many patients no longer need it at all.
If dizziness, balance problems, or that “always swaying” feeling have been a major part of your post-concussion experience, our deep-dive Best Vertigo Treatment guide covers exactly how upper cervical care addresses cervicogenic vertigo, post-traumatic vertigo, BPPV, PPPD, and the full spectrum of post-concussion balance disorders.
What Makes Upper Cervical Chiropractic Different (And Why It Works for Concussions)
Most people, when they hear “chiropractor,” picture a forceful neck twist with loud popping sounds. That is not what we do at Lavender Family Chiropractic / NeckWise North Sarasota.
Upper cervical chiropractic is a specialty within chiropractic that focuses exclusively on the precise correction of the atlas and axis. There is no twisting, no cracking, no popping. The corrections are gentle, specific, and based on imaging — not guesswork.
Here’s what makes our approach different from anything else you’ve tried:
1. 3D CBCT (Cone Beam Computed Tomography) imaging. Before we ever touch your neck, we take a detailed 3D scan that shows the exact position of your atlas down to fractions of a degree and millimeter. We then calculate a custom correction angle unique to your anatomy. No two patients receive the same adjustment.
2. Tytron functional nervous system scanning. This thermographic scan measures the heat patterns coming off your spine, giving us an objective look at how your nervous system is functioning before and after each correction. We can literally see your nervous system calming down as your atlas holds.
3. Gentle, low-force corrections. The actual correction takes about 2 seconds, involves no twisting, and most patients describe it as “weirdly subtle.” There is no popping or cracking. The science behind this style of correction goes back to research from the 1930s and has been refined for nearly a century.
4. We measure whether you’re holding. A correction that doesn’t hold is a correction that doesn’t help. We re-scan you at every visit to make sure the work is sticking. Once your atlas stabilizes, you need fewer and fewer visits — the goal is always to get you to a place where you don’t need us very often.
5. We treat the cause, not the symptoms. We’re not trying to numb your headache, suppress your dizziness, or distract you from your brain fog. We’re trying to restore the mechanical and neurological foundation of your head and neck so your body can do the actual healing.
For patients who want to dive deeper into the specific specialty system we use, our NeckWise North Sarasota page explains the full NeckWise protocol — a thoughtful, precise, and neurologically focused approach designed to restore alignment, maintain stability, and let your body heal over time, rather than chasing endless appointments and temporary relief.
This approach is different from traditional concussion rehab, vestibular therapy, vision therapy, or physical therapy — and that’s not to say those don’t have a place. They often do. But if your atlas is misaligned, those therapies will work harder, take longer, and produce smaller results than they should. Correct the atlas first, and everything downstream tends to respond faster.
Real Patients, Real Results in Sarasota and Beyond
We see concussion and post-concussion patients from all over Southwest Florida — high schoolers from Riverview, Out-of-Door Academy, and Cardinal Mooney; college athletes home for the summer; pickleball players from Lakewood Ranch and Venice; cyclists from the Legacy Trail; surfers from Siesta Key; and plenty of patients who were rear-ended on I-75 and never fully bounced back.
Common stories we hear:
- “I had a soccer concussion in 9th grade and I’ve had headaches every single day since. I’m 27 now.”
- “I was in a fender-bender that didn’t even seem that bad — but I haven’t slept right in two years.”
- “My son’s been pulled out of school because of post-concussion syndrome. He played hockey his whole life. We’ve tried everything.”
- “I fell off my paddleboard last summer and now I can’t tolerate grocery store lighting.”
- “I have brain fog so bad I can’t do my job. The neurologist said my MRI is clean.”
- “I was a competitive gymnast — I’ve had more concussions than I can count, and I haven’t felt like myself in 15 years.”
The unifying thread? When we image these patients, we almost always find a significant atlas misalignment. And when we begin specific upper cervical care, the symptoms that have plagued them for months or years often start improving within weeks.
We don’t promise miracles — every person heals differently and at their own pace. But we do see, over and over, that the body’s capacity to heal from concussion is often gated by a single mechanical issue that goes undetected by every other type of provider. Our Atlas Chiropractic guide features several real patient case studies — including post-concussion patients — that illustrate exactly what this kind of healing can look like.
Why Sarasota Patients Are Choosing Natural Concussion Care
The standard medical approach to lingering concussion symptoms generally involves some combination of: medication for headaches, medication for sleep, medication for anxiety, medication for nausea, vestibular therapy, vision therapy, and waiting it out. This works for some patients. For many, it doesn’t — and the side effects of the medications often add a whole new layer of problems on top of the concussion itself.
Natural concussion treatment looks different. The goal is not to suppress symptoms but to remove the obstacles preventing your brain and nervous system from healing. At our Sarasota office, the natural approach we use combines:
- Specific upper cervical correction to restore proper atlas alignment, blood flow, CSF flow, and brainstem function
- Targeted nutritional support — concussion recovery is metabolically expensive, and most patients are deficient in the nutrients their brain needs to repair (omega-3s, magnesium, B-vitamins, antioxidants)
- Sleep optimization — sleep is when the brain heals; we work hard to address the upper cervical drivers of insomnia
- Hydration and electrolyte balance — especially important for concussed patients in Florida heat
- Gradual reintroduction of movement and exercise — once the atlas is stable, light aerobic activity actually accelerates healing
- Light, sound, and screen tolerance training — building back your sensory threshold without flaring symptoms
- Stress and nervous system regulation — concussions wreck the autonomic nervous system, and breath work, vagal toning, and proper sleep hygiene matter enormously
Patients drive in from Bradenton, Lakewood Ranch, Venice, Osprey, Port Charlotte, Parrish, and Palmetto specifically because we don’t approach concussion care like everyone else. We don’t rush you. We don’t dismiss symptoms because your scan looks normal. And we don’t keep you adjusting forever — we get you stable and let your body do its work.
Concussions in Children, Teens, and Athletes: A Special Word to Parents
Pediatric and adolescent concussions deserve a special note because they are massively under-treated and the long-term consequences of missing them can be severe.
If your child has had any of the following, please take it seriously — even if they “seem fine”:
- A fall from a bike, scooter, golf cart, or playground equipment
- A sports collision (football, soccer, hockey, lacrosse, cheerleading, gymnastics, basketball, wrestling)
- A car accident, even a minor one
- A horse-related fall
- A diving or trampoline accident
Kids and teens often hide concussion symptoms because they don’t want to be pulled from sport, school, or social events. They will tell you they’re “fine” while suffering massive headaches, mood swings, sleep disruption, declining grades, and personality changes that the entire family has chalked up to puberty, stress, or a “phase.”
We see student athletes from across Sarasota and Manatee County who are still suffering years after concussions everyone forgot about. Many of them have been on stimulants, antidepressants, anti-anxiety medications, or migraine medications that no one ever connected back to the original head injury. When we correct the underlying upper cervical issue, the entire picture often shifts within weeks.
Our gentle, low-force, instrument-assisted technique is uniquely suited for pediatric patients. There is nothing forceful about it. Many parents bring in entire families because once one person experiences upper cervical care, they want their kids checked too.
When You Should Absolutely Seek Emergency Care
We have to be clear: upper cervical chiropractic is for patients with stable, post-acute concussion symptoms. If you are in the immediate aftermath of a head injury, or if you experience any of the following at any point, please seek emergency medical care immediately:
- Loss of consciousness lasting more than 30 seconds
- Repeated vomiting
- Seizures
- Slurred speech
- Severe or rapidly worsening headache (“worst headache of my life”)
- One pupil larger than the other
- Inability to wake up
- Weakness, numbness, or loss of coordination on one side of the body
- Confusion that worsens rather than improves
These symptoms can indicate serious bleeding, swelling, or structural injury in the brain that requires emergency imaging and intervention. We are not a substitute for emergency medical care — we are a complement to it, and we step in once the acute danger has passed and the lingering symptoms become the issue.
Frequently Asked Questions
How long after a concussion can I start upper cervical care? We typically recommend waiting 7–10 days after the initial injury, assuming there are no red flags and you’ve been medically cleared. Many patients benefit most when they begin within the first 30 days — but we also see incredible results with patients who are years post-injury.
Will the adjustment hurt my head or make symptoms worse? The corrections we use are extremely gentle and low-force. Some patients feel slightly “weird” or fatigued for a day after their first correction as the nervous system recalibrates, but we have never had a concussion patient report a worsening of their underlying symptoms from the adjustment itself.
How many visits will I need? Every patient is different. Most concussion patients see meaningful changes within 4–8 weeks of consistent care, with continued improvement over 3–6 months. Once stable, visits become less frequent — many patients move to a maintenance schedule of once a month or less.
Do you take insurance? Our office is out of network with insurance. We provide a superbill you can submit for potential reimbursement. We made this choice so we can spend the time each visit deserves rather than running you through a 6-minute insurance-driven appointment.
Is this safe for kids and teenagers? Yes. Our gentle, low-force approach is actually ideally suited for pediatric and adolescent concussion patients. We see a lot of student athletes from across Sarasota and Manatee County. Sports concussions in particular often involve significant atlas displacement, and addressing that early can prevent years of lingering symptoms.
Can you help if my concussion was years ago? Yes. While early intervention is ideal, we routinely see patients who are 5, 10, even 20+ years out from their original injury — and they still respond to care. The body remembers its concussion, but it can also still heal once the underlying mechanical issue is corrected.
What if I have multiple concussions stacked on top of each other? This is incredibly common — and incredibly responsive to upper cervical care. Multiple concussions tend to compound atlas misalignment. The good news is that correcting the underlying mechanical issue often produces dramatic improvement even in patients with significant concussion history.
Will I need imaging? Yes — but the imaging is fast, low-radiation, and incredibly useful. Our 3D CBCT scan is one of the most precise tools available for visualizing the upper cervical spine and is significantly more detailed than a standard X-ray.
What to Expect at Your First Visit
Your first appointment is a thorough conversation and assessment, not a treatment. We sit down with you, listen to your full history (yes, the whole thing — including the head injuries you forgot about until we asked), perform a series of upper cervical orthopedic and neurological tests, and run your initial Tytron scan.
If we believe upper cervical care is a fit for your case, we’ll schedule a follow-up to take CBCT imaging and review everything in detail before we ever touch your neck. If we don’t believe we can help, we’ll tell you — honestly — and refer you to a provider who can.
We don’t promise outcomes, because every body is different. But we do promise honest assessment, careful diagnostics, gentle and specific care, and a team that will walk alongside you every step of the way.
Related Articles From Our Blog
If you found this guide helpful, here are five additional in-depth reads from our team that frequently overlap with concussion and post-concussion symptoms. These are some of the most-read articles on our site — and many concussion patients benefit from understanding these connected conditions:
1. Best Vertigo Treatment: A Comprehensive Guide Featuring Lavender Family Chiropractic Dizziness, BPPV, vestibular migraine, PPPD, and post-traumatic vertigo are some of the most common — and most under-treated — symptoms after a concussion. This guide breaks down why the upper cervical spine is so often the missing link in lasting vertigo relief.
2. Vestibular Migraines and Upper Cervical Care: A Comprehensive Guide to Relief If your post-concussion symptoms include dizziness and headaches and light/sound sensitivity, you may actually be dealing with vestibular migraine — a frequently misdiagnosed overlap condition. This article explains the connection in detail.
3. Occipital Neuralgia Relief in Sarasota: How Upper Cervical Chiropractic Helps You Heal at the Source Many concussion patients suffer from sharp, stabbing, or electric-shock-like pain at the base of the skull — a hallmark of occipital neuralgia. This is one of the conditions most directly linked to upper cervical misalignment after head trauma.
4. Why Does My Head Hurt From Barometric Pressure? Our #1 Guide to Storm Headaches Post-concussion patients often become extremely weather-sensitive, with symptoms flaring before storms or pressure changes. This guide explains the fascinating connection between the upper cervical spine, barometric pressure, and head pain — especially relevant in Florida.
5. Atlas Chiropractic in Sarasota: Unlocking Your Body’s True Potential Through Life Changing Care A deep dive into the science of the atlas vertebra and its influence on conditions ranging from migraines and vertigo to post-concussion syndrome and fibromyalgia. Includes real patient case studies — several involving concussion recovery.
Ready to Find Out If We Can Help?
We offer complimentary consultations to learn more about you and determine whether upper cervical care is the right fit. There’s no pressure, no commitment — just an honest conversation about your symptoms, your history, and your options.
Schedule your complimentary consultation here: https://intake.chirohd.com/new-patient-scheduling/724/lavender-family-chiropractic
Or call us directly: (941) 243-3729
Lavender Family Chiropractic / NeckWise North Sarasota 📍 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 🌐 www.chiropractorsarasotaflorida.com 📱 Instagram: @lavenderfamilysrq 🎵 TikTok: @drrustylavender
Proudly serving Sarasota, Bradenton, Lakewood Ranch, Venice, Osprey, Port Charlotte, Parrish, and Palmetto — and helping patients across Southwest Florida finally heal at the root.
If you are in Tampa, Fort Myers, or Salt Lake City, you can visit our other NeckWise locations at www.neckwise.com. If you are not local to any of these, visit www.uccnearme.com to find a doctor in your area.
Your concussion does not have to define your life. Your symptoms do not have to be permanent. The fog can lift. The headaches can stop. The dizziness can fade. Let’s check your atlas — and see what becomes possible.
Disclaimer: Our office is out of network with insurance. Individual results vary. Upper cervical chiropractic care is not a substitute for emergency medical care. If you have suffered a recent head injury and are experiencing severe or worsening headache, repeated vomiting, seizures, slurred speech, unequal pupils, loss of consciousness, or new weakness/numbness on one side of the body, seek emergency care immediately.