Thoracic Outlet Syndrome: If you have been waking up with numb fingers, dropping your coffee cup because your grip feels weak, losing feeling in your arm when you lift it overhead, dealing with a constant ache between your shoulder blade and your collarbone, or watching one hand turn pale and cold while the other looks completely normal — you are not making it up, and you are not alone.
Thoracic outlet syndrome, often shortened to TOS, is one of the most missed, misdiagnosed, and mistreated conditions we see at our office. Patients come to us from every corner of the Suncoast carrying thick folders of nerve conduction studies, MRIs of the shoulder, EMGs of the arm, ultrasounds of the wrist, and a parade of diagnoses that never quite fit — carpal tunnel, tennis elbow, rotator cuff strain, “anxiety,” “just sleep on the other side.” Nothing explains the whole picture, and nothing makes the symptoms truly go away.
We see this every week, and there is almost always a pattern hiding underneath it. In the vast majority of TOS cases, the missing piece of the puzzle lives somewhere very few providers ever look — the top of the neck, where the atlas and axis vertebrae sit just below the skull, where the brainstem begins, and where every nerve and blood vessel that travels down into your arm starts its journey.
At Lavender Family Chiropractic, we are an upper cervical specialty office located at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243. Our team — Dr. Rusty Lavender and Dr. Jacob Temple — focuses on the precise, gentle correction of the atlas (C1) and axis (C2) vertebrae using 3D CBCT imaging and Tytron functional nervous system scans. We proudly serve patients throughout Sarasota, Bradenton, Lakewood Ranch, Venice, Osprey, Port Charlotte, Parrish, Palmetto, and the surrounding Gulf Coast communities.
This is the article we wish every TOS patient could read before another year goes by, before another surgery is scheduled, and before they are told one more time that nothing else can be done.
What Is Thoracic Outlet Syndrome?
The thoracic outlet is a real anatomical space, not a metaphor. It is the narrow passage between your collarbone and your first rib, on either side of your neck, where a bundle of critical structures has to squeeze through on their way from the spine and chest down into the arm. That bundle includes the brachial plexus — the cluster of nerves that controls the entire arm and hand — along with the subclavian artery and subclavian vein, which deliver blood to and from the arm.
When something compresses, irritates, or restricts this bundle as it passes through the thoracic outlet, you get thoracic outlet syndrome. The compression can be neurological, vascular, or both, and the symptoms reflect whatever is being pinched.
There are three classic types of TOS:
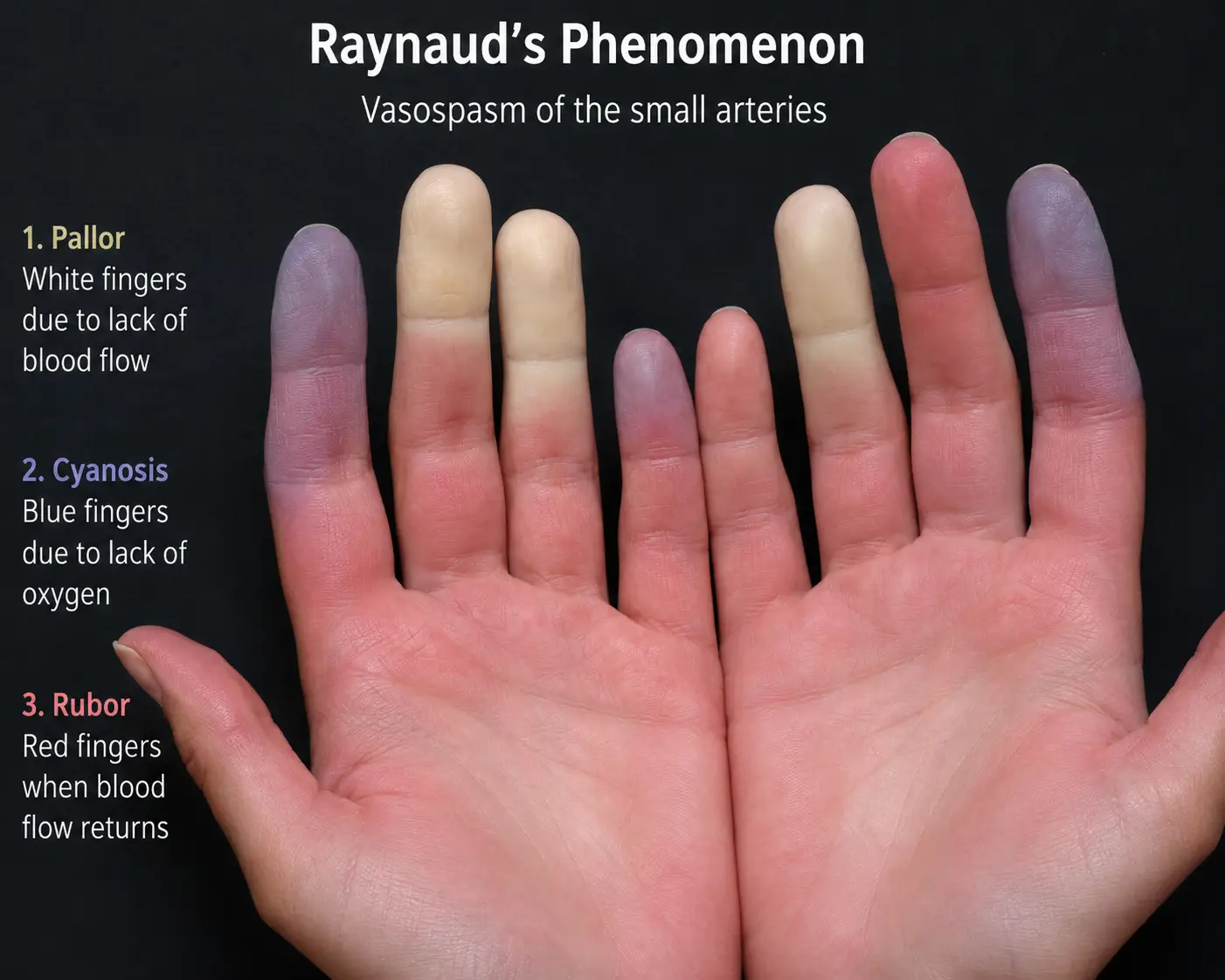
Neurogenic TOS is by far the most common, accounting for somewhere around 90 to 95 percent of cases. The brachial plexus is being compressed or irritated, and the symptoms are mostly nerve-related — numbness, tingling, weakness, burning, electric-shock sensations, hand fatigue, dropping things, difficulty with fine motor tasks like buttoning a shirt or typing, and a dull aching pain that often spreads from the side of the neck down through the shoulder, into the arm, and out into the fingers, especially the pinky and ring finger.
Venous TOS happens when the subclavian vein is compressed, and it tends to show up dramatically. The arm swells, turns blue or dusky, feels heavy, and the veins on the surface of the chest and shoulder may bulge. This is sometimes called effort thrombosis or Paget-Schroetter syndrome and often occurs in younger people who do a lot of overhead activity.
Arterial TOS is the rarest form. The subclavian artery is compressed or damaged, and the arm becomes pale, cold, painful with use, and weak. There may be a noticeable difference in pulse strength between the two wrists.
Most patients we see in Sarasota fall into the neurogenic category. They describe symptoms that are worse with arms overhead, worse at night, worse after long drives or long periods at a computer, worse when carrying a purse or backpack on the affected side, and worse during stretches of poor sleep or high stress. Many of them have already been worked up for carpal tunnel and either had surgery that did not fully resolve their symptoms or were told the nerve studies “looked normal” and there was nothing more to do.
That diagnostic dead end is exactly where we tend to enter the picture.
TOS Is a Nerve and Blood Vessel Condition — Not a Muscle Problem
One of the biggest mistakes in how thoracic outlet syndrome gets treated is the assumption that it is a muscle problem. Patients are told the scalenes are tight, the pec minor is short, the upper traps are overactive, and they are sent off with stretches, postural exercises, dry needling, and massage. Some of that helps in the short term — but it almost never resolves the underlying issue, because TOS is fundamentally a nerve and blood vessel issue, and the muscles that contribute to it are usually responding to a deeper signal coming from the upper cervical spine and brainstem.
To understand why, you have to look at three things at once: the nerves, the vessels, and the system that controls them.
The Brachial Plexus
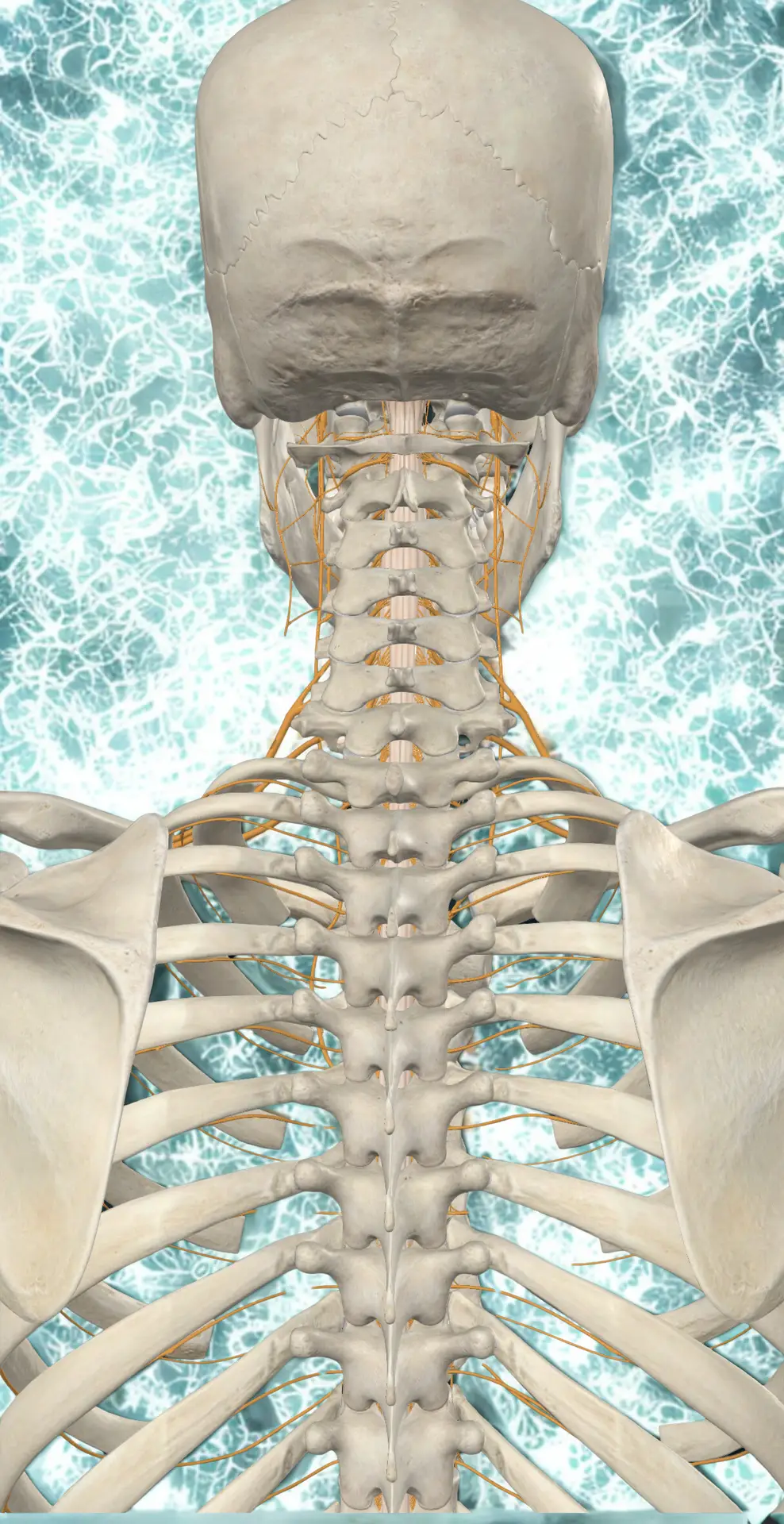
The brachial plexus is formed by nerve roots that exit the spine at C5, C6, C7, C8, and T1. These roots merge, divide, and reorganize into the nerves that supply the entire arm — the median nerve, ulnar nerve, radial nerve, axillary nerve, and musculocutaneous nerve. Anywhere along the path from the spinal cord to the fingertips, these nerves can be compressed, but the thoracic outlet is by far the most common bottleneck.
Crucially, every one of those nerve roots originates from a spinal cord that is suspended from and connected to the brainstem at the upper cervical junction. When the atlas or axis is misaligned, even by fractions of a degree, it can create mechanical tension on the dural membrane and the spinal cord itself, alter the resting tone of the cervical musculature, and feed abnormal signals down into the lower cervical and upper thoracic nerve roots that form the plexus. The result is a system primed for irritation long before the nerves ever reach the thoracic outlet.
The Subclavian Vessels
The arteries and veins that supply the arm pass over the first rib, under the collarbone, behind the pec minor, and through the same scalene gap as the brachial plexus. They are governed in part by the autonomic nervous system, particularly the sympathetic chain, which controls vessel diameter, blood flow, and temperature regulation. The sympathetic nerves that supply the upper extremity originate in the upper thoracic cord but are heavily influenced by signals coming from higher up, including the brainstem and the upper cervical region.
When upper cervical dysfunction disrupts autonomic balance, vessels in the arm can constrict or dilate inappropriately. Patients describe one hand always feeling colder, one arm getting “tingly” when they raise it, fingers that go pale or blotchy, and grip strength that fluctuates throughout the day. This is not just a “tight muscle” problem. This is a nervous system that has lost the ability to regulate the vascular and neural environment of the arm.
The Autonomic Nervous System
Behind it all, the autonomic nervous system — the part of your nervous system that runs every organ, every blood vessel, and every gland without your conscious input — is the conductor. The vagus nerve, the largest and most influential branch of the parasympathetic system, exits the skull right next to the atlas. The sympathetic chain runs alongside the entire cervical and thoracic spine. When the upper neck is misaligned, both branches of the autonomic system can be irritated. The result is sometimes called sympathetic dominance, and it shows up clinically as muscle tension that will not release, blood vessels that will not relax, sleep that does not restore, and a body that stays in a low-grade fight-or-flight state for years at a time.
That state is fertile ground for thoracic outlet syndrome to take root and stay rooted, no matter how many stretches you do. To learn more about how this kind of nervous system dysregulation drives a wide range of seemingly unrelated symptoms, see our deep dive on Dysautonomia and POTS in Sarasota.
The Upper Neck: Your Body’s Most Critical Junction
The upper cervical spine — the area where your skull meets your atlas, and your atlas meets your axis — is unlike any other part of the body. It carries an enormous amount of responsibility in a very small space.
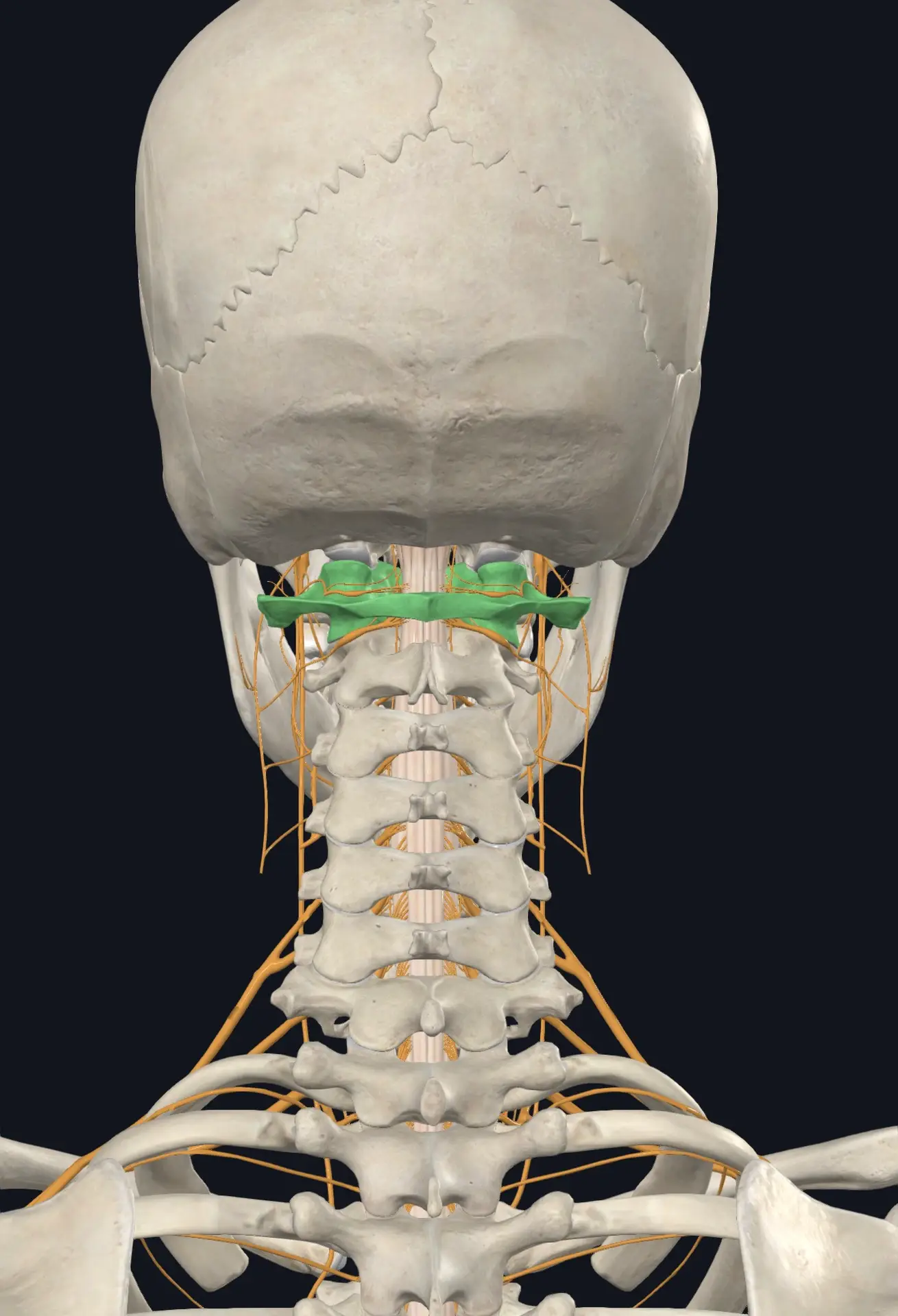
The atlas is the only vertebra in your body without a disc above or below it. It pivots around a peg-like projection from the axis called the dens, which is held in place by ligaments rather than bone. This design gives the head an extraordinary range of motion — about 50 percent of all rotation in the neck happens at this single joint — but it also makes the upper cervical area uniquely vulnerable to trauma, postural strain, and slow-developing misalignments.
Inside that joint, the brainstem sits in a protective sleeve. Cerebrospinal fluid flows around the spinal cord. The vertebral arteries thread up through small holes in the bone on their way to supply the back of the brain. The vagus nerve, glossopharyngeal nerve, and spinal accessory nerve all exit the skull within a finger’s width of the atlas. The dural membrane attaches in this region, anchoring the spinal cord to the skull and the upper neck.
When the atlas or axis loses its correct alignment — even by a millimeter or two — the whole architecture above and below it adapts. Shoulders may sit at different heights. One leg may functionally appear shorter. The thoracic spine may rotate. The first rib may elevate. The scalene muscles, which attach to the cervical spine and the first rib, may go into chronic guard. The pec minor may shorten. And right in the middle of all that, the thoracic outlet narrows.
This is why so many patients with TOS are also struggling with headaches, jaw tension, dizziness, ringing ears, GI issues, sleep problems, anxiety, and unexplained fatigue. None of it is coincidence. It is all the same system asking for help in different ways.
Why Traditional Care Often Misses This
Most providers who evaluate TOS focus exclusively on the local area — the scalenes, the first rib, the pec minor, the clavicle, the brachial plexus itself. They will perform Adson’s test, Roos test, Wright’s test, sometimes order an MR angiogram with the arms in different positions. Some of these patients will end up with a first rib resection or scalenectomy. A small percentage do well after surgery; many do not, and a meaningful number end up worse.
What is almost universally missed is the upper cervical assessment. We have lost count of how many patients have come into our office with a TOS diagnosis after years of treatment, and on imaging we find a clear, measurable atlas or axis misalignment driving postural compensations that pull the entire shoulder girdle into a TOS pattern. They have spent thousands on care that targeted everything but the source. Our Atlas Chiropractic page explains in detail how a single misaligned bone at the top of the neck can quietly drive symptoms throughout the entire body.
Upper Cervical Chiropractic Care: What Makes It Different
Upper cervical chiropractic is not the same as general chiropractic care. It is a specialty within the profession with its own training, its own imaging, and its own approach to correction.
The defining principle is precision. Rather than adjusting the entire spine in a session, an upper cervical chiropractor focuses on identifying and correcting the specific misalignment of the atlas or axis that is interfering with brainstem function and downstream nervous system regulation. The adjustment itself is typically gentle, low-force, and surgical in its accuracy. There is no twisting, popping, or cracking in the way most people picture chiropractic care.
At Lavender Family Chiropractic, we use 3D CBCT (cone-beam computed tomography) imaging to measure the position of the atlas and axis to within a fraction of a degree. We use Tytron infrared scanning to assess how the autonomic nervous system is functioning along the spine and to track changes over time. Together, these tools give us an objective, repeatable picture of what is happening at the most important junction in your body.
The correction itself is calculated specifically for your spine. Two patients with identical symptoms can have completely different misalignment patterns and require completely different vectors of correction. This is why the precision matters so much, and why people often travel hours to find a true upper cervical specialist.
When the atlas is restored to its correct position, the rest of the body begins a process of unwinding. The skull resettles. The shoulder girdle relaxes. The scalenes release without being forced. The first rib drops. The brachial plexus is no longer being asked to thread through a chronically constricted space. Vascular tone normalizes. Sleep deepens. The autonomic nervous system calms. And the body begins to heal in the order it needs to — not in the order we demand of it.
What to Expect at Lavender Family Chiropractic
Your first visit at our Sarasota office is a deep, careful evaluation. We sit down with you and listen — really listen — to your full story, including all of the providers you have seen, the treatments you have tried, the imaging you have already had, and the symptoms that have not yet been explained. We perform a thorough neurological, structural, and postural exam. If indicated, we capture our 3D CBCT scan to evaluate the upper cervical spine in three dimensions, and we perform a Tytron scan to assess autonomic function.
On your second visit, we sit back down and walk you through everything we found, in plain language, with the imaging on the screen so you can see it for yourself. We will tell you honestly whether we believe upper cervical care is a good fit for what you are dealing with. If it is, we will recommend a specific care plan. If it is not, we will refer you to someone who can help.
If you choose to begin care, the first adjustment is typically performed on that visit. The correction is gentle. Many patients describe it as feeling like a quiet click or pressure, nothing forceful. From there, your visits become shorter, more focused, and built around objective measurements that tell us when the atlas is holding and when it needs another correction. Our goal is always to need to adjust you as little as possible — because the longer your correction holds, the more your nervous system is restoring itself.
Our NeckWise North Sarasota page walks through the full step-by-step process so you know exactly what to expect from your very first phone call to your first adjustment.
Ready to find out if upper cervical care is the missing piece of your TOS story? Schedule your new patient evaluation here: https://intake.chirohd.com/new-patient-scheduling/724/lavender-family-chiropractic
Evidence and Emerging Research
Upper cervical chiropractic is sometimes painted as alternative or fringe, but the underlying anatomy and the body of supporting research are increasingly hard to ignore.
The connection between upper cervical alignment, brainstem function, and autonomic regulation has been studied in the context of post-concussion syndrome, cervicogenic headaches, hypertension, vertigo, and a variety of nerve-driven conditions. Research published in journals such as the Journal of Human Hypertension, the Journal of Upper Cervical Chiropractic Research, and various neurology publications has pointed to measurable changes in blood flow, cerebrospinal fluid dynamics, and autonomic balance after precise upper cervical correction.
In the context of thoracic outlet syndrome specifically, a growing body of literature recognizes the role of cervical spine dysfunction in driving compensatory patterns of the scalenes, first rib, and shoulder girdle. Studies on whiplash and post-traumatic neck injury patients show a high coexistence of TOS-type symptoms, and clinicians who manage these cases consistently find better outcomes when the cervical spine is addressed as part of the picture rather than ignored.
The vagus nerve and autonomic nervous system have become an enormous area of research in the last decade, and the upper cervical region — where the vagus exits the skull and where the sympathetic chain originates — is increasingly recognized as a clinically meaningful structure to assess and address. Patients who have struggled with TOS, dysautonomia, POTS, chronic fatigue, and other related conditions often share a common denominator at the top of the neck, and our experience in Sarasota mirrors what the broader research community is beginning to confirm.
We do not promise that every patient with TOS will fully resolve their symptoms with upper cervical care. We do believe that any honest, thorough TOS workup should include an evaluation of the upper cervical spine — and right now, in most parts of the country, that evaluation is rarely happening.
Lifestyle Factors That Complement Upper Cervical Care
Care does not stop at the adjustment. We coach our TOS patients on a number of lifestyle factors that support the work being done in the office. These are simple, inexpensive, and remarkably effective when stacked together.
Sleep position. Side sleeping with the affected arm under the head or pillow is one of the most common aggravators of TOS we see. Many patients begin to improve dramatically just by switching to back sleeping with a properly contoured pillow and arms supported at the sides.
Posture and workstation setup. Most modern jobs put the head forward and shoulders rolled in for hours at a time. A keyboard at the right height, a screen at eye level, frequent postural breaks, and time spent walking with the arms relaxed at the sides go a long way.
Breathing. Most TOS patients are chest breathers, using the scalenes and accessory muscles of the neck to draw air in instead of using the diaphragm. This is exhausting for the very muscles that should be quiet, and it perpetuates the compression in the thoracic outlet. Diaphragmatic breathing practice, even for a few minutes a day, can be transformative.
Bag and load habits. Heavy purses, briefcases, gym bags, or backpacks on a single shoulder pull the shoulder girdle down on one side and grind through the thoracic outlet for hours at a time. We routinely have patients change to a small crossbody, a rolling bag, or a properly fitted two-strap backpack and watch their symptoms improve within weeks.
Stress and the autonomic system. Chronic stress keeps the sympathetic nervous system on overdrive, which keeps muscles tight and vessels constricted. Walking, sunlight, time in nature, and consistent sleep are not luxuries — they are part of the treatment.
Hydration and inflammation. Dehydrated tissues are stickier, less mobile, and more prone to nerve irritation. A consistent hydration habit and an anti-inflammatory diet quietly support nerve recovery in the background.
For patients whose TOS symptoms overlap with chronic neck pain, postural strain, or old whiplash injuries, our blog on Why Does My Neck Hurt? walks through the same upper cervical principles in a different but very related context.
Serving Sarasota and the Surrounding Gulf Coast
Our office sits in North Sarasota at the corner of University and Whitfield, just off Route 41, which makes us easy to reach from a wide stretch of the Suncoast. We see TOS patients from many of the surrounding neighborhoods and communities, including:
Downtown Sarasota, Southside Village, Arlington Park, Gillespie Park, Ringling Park, Bayou Oaks, Rosemary District, Indian Beach, Sapphire Shores, Whitfield Estates, Desoto Lakes, University Park, The Meadows, Palmer Ranch, Bee Ridge, Gulf Gate, Siesta Key, Lido Key, Longboat Key, Casey Key, Osprey, Nokomis, Venice, Wellen Park, North Port, Englewood, Port Charlotte, Punta Gorda, Lakewood Ranch, Greenbrook, Country Club East, Esplanade, Heritage Harbour, Bradenton, West Bradenton, Anna Maria Island, Holmes Beach, Cortez, Palmetto, Ellenton, Parrish, Terra Ceia, and beyond.
For a complete list of the cities and neighborhoods we serve, visit our Areas We Service page.
If you have been driving from one specialist to another up and down I-75 with no real answers for your numbness, tingling, or arm weakness, you are far from the first person to make that drive — and we are honored to be the office where so many of these stories finally start to turn around.
Is Upper Cervical Care Right for You?
If you have been diagnosed with thoracic outlet syndrome and traditional treatment has not given you the relief you hoped for, you owe it to yourself to have your upper cervical spine evaluated by a true specialist. If you have not been formally diagnosed with TOS but recognize yourself in the symptoms described in this article — the numbness, the tingling, the cold hand, the heavy arm, the grip that comes and goes, the pain that no provider can quite name — the same is true.
You do not have to live the rest of your life avoiding overhead work, dropping your phone, sleeping with your arm on a pillow tower, or wondering if surgery is the only thing left. There is another path, and it begins with looking in the place almost no one has looked yet.
To schedule a new patient evaluation at Lavender Family Chiropractic in Sarasota, call us at (941) 243-3729 or book online directly at:
https://intake.chirohd.com/new-patient-scheduling/724/lavender-family-chiropractic
We will take the time to listen to your full story, complete a thorough exam, image your upper cervical spine in three dimensions, scan your nervous system, and give you a clear, honest answer about whether we can help. If we cannot, we will tell you so and point you toward who can.
Thoracic outlet syndrome is not a life sentence. It is a signal that your nervous system needs help. We would be honored to help you listen to it.
Related Articles
If this article resonated with you, the following posts from our blog go deeper into the same nervous system principles in related conditions:
- Can Neck Pain Cause Headaches? Understanding the Atlas Connection — A close look at how upper cervical misalignment drives headaches, neck pain, and the same kind of nerve irritation patterns we see with TOS.
- Occipital Neuralgia: Proven Lasting Relief Through Atlas Alignment — How precise upper cervical correction addresses nerve-driven pain that radiates from the base of the skull, with strong overlap to nerve compression patterns in the upper extremity.
- Alternative Doctor for Vertigo in Sarasota and Manatee County — How upper cervical care addresses the dizziness, balance, and autonomic patterns that so often travel with TOS.
This blog is for informational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider for diagnosis and treatment of any health condition. Lavender Family Chiropractic | 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 | (941) 243-3729