Natural Migraine Treatment: If you’re reading this, there’s a good chance you’ve already tried almost everything. The prescription preventives that left you foggy, exhausted, or 15 pounds heavier. The abortive medications that worked for a while and then stopped. The dark rooms, ice packs, elimination diets, magnesium, riboflavin, Botox injections, nerve blocks, even the new CGRP biologics. You’ve kept a trigger journal. You’ve cut the wine, the chocolate, the aged cheese, the gluten.
You’ve done acupuncture, massage, and physical therapy. And still — the migraines come. They come on flights. They come with the weather changes that roll across Sarasota Bay every afternoon. They come the morning after you finally had a stressful week behind you. They come for no reason at all.
At Lavender Family Chiropractic, located at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243, we see migraine sufferers from across Sarasota, Bradenton, Lakewood Ranch, Venice, Osprey, Parrish, and Palmetto every single week — people who have been told by neurologists that they’ve reached the ceiling of what modern medicine can offer them, and that they should learn to “manage” their condition for the rest of their lives. We don’t accept that as a final answer.
Drs. Rusty Lavender and Jacob Temple have built this practice specifically around one of the most consistently overlooked drivers of chronic migraine: a misalignment of the top two bones of the neck, the atlas (C1) and axis (C2). When this junction is off — even by a fraction of a millimeter — it can disrupt nerve signaling, alter blood flow to the brain, impair cerebrospinal fluid drainage, and create the exact neurovascular instability that defines the migraine state.
What Is a Migraine, Really? Natural Migraine Treatment
A migraine is not a bad headache. That single misunderstanding may be the most damaging myth in all of headache medicine, because it has trained millions of patients — and a fair number of their doctors — to think of migraine as something that can be solved with a stronger pain pill. It can’t. Migraine is a complex, episodic neurological disorder that involves the entire central nervous system, the cerebral vasculature, the autonomic nervous system, and the trigeminal pain pathways. The head pain is just the loudest symptom in a much broader storm.
A typical migraine attack moves through four phases, although not every patient experiences every phase in every attack. The prodrome, which can begin hours or even a day or two before the pain, includes neck stiffness, food cravings, irritability, frequent yawning, increased urination, and a feeling that something is “off.” The aura, experienced by roughly 25 percent of migraineurs, involves transient neurological symptoms such as flashing lights, zigzag lines, blind spots, tingling in a hand or face, or difficulty finding words.
The headache phase itself is the throbbing, pulsing, often one-sided pain that can last from four to 72 hours and is typically accompanied by nausea, vomiting, light sensitivity (photophobia), sound sensitivity (phonophobia), and sometimes vertigo. The postdrome — the “migraine hangover” — leaves patients depleted, foggy, and slow for a day or more after the pain resolves.
The World Health Organization ranks migraine among the top twenty most disabling conditions in the world. About 12 percent of adults in the United States meet diagnostic criteria for migraine, with women affected roughly three times as often as men. Chronic migraine — defined as fifteen or more headache days per month for at least three months — affects 1 to 2 percent of the population and is one of the leading global causes of disability in people under fifty. Migraine costs the US economy an estimated 36 billion dollars per year in healthcare expenses and lost productivity. Behind those numbers are millions of people whose careers, relationships, and quality of life are quietly being eroded by a condition that mainstream medicine still does not fully understand.
Migraine Is a Nerve and Vascular Condition
To understand why upper cervical chiropractic care can be so effective for migraine, you have to understand what is actually happening inside the head during an attack. Migraine is a neurovascular condition, meaning it involves both the nerves and the blood vessels of the brain — and the two systems are inextricably linked.
The Trigeminovascular System
The central player in migraine generation is the trigeminovascular system. The trigeminal nerve, the largest of the cranial nerves, supplies sensation to the face, scalp, and the dura mater — the tough membrane that wraps around the brain. When the trigeminal nerve becomes hyperactive, it releases inflammatory neuropeptides like CGRP (calcitonin gene-related peptide), substance P, and neurokinin A. These chemicals dilate blood vessels in the meninges, produce sterile inflammation, and sensitize pain receptors. The result is the pounding, pulsating pain that migraine sufferers know all too well.
This trigeminovascular cascade is why the newest class of migraine drugs — the CGRP antagonists — works the way it does: it interrupts one piece of the chemical storm. It does not, however, explain whythat storm starts in the first place.
Brainstem Dysfunction and Central Sensitization
A growing body of evidence points to the brainstem — specifically structures like the periaqueductal gray, the locus coeruleus, and the trigeminal nucleus caudalis — as the “migraine generator.” These regions sit immediately below the upper cervical spine and modulate pain processing, autonomic function, and sensory gating. When the brainstem is irritated or its signaling becomes dysregulated, the entire system becomes hypersensitive. Light feels too bright. Sound feels too loud. Smells become nauseating. Pain pathways that should be filtered out instead fire freely. This is called central sensitization, and it is one of the reasons chronic migraineurs become more sensitive to triggers over time rather than less.
Cerebrospinal Fluid and Intracranial Pressure
Cerebrospinal fluid (CSF) cushions the brain and spinal cord, delivers nutrients, and clears metabolic waste — including waste products implicated in headache and inflammation. CSF moves in a rhythmic, dynamic pattern, and its drainage out of the skull depends critically on the patency of the craniocervical junction. When the atlas and axis are misaligned, the small openings through which CSF and venous blood exit the cranium can become partially restricted. The result is reduced intracranial compliance — a measurable, MRI-documented change that has been directly linked to migraine in published research, which we’ll come back to later in this article.
Cervical Afferent Input and Neck-Headache Convergence
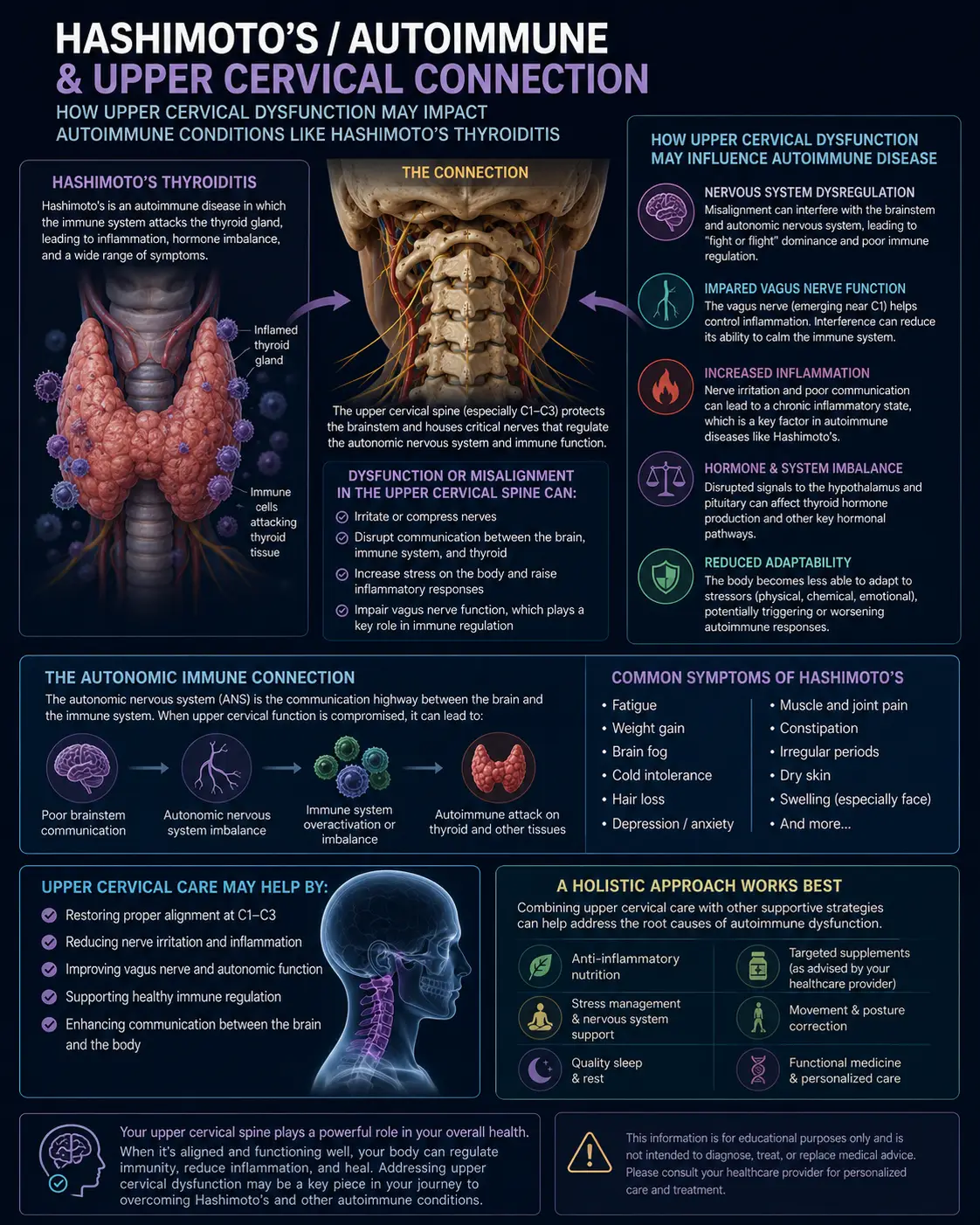
Here is one of the most important — and least appreciated — facts in headache medicine: the sensory nerves from the upper three cervical vertebrae (C1, C2, C3) converge with the trigeminal nerve in a region of the brainstem called the trigeminocervical nucleus. This convergence means that signals coming from the upper neck and signals coming from the face and head essentially share the same neurological “wiring.”
A dysfunctional upper neck can fire abnormal signals into the trigeminocervical nucleus and produce pain that is felt in the head — even when there’s nothing wrong with the head itself. Studies have repeatedly demonstrated that migraine patients have significantly more cervical musculoskeletal dysfunction than non-migraine controls, and that the upper cervical spine can be a primary driver of migraine attacks in a substantial percentage of patients.
The Upper Neck: Your Body’s Most Critical Junction
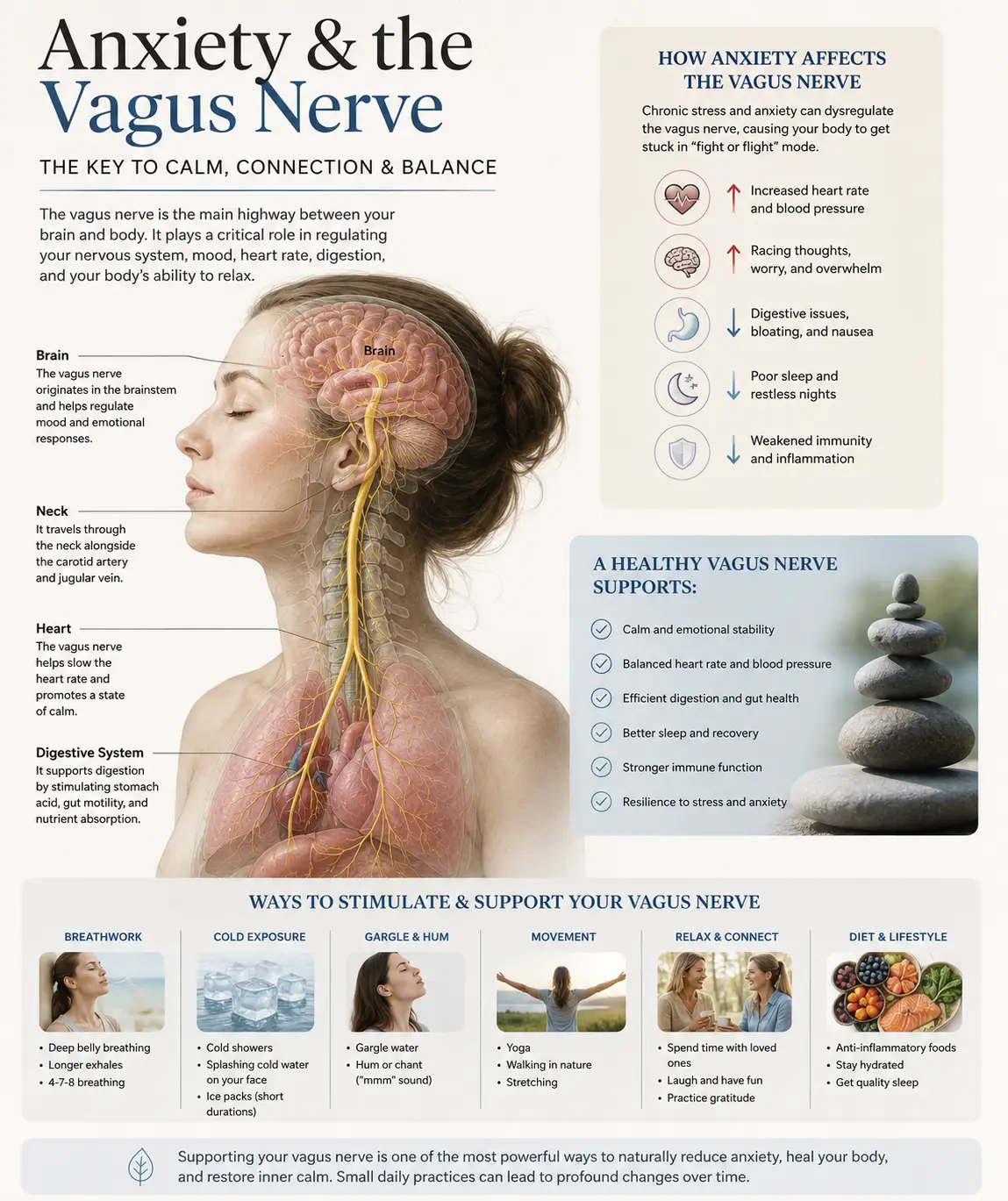
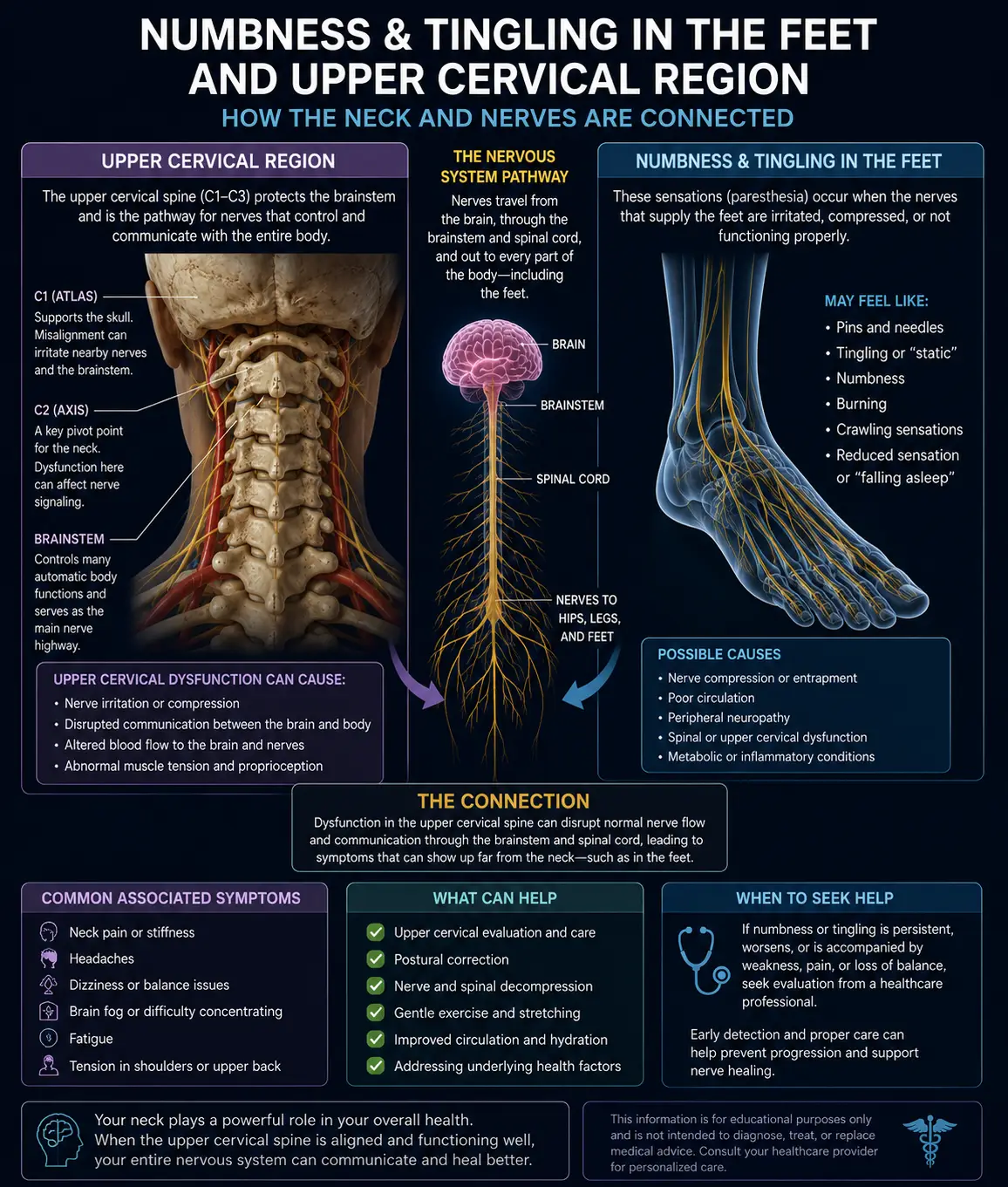
The atlas (C1) and axis (C2) are unlike any other bones in the spine. The atlas is a ring of bone that holds the weight of the entire head — roughly 10 to 12 pounds — on two small joint surfaces. It has no disc above or below it. It is held in place largely by ligaments, and it is the most mobile vertebra in the spine. Sitting directly beneath the skull, the atlas surrounds and protects the lower brainstem, the vertebral arteries that supply the back of the brain, and the foramen magnum — the large opening through which the spinal cord exits the skull.
When the atlas is in its proper position, the head is centered over the neck, the brainstem is unrestricted, the vertebral arteries flow freely, CSF circulates without obstruction, and the upper cervical nerves transmit clean sensory information back to the brain. When the atlas shifts even slightly out of alignment — which can happen from car accidents, sports injuries, falls onto the head or tailbone, the birthing process, prolonged forward head posture, or repeated minor traumas — every one of those systems can be subtly compromised.
The body responds with compensations: head tilt, shoulder elevation, hip rotation, postural muscle spasm, and increased tension throughout the suboccipital region. Over months and years, these compensations create the perfect physiological terrain for chronic migraine.
Why Traditional Care Often Misses This
The upper cervical spine sits in a diagnostic blind spot for most of conventional medicine. A standard cervical MRI is excellent at identifying disc herniations, tumors, and gross structural abnormalities — but it is typically interpreted while you are lying flat and still, in a position that masks the subtle rotational and lateral misalignments that drive symptoms. Standard X-rays don’t capture the three-dimensional relationships between the atlas, the skull, and the axis. Neurologists are trained to look for tumors, strokes, and demyelinating disease, not biomechanical asymmetries of the C1-C2 complex. Even most chiropractors do not focus on this region with the precision required to address it correctly — they perform general spinal manipulation, which is a completely different discipline from upper cervical specific care.
This diagnostic blind spot is why so many migraine patients spend years cycling through specialists, accumulating “unremarkable” imaging reports, and being told their migraines are simply “idiopathic” — a fancy medical word that essentially means we don’t know. Meanwhile, the answer is sitting two inches above their shoulders, hidden in a region that almost nobody is trained to evaluate properly.
Upper Cervical Chiropractic Care: What Makes It Different
Upper cervical chiropractic is a sub-specialty within the chiropractic profession. It does not involve twisting the neck, popping or cracking, or general spinal manipulation. Instead, it is a precision-based discipline focused exclusively on correcting misalignments of the atlas and axis, using imaging-guided, low-force techniques that are gentle enough for infants and elderly patients alike. The premise is simple but powerful: if you correct the structural problem at the most neurologically critical junction in the entire spine, the body’s own healing systems can begin to resolve the cascading dysfunctions downstream — including chronic migraine.
At Lavender Family Chiropractic, we use 3D Cone Beam Computed Tomography (CBCT) imaging to create a precise, three-dimensional map of each patient’s atlas and axis. This is the same technology used in advanced dental and ENT imaging, and it allows us to measure misalignment in millimeters and fractions of a degree — far beyond what standard X-rays can show.
We pair this with Tytron functional nervous system scanning, which uses paraspinal infrared thermography to detect asymmetries in autonomic nervous system output. Together, these tools give us an objective, repeatable picture of both the structural problem and the neurological consequences of that problem. Adjustments are then customized to the individual patient’s measurements and delivered without any forceful twisting, popping, or cracking.
What to Expect at Lavender Family Chiropractic
Your first visit is a comprehensive consultation and examination. We spend time understanding your migraine history — the patterns, the triggers, the past treatments, the trauma history that other providers may have skipped right past. We perform a thorough neurological and postural exam. If we believe you are a candidate for upper cervical care, we proceed to CBCT imaging and Tytron scanning.
We then sit down with you, walk you through your scans, and explain — in plain language — exactly what we are seeing and why we believe it is relevant to your migraine pattern. There are no contracts, no high-pressure sales pitches, and no commitments before we have looked at your data and you have looked at it with us. You can read more about the new patient experience at our office on our What to Expect page, which walks through every step in detail.
The corrective adjustment itself is remarkably gentle. Patients are often surprised at how little force is required. After the adjustment, we have you rest for a short period to allow the nervous system to begin integrating the change. Most patients describe an immediate sense of relaxation, a softening of the chronic neck tension they have been carrying, and a feeling of being more “settled” in their body. The deeper changes — reduced migraine frequency, less intensity, fewer prodromal warning signs — typically unfold over a series of visits as the body holds the correction more reliably and the nervous system recalibrates. To learn more about the specific technique and philosophy that guides our work, visit our page on Upper Cervical Chiropractic Care.
Ready to find out if upper cervical care can help with your migraines? Schedule Your Free Consultation Here — or call our Sarasota office directly at (941) 243-3729. We see patients from all across the Gulf Coast and would be honored to help you find the relief you’ve been searching for.
Evidence and Emerging Research
Skepticism is healthy. If a treatment is going to ask you to invest your time, money, and hope, you have every right to expect evidence behind it. The body of research supporting upper cervical chiropractic care for migraine is growing, and while it is not yet at the scale of pharmaceutical research, the findings have been remarkably consistent.
The most cited piece of research in this area is the Effect of Atlas Vertebrae Realignment in Subjects with Migraine observational pilot study, published in BioMed Research International and indexed at the National Library of Medicine. This study followed eleven neurologist-diagnosed migraine patients who received NUCCA (National Upper Cervical Chiropractic Association) atlas corrections over an eight-week period. Researchers used pre- and post-treatment MRI imaging to measure changes in intracranial compliance — essentially, how well the brain can accommodate normal pressure fluctuations.
The results showed measurable improvement in intracranial compliance alongside significant reductions in headache symptoms and meaningful gains in migraine-specific quality of life measures. This was the first study to demonstrate, with objective MRI evidence, that correcting atlas alignment produces a measurable change in the physical environment of the brain — and that this change correlates with symptom relief. The full study is publicly accessible through the National Institutes of Health PubMed Central database.
A 2017 study by Luedtke and May, published in The Journal of Headache and Pain, examined dynamic pain provocation over the upper cervical spine in migraine patients and concluded that neck pain in migraine “is not simply a symptom of the migraine attack but corresponds to identifiable muscle and joint alterations.” The researchers proposed stratifying migraine patients based on their upper cervical findings, recognizing that a substantial subset of migraine sufferers have a cervical contribution to their condition that is not being addressed by standard pharmaceutical management.
A 2024 observational study published in Frontiers in Neurology compared cervical impairments between migraine patients, tension-type headache patients, and healthy controls. The migraine group demonstrated significantly altered deep cervical muscle thickness, greater local and widespread pain sensitivity, and reduced cervical functionality compared to controls. The authors concluded that cervical dysfunction is a measurable and clinically relevant feature of migraine — not a coincidence, and not a downstream effect of headache, but a contributing component of the disorder itself.
Most recently, a 2025 systematic and critical review published in the Asia Pacific Chiropractic Journal analyzed seven eligible trials covering 453 participants and concluded that chiropractic manipulation, including the precise low-force adjustments used in upper cervical care, may be an effective intervention for migraine management. The review specifically noted that the chiropractic approach offers an option for migraine patients seeking alternatives to long-term pharmaceutical management — particularly those who have not responded adequately to standard preventive medications.
Taken together, these studies — along with hundreds of case reports in the chiropractic literature — paint a coherent picture. Upper cervical misalignment is a real, measurable, and clinically meaningful contributor to migraine in a significant subset of patients, and precise correction of that misalignment produces both objective physiological changes and subjective symptom relief.
Lifestyle Factors That Complement Upper Cervical Care
Upper cervical chiropractic care is powerful, but it is not magic. Your body’s response to structural correction is influenced by everything else you do to support your nervous system — and patients who combine upper cervical care with intelligent lifestyle changes tend to see the most dramatic, lasting results. Here are the lifestyle factors we encourage every migraine patient at our Sarasota office to consider.
Hydration. The brain is roughly 75 percent water, and even mild dehydration is a powerful migraine trigger. In our Florida climate — especially during the summer months when the humidity is brutal and people are losing more fluid than they realize — chronic low-grade dehydration is rampant. Aim for at least half your body weight in ounces of water daily, and add electrolytes if you sweat heavily.
Sleep regularity. The migraine brain is exquisitely sensitive to changes in sleep schedule. Going to bed at midnight on Friday and 9 PM on Sunday is enough to trigger an attack in many patients. Aim for consistent sleep and wake times — even on weekends.
Magnesium. Multiple studies have shown that magnesium glycinate or magnesium threonate (300–500 mg per day) can reduce migraine frequency, particularly in patients with menstrual migraine or aura. It is one of the few supplements with reasonable evidence behind it.
Blood sugar stability. Skipping meals, crashing on caffeine, and high-glycemic snacks all create blood sugar swings that the migraine brain reads as a threat. Build meals around protein, healthy fats, and fiber, and avoid going more than four to five hours without eating.
Stress regulation. The autonomic nervous system — which is profoundly influenced by upper cervical alignment — is also profoundly influenced by your stress habits. Daily breathwork, gentle yoga, walking outdoors, time off screens, and dedicated decompression time all support the same regulatory systems that upper cervical care addresses structurally.
Posture and screen ergonomics. Forward head posture loads the upper cervical spine with up to 60 pounds of effective weight. Setting up your workstation so your screen is at eye level, taking frequent breaks, and being mindful of your “tech neck” habits will protect the correction you receive in our office.
For a deeper dive into the broader migraine picture — including detailed sections on trauma history, specific imaging findings, and the role of CBCT-guided adjustments — we recommend reading our comprehensive companion article, Best Migraine Treatment in Lakewood Ranch, Florida: Proven Results With This Natural Approach. It is the most thorough resource we have published on migraine and pairs perfectly with what you have just read.
Serving Sarasota and the Surrounding Gulf Coast
Lavender Family Chiropractic is located at the corner of University and Whitfield in North Sarasota, just minutes from the SRQ airport, the University Town Center, and easy access from I-75. Our address is 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243. We are proud to serve migraine patients from across the Gulf Coast, including:
- Sarasota — downtown, Bird Key, Lido Key, Siesta Key, Palmer Ranch, Gulf Gate, and all surrounding neighborhoods
- Bradenton — including West Bradenton, East Bradenton, and the Cortez corridor
- Lakewood Ranch — including Country Club East, Greenbrook, and Heritage Harbour
- Venice — including Nokomis, Laurel, and surrounding communities
- Osprey and Casey Key
- Parrish and Palmetto — including the rapidly growing North River and Ellenton communities
- Port Charlotte, Punta Gorda, and North Port
- Anna Maria Island, Longboat Key, and Holmes Beach
- Myakka City and surrounding rural Manatee County
Many of our patients drive in from St. Petersburg, Tampa, Fort Myers, and even further for specialty upper cervical care. We understand that severe migraine sufferers are willing to travel for relief — and we work to make our care worth every mile. You can view a complete list of the communities we serve on our Areas We Service page.
If you are wondering whether your migraine pattern is one we can help with — or whether upper cervical care is the right approach for your particular situation — we encourage you to learn more about our philosophy on our Why Upper Cervical page, which explains in depth why we have built our practice around this specific niche.
Top 15 Frequently Asked Questions About Upper Cervical Care for Migraines
1. How is upper cervical chiropractic care different from regular chiropractic?
Regular chiropractic typically involves manipulation of multiple regions of the spine, often using rotational, high-velocity, low-amplitude thrusts that produce the audible “pop.” Upper cervical chiropractic, by contrast, focuses exclusively on the precise correction of the atlas (C1) and axis (C2) using imaging-guided, low-force techniques. There is no twisting, no popping, and no general manipulation. It is a specialty discipline that requires extensive additional training and specific diagnostic technology.
2. Is upper cervical care safe?
Yes. The techniques used in upper cervical care are among the gentlest interventions in all of musculoskeletal medicine. Because we use 3D CBCT imaging to plan each correction and because the adjustments themselves involve very little force, the procedure is appropriate for patients of all ages — from infants to adults in their 80s and 90s.
3. How quickly will I see results?
Every patient is different. Some patients feel a significant change within days of their first correction. Others — particularly those with long-standing chronic migraine — see results gradually unfold over several weeks to a few months as the body holds the correction more reliably. We monitor your progress with both subjective symptom tracking and objective re-scanning.
4. Will I have to come forever?
No. The goal of upper cervical care is to correct the underlying structural problem and have your body hold that correction independently. Most patients move from an initial corrective phase into a much less frequent maintenance phase as their body stabilizes. We do not believe in “forever” care plans.
5. Do you take insurance?
We do not bill insurance directly for our specialty care, but we provide detailed receipts that many patients submit for out-of-network reimbursement or HSA/FSA use. Our team can explain the financial side in detail during your initial consultation.
6. Is it covered by Medicare?
We are not Medicare participating providers for our upper cervical specialty care. We can discuss the specifics during your consultation so there are no surprises.
7. Will it hurt?
No. The corrections themselves are gentle and painless. Some patients experience mild soreness in the day or two after their first correction as the body begins to unwind compensations — similar to what you might feel after starting a new exercise program — but this is typically very minor and short-lived.
8. Can I still take my migraine medications?
Absolutely. Upper cervical care works alongside whatever medications you are currently using. As your body responds and your migraines improve, many patients work with their prescribing physicians to gradually reduce or eliminate medications — but that is always a decision made between you and your medical doctor, not something we manage directly.
9. What if I’ve had neck surgery or have a serious spinal condition?
Patients with prior cervical surgery, severe osteoporosis, rheumatoid arthritis, or other significant spinal conditions can still often be candidates for upper cervical care — but we evaluate each case individually using imaging and a detailed medical history before recommending any treatment.
10. Can children get migraines, and can you help them?
Yes to both. Pediatric migraine is more common than most parents realize, and the gentleness of upper cervical care makes it particularly well-suited for children. Many pediatric migraine patterns are linked to birth trauma, falls, or sports injuries — all of which can affect the upper cervical spine.
11. I have vestibular migraine. Can upper cervical care help with the dizziness too?
Often, yes. Because the upper cervical spine has a direct neurological relationship with the vestibular system, balance, and proprioception, vestibular migraine patients frequently see improvements in both the headache and the dizziness components of their condition with upper cervical care.
12. What about hormonal or menstrual migraines?
Hormonal fluctuation is a powerful migraine trigger, but it is a trigger acting on an already sensitized nervous system. Upper cervical care reduces that underlying sensitivity, which often translates into fewer and less severe menstrual migraine attacks even though we are not directly addressing hormones.
13. How do I know if my migraines are coming from my upper neck?
The honest answer is that we cannot know with certainty until we examine you and image your upper cervical spine. That said, common clues include a history of head or neck trauma, migraines that worsen with neck movement, prominent neck pain or stiffness before or during attacks, one-sided symptoms, and a lack of meaningful response to standard migraine medications.
14. What if I’ve never had a neck injury that I can remember?
Many upper cervical misalignments come from events the patient does not remember or never identified as significant — childhood falls, sports injuries, the birth process itself, repeated minor whiplash from sudden braking, sleeping in awkward positions on planes or couches, or simply years of forward head posture. Trauma history is helpful but not required for diagnosis.
15. How do I get started?
The simplest step is to schedule a complimentary consultation either online at our scheduling link or by calling our Sarasota office at (941) 243-3729. We will listen to your story, answer your questions, and help you determine whether upper cervical care is a reasonable next step for your specific situation — with no pressure and no obligation.
You Don’t Have to Live This Way
The most painful thing about chronic migraine is not the pain itself — it is the loss. The vacations canceled. The birthday parties endured rather than enjoyed. The work projects you could have crushed if you weren’t terrified the next attack was three hours away. The quiet, slow erosion of a life you used to take for granted. We have sat across from hundreds of migraine patients in our Sarasota office who looked at us with the same exhausted expression — somewhere between hope and self-protection — wondering if this could possibly be the thing that finally helps.
It often is. Not because upper cervical chiropractic is a miracle, but because the upper cervical spine is genuinely, mechanically, neurologically central to the migraine equation — and almost nobody else is looking at it the way we look at it. Drs. Rusty Lavender and Jacob Temple have built this practice for one reason: because the patients who walk through our doors deserve a real shot at the kind of relief that addresses the root cause of their condition, not just another prescription pad and another instruction to “manage” it for the rest of their lives.
If you are ready to take that step, we would be honored to walk it with you.
Schedule Your Free Consultation | Call us directly: (941) 243-3729 | Visit us at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243
Related Articles from Our Blog
Best Migraine Treatment in Lakewood Ranch, Florida: Proven Results With This Natural Approach Our most comprehensive resource on migraine and upper cervical care. This deep-dive article covers the full migraine landscape — types, triggers, trauma history, CBCT imaging, the knee-chest technique, and detailed FAQ — and pairs perfectly with the article you just read.
Vestibular Migraines and Upper Cervical Care: A Comprehensive Guide to Relief If your migraine attacks include vertigo, dizziness, or balance disturbances, this article is essential reading. We explore the neurological overlap between the migraine pathway and the vestibular system — and why upper cervical correction so often helps both components simultaneously.
Top 15 FAQs About Barometric Headaches and Migraines in Bradenton, Florida Living on Florida’s Gulf Coast means living with constant atmospheric pressure shifts. This blog explains why weather-triggered migraines are so common here, how upper cervical alignment changes your sensitivity to barometric changes, and what you can do beyond chiropractic care to reduce weather-driven attacks.
This blog is for informational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider for diagnosis and treatment of any health condition. Lavender Family Chiropractic | 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 | (941) 243-3729