Types of Vertigo: If you’ve ever stood up from bed and felt the room lurch sideways, or turned your head in the grocery store and suddenly grabbed for a shelf to stay upright, you already know that “vertigo” is too small a word for what’s actually happening. Vertigo isn’t one condition. It’s an entire family of conditions that share one frustrating symptom — the false sensation of movement — but have very different causes, very different patterns, and very different paths to relief.
Here in Sarasota, we see vertigo patients every single week at our office at 5899 Whitfield Avenue, right at the corner of University and Whitfield. They come from Sarasota, Lakewood Ranch, Bradenton, Osprey, Venice, and Parrish. They come after months — sometimes years — of being told it’s “just BPPV” or “just anxiety” or “just getting older.” And in nearly every case, the first real breakthrough comes from the same thing: actually understanding which kind of vertigo they’re dealing with.
This blog is the in-depth companion piece to our main resource, Vertigo Doctor Sarasota: Proven Relief with Upper Cervical Chiropractic at Lavender Family Chiropractic. If you haven’t read that one yet, start there for the overview of how we approach vertigo as a whole. This guide goes deeper into the specific types — what they feel like, what causes them, what the research says, and how upper cervical chiropractic fits into each picture.
What Is Vertigo, Really? Types of Vertigo
Vertigo is the false perception of motion. You feel like you or the world around you is spinning, tilting, swaying, or rocking — but nothing is actually moving. That’s the defining feature. It’s different from lightheadedness (feeling faint), and it’s different from disequilibrium (feeling unsteady on your feet). True vertigo has motion built into it.
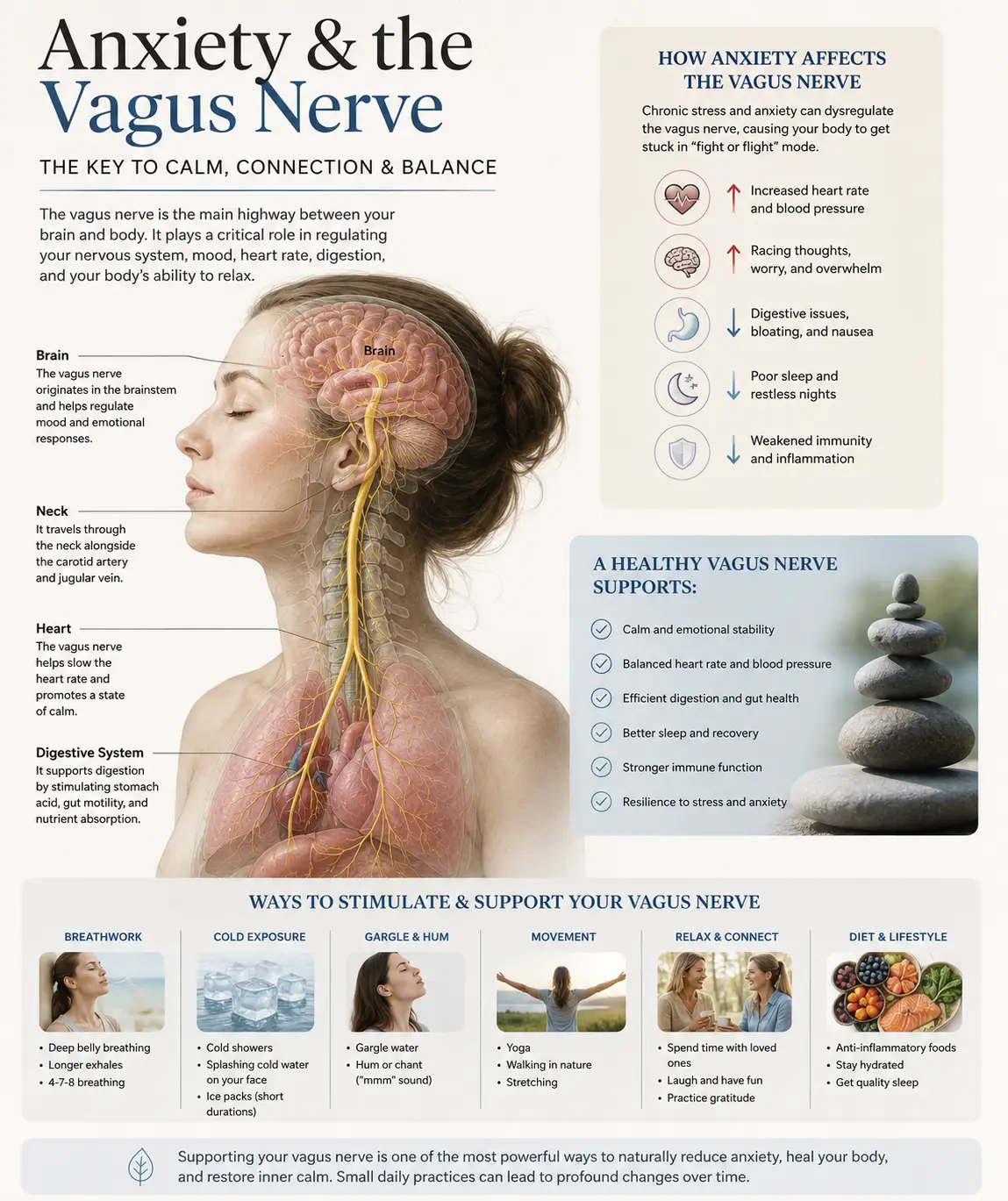
That motion illusion gets generated when there’s a mismatch between the three systems your brain uses to know where you are in space: your inner ears (the vestibular system), your eyes (visual input), and the receptors in your joints and muscles — especially the deep muscles of your upper neck (proprioception). When any one of those three sources sends bad data, your brain can’t reconcile it, and the result is vertigo.
Understanding which system is misfiring is the entire game. That’s why labeling someone with “vertigo” and sending them home with a motion sickness pill so often fails. It’s like calling every car problem “engine trouble” without ever opening the hood.
The Nerve and Vascular Connection You Need to Know
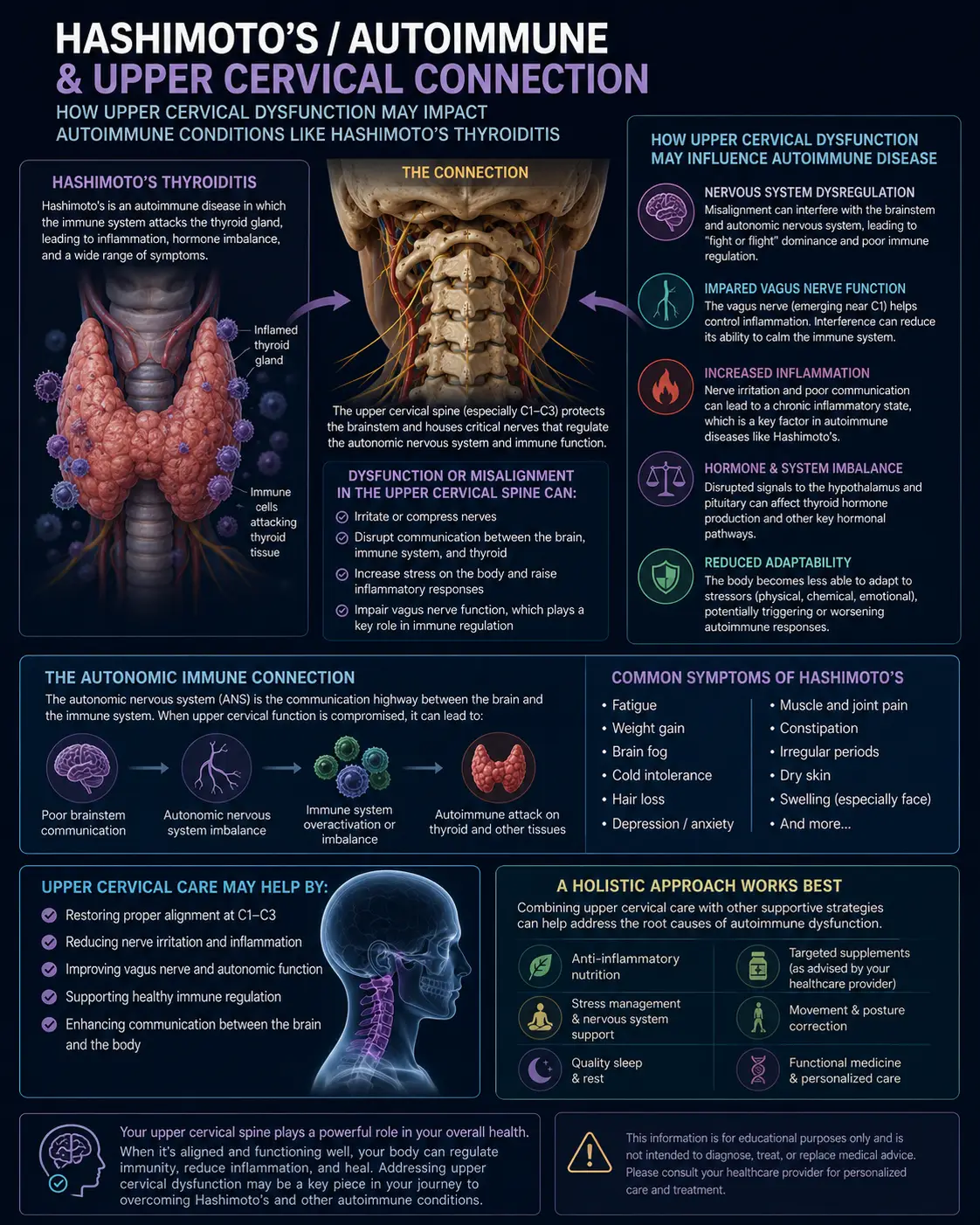
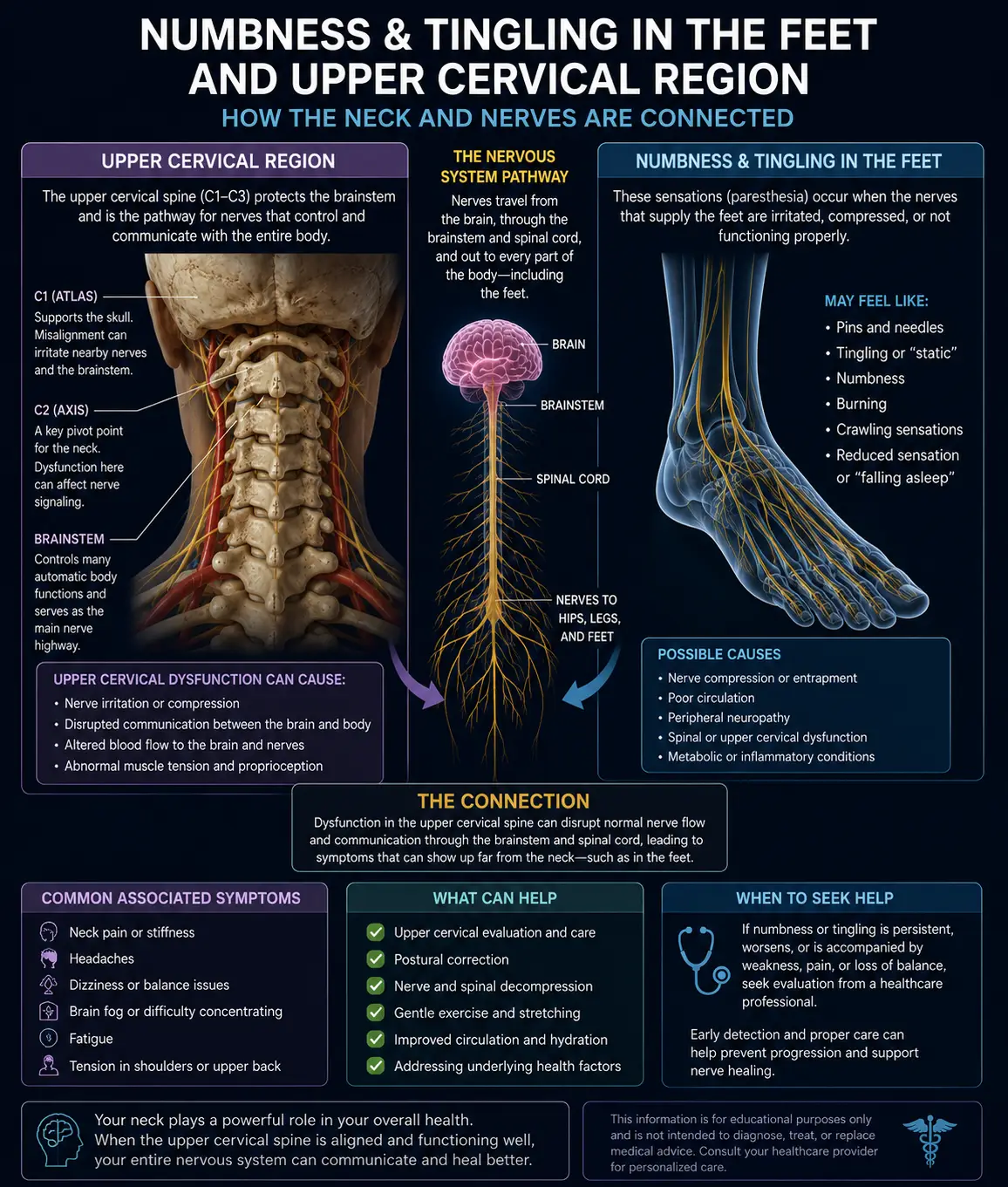
Before we dive into specific types, there’s an anatomical reality that ties almost all of them together: the upper cervical spine — the top two vertebrae of your neck, called the atlas (C1) and axis (C2) — sits directly underneath your brainstem and is wrapped around by some of the most important blood vessels in your body.
The vertebral arteries thread up through small holes in the cervical vertebrae and feed the brainstem, cerebellum, and inner ear structures with blood. The vestibular nuclei — the brain’s balance command center — live right inside the brainstem at this exact level. The vestibulocochlear nerve (cranial nerve VIII), which carries balance and hearing signals, exits the skull right here too. And the deep neck muscles around C1 and C2 contain a higher density of proprioceptive receptors than almost anywhere else in the body.
So when this region is misaligned, irritated, or restricted, every one of the systems involved in balance can be affected at once. That’s not a chiropractic talking point — that’s anatomy. And it’s exactly why so many people who never thought their vertigo had anything to do with their neck end up finding relief through upper cervical care.
Why the Upper Neck Matters So Much
The atlas and axis are unlike any other vertebrae in your spine. The atlas doesn’t have a body — it’s a ring that cradles the base of your skull. The axis has a peg called the dens that the atlas rotates around. Together they’re responsible for more than half of all the rotation in your neck. They also house the brainstem and sit at the gateway where the central nervous system transitions from brain to spinal cord.
A misalignment here doesn’t have to be dramatic to cause problems. A shift of even a millimeter or two can irritate nerves, alter blood flow, and disrupt the proprioceptive signaling that your brain depends on to know where your head is in space. The result, depending on which system gets the worst of it, can show up as any of the vertigo types we’re about to discuss.
Upper Cervical Care and What to Expect
At Lavender Family Chiropractic, Dr. Rusty Lavender and Dr. Jacob Temple use 3D Cone Beam Computed Tomography (CBCT) imaging to look at the upper cervical spine in three dimensions — something traditional flat X-rays simply can’t do. Combined with functional nervous system scans, this gives us a picture of not just where the bones sit, but how the nervous system is actually performing.
The adjustment itself isn’t what most people picture when they hear the word “chiropractor.” There’s no twisting, no cracking, no popping. It’s a gentle, precise correction delivered with a very specific line of force, calculated from your imaging. Many patients describe it as anticlimactic — and then walk out a few visits later realizing they haven’t had a vertigo episode in days.
Now let’s break down the major types of vertigo and what the research actually shows about each one.
Type 1: Benign Paroxysmal Positional Vertigo (BPPV)
BPPV is far and away the most common form of vertigo. According to a landmark population-based study published in the Journal of Neurology, Neurosurgery & Psychiatry, the lifetime prevalence of BPPV is around 2.4%, the one-year prevalence is 1.6%, and BPPV accounts for roughly 20–30% of all vestibular vertigo cases (read the study here).
BPPV happens when tiny calcium carbonate crystals called otoconia — the body’s natural “gravity sensors” inside the inner ear — break loose from where they belong and drift into one of the semicircular canals. These canals are filled with fluid and lined with motion-sensitive hair cells. When loose crystals slosh into them, every small head movement sends a wildly amplified motion signal to the brain. The result is intense, short-lived spinning, usually lasting less than a minute, triggered by specific positions: rolling over in bed, looking up at a shelf, tilting your head back at the dentist.
What most people don’t realize is how strongly BPPV is linked to head and neck trauma. The same study above found that age, migraine, hypertension, and stroke history all independently raised BPPV risk. And separate research published on PubMed shows that in post-traumatic BPPV, men and women are affected equally (1:1) — compared to the typical 2.3:1 female-to-male ratio in idiopathic cases — and bilateral involvement is far more common after trauma (study link).
There’s also a striking 2023 study in a traumatic brain injury rehabilitation population that found a remarkably high rate of BPPV — and notably, most of those patients hadn’t reported dizziness on their own. They had it. They just didn’t connect the dots (read the study here).
Why does this matter? Because the same forces that dislodge inner ear crystals — whiplash, falls, sports impacts, car accidents — also misalign the upper cervical spine. The Epley maneuver, which is the standard treatment for BPPV, can be very effective at repositioning the crystals. But if the underlying neck dysfunction isn’t addressed, BPPV often recurs. Recurrence rates of 15–50% within a few years are well documented in the literature. Patients who keep ending up back at square one are exactly the ones who benefit most from a deeper look at the upper cervical spine.
Type 2: Meniere’s Disease
Meniere’s disease is a chronic inner ear disorder that produces a very specific cluster of four symptoms: episodes of spinning vertigo lasting 20 minutes to several hours, fluctuating hearing loss (usually low-frequency at first), tinnitus (ringing or roaring in the affected ear), and a sense of fullness or pressure in the ear. The episodes can be brutal — patients often have to lie still for hours waiting for them to pass — and they’re frequently followed by exhaustion that can last for a day or more.
The current understanding is that Meniere’s involves abnormal fluid pressure (endolymphatic hydrops) inside the membranous labyrinth of the inner ear. What causes that pressure imbalance is still debated, but autoimmunity, viral involvement, genetic predisposition, allergies, and vascular factors have all been proposed.
Here’s where it gets interesting for our patients. A 2021 paper published in the Indian Journal of Otolaryngology and Head & Neck Surgery proposed a novel concept: that Meniere’s disease, BPPV, and cervicogenic dizziness may not be three completely separate diseases but rather points on a spectrum sharing significant cervical involvement. The researchers examined 132 vertigo patients and found cervical signs and symptoms across all three groups (read the full study here).
There’s also documented case-report evidence of patients with Meniere’s disease seeing significant symptom improvement following upper cervical and TMJ-focused chiropractic care. A case report published in the Journal of Chiropractic Medicine documented this in detail (read the case report).
To be clear: we don’t claim to “cure” Meniere’s, and no one honest does. But many Meniere’s patients have a coexisting cervical component that, when addressed, reduces episode frequency, severity, or both. For someone losing days of their life to attacks, that’s not a small thing.
Type 3: Vestibular Migraine
Vestibular migraine is now recognized as one of the most common causes of episodic vertigo — possibly more common than Meniere’s disease — and yet it’s underdiagnosed all the time. The Bárány Society established formal diagnostic criteria for it back in 2012, and the condition involves vertigo episodes that occur alongside migraine features (headache, light sensitivity, sound sensitivity, visual aura) — though importantly, the vertigo doesn’t have to happen at the same time as the headache.
Episodes can last anywhere from minutes to days. Patients often have a personal or family history of migraines, and triggers overlap with classic migraine triggers: poor sleep, stress, certain foods, hormonal changes, and weather shifts. Sarasota patients sometimes notice flare-ups around barometric pressure changes during the summer storm season.
Distinguishing vestibular migraine from Meniere’s can be difficult clinically, because they share so many features. A study in Frontiers in Neurology compared 100 patients with vestibular migraine to 100 with Meniere’s using vestibular evoked myogenic potentials (VEMPs) and found measurable differences in the cervical VEMP asymmetry ratio — a glimpse at the kind of work being done to tease these conditions apart (read the study).
The cervical connection here is meaningful too. The trigeminocervical complex — a hub in the brainstem where neck sensory nerves and the trigeminal nerve converge — is heavily implicated in migraine pathophysiology. Irritation in the upper neck can sensitize this complex, lowering the threshold at which migraine attacks fire. That’s why so many migraine and vestibular migraine patients notice their neck feels tight, stiff, or “off” before an episode — and why upper cervical correction often reduces attack frequency.
Type 4: Cervicogenic Vertigo (Cervical Vertigo)
Cervicogenic vertigo — sometimes called cervical vertigo or cervicogenic dizziness — is vertigo or dizziness whose primary driver is dysfunction in the cervical spine itself. It tends to be a chronic, sensory-mismatch type of dizziness rather than the dramatic spinning of BPPV. Patients describe it as floating, swaying, lightheadedness with movement, or just a constant low-grade “off” feeling that gets worse with certain neck positions.
The mechanism makes intuitive sense once you think about it. Your brain uses signals from neck proprioceptors to know where your head is relative to your body. When those signals are noisy or wrong because of cervical joint dysfunction or muscle imbalance, the brain receives motion data that doesn’t match what your eyes and inner ears are reporting. That’s a recipe for dizziness.
The research on manual therapy for cervicogenic dizziness is genuinely encouraging. A 2022 systematic review and meta-analysis in Healthcare looking at randomized controlled trials concluded that manual therapy targeting the upper cervical spine produces measurable improvements in dizziness intensity and balance parameters (read the full review).
Another systematic review published in Chiropractic & Manual Therapies found moderate (Level 2) evidence supporting manual therapy for cervicogenic dizziness, with consistent positive findings across studies (read the review). And a more recent 2025 systematic review in the Journal of Bodywork & Movement Therapies reported that all eight studies analyzed showed statistically significant improvements in dizziness intensity with manual therapy.
Cervicogenic vertigo is the type that responds most directly and most quickly to upper cervical chiropractic care — which makes sense, since it’s by definition a neck-driven condition.
Type 5: Vestibular Neuritis and Labyrinthitis
Vestibular neuritis is inflammation of the vestibular nerve, usually following a viral infection. Labyrinthitis is similar but involves the entire inner ear labyrinth, which means it includes hearing changes along with the vertigo.
The hallmark presentation is sudden onset, severe, constant vertigo lasting days at a time, often with significant nausea and vomiting. Most people end up in an emergency room during the first attack because it’s so intense and frightening. The acute phase typically lasts a few days to a week, but residual unsteadiness, motion sensitivity, and brain fog can linger for months.
That lingering phase is where things get interesting. The acute viral inflammation is over, but the brain has spent days receiving lopsided signals from the affected side. It now has to recalibrate — a process called vestibular compensation — and during that recalibration, accurate proprioceptive input from the neck becomes critical.
If the upper cervical spine is misaligned, the brain has bad reference data to compare the recovering ear signals against, and compensation stalls. We see this all the time: patients who had an acute viral vertigo attack months or years ago and just never fully got their balance back.
Type 6: Mal de Débarquement Syndrome (MdDS)
MdDS — French for “sickness of disembarkation” — is a rare but real condition where someone feels like they’re still on a moving boat, plane, or car long after they’ve gotten off. Patients describe a persistent rocking, swaying, or bobbing sensation that can last weeks, months, or even years. It’s most common after cruises but can follow flights, long road trips, or sometimes appear with no obvious trigger at all.
Interestingly, MdDS often improves when patients are in motion again (driving, walking, riding) and worsens when they’re still. That’s the opposite pattern of most vertigo and is one of the diagnostic clues.
The current research points to MdDS being a problem of maladaptive neural reorganization in the brainstem and vestibular system — the brain learns the motion pattern of the boat or plane and gets stuck running it. Because the upper cervical spine influences brainstem signaling and proprioceptive input, addressing it can be part of helping the brain “unstick” and reset to a normal motion baseline.
Type 7: Post-Traumatic Vertigo
Post-traumatic vertigo encompasses vertigo following any head, neck, or whole-body trauma — car accidents, sports collisions, falls, concussions, whiplash injuries. It’s not really one type so much as a category that can include traumatic BPPV, post-concussion vestibular dysfunction, cervicogenic vertigo of traumatic origin, and labyrinthine concussion.
The reason it gets its own category is that the mechanism — and the treatment plan — is fundamentally different from idiopathic vertigo. When trauma is involved, the upper cervical spine is almost always part of the picture, even if the impact didn’t seem to focus on the neck. The atlas and axis are exquisitely vulnerable to whiplash forces because of their position and their mobility, and post-traumatic patients tend to have measurable misalignments more often than the general population.
This is one of the areas where 3D CBCT imaging makes a real difference, because traditional X-rays can miss the kind of subtle rotational and lateral misalignments that follow trauma.
Other Types and Causes Worth Knowing
A few other vertigo causes show up regularly enough to mention. Acoustic neuroma is a benign tumor on the vestibular nerve that can cause progressive vertigo, hearing loss on one side, and tinnitus. Superior semicircular canal dehiscence is a rare condition where a thin spot in the bone above one of the canals lets pressure changes (loud sounds, sneezing, Valsalva) trigger vertigo. Perilymphatic fistula is a leak of inner ear fluid, often following barotrauma or head injury.
Multiple sclerosis and other central neurological conditions can cause vertigo when they affect the brainstem or cerebellum. Medications — particularly certain antibiotics, blood pressure medications, antidepressants, and sedatives — can produce drug-induced vertigo. Cardiovascular issues, low blood pressure, and dehydration can also masquerade as vertigo, especially in older adults.
These are reminders of why thorough evaluation matters so much. Not every spinning sensation is BPPV, and not every chronic dizziness is “just” anxiety. Vertigo deserves a real diagnostic workup.
Schedule Your Vertigo Consultation
If you’re reading this because vertigo is interrupting your life, you don’t have to keep guessing what type you have or which treatment to try next. At Lavender Family Chiropractic in Sarasota, we evaluate your upper cervical spine using 3D CBCT imaging and functional nervous system scans, then build a care plan around what’s actually driving your symptoms.
Call us at (941) 243-3729 to schedule your consultation, or book online. We’re located at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 — at the corner of University and Whitfield.
What the Research Says About Upper Cervical Care
One of the most common questions we get is, “Is there actually research behind this, or is it just chiropractors saying it works?” Fair question, and the answer is yes — there’s a growing body of peer-reviewed evidence connecting upper cervical care to improvements in vertigo and dizziness.
Beyond the studies linked throughout this article, the broader literature on chiropractic management of vestibular conditions includes published case reports in journals like the Journal of Chiropractic Medicine and Journal of Upper Cervical Chiropractic Research, systematic reviews showing positive effects of manual therapy on cervicogenic dizziness, and physiological research demonstrating that spinal manipulation affects primary afferent neurons in paraspinal tissues, which then influences how the central nervous system processes sensory information.
Is the research perfect? No. Many studies have small sample sizes or methodological limitations, and the field needs more high-quality randomized controlled trials. But the trend is consistent and the mechanism is anatomically reasonable. For patients who haven’t responded to standard care, it’s a worthwhile path to explore — especially given the safety profile of gentle upper cervical adjustment.
Lifestyle Factors That Influence Vertigo
While upper cervical care addresses the structural and neurological root, there’s a lot you can do day to day to support your recovery and reduce vertigo episodes.
Sleep is one of the most underrated factors. Sleeping on your stomach forces your neck into rotation for hours at a time and is a common driver of upper cervical irritation. Side or back sleeping with a properly contoured pillow is much friendlier to your atlas and axis. Staying well hydrated matters — inner ear fluid balance depends on systemic hydration, and Florida summers make dehydration easy to slip into. Limiting high-sodium foods can be especially important for Meniere’s patients, since sodium influences endolymphatic fluid pressure. Managing stress matters more than people realize, because chronic sympathetic nervous system activation increases muscle tension throughout the neck and shoulders, which mechanically stresses the upper cervical spine.
Posture during long hours at a screen is huge. Forward head posture loads the upper cervical region heavily and is one of the most common precursors to chronic neck dysfunction and dizziness. If you spend hours at a desk, look at our companion article on Why Vertigo Happens for a closer look at how everyday habits feed into the problem.
Regular movement helps too. Gentle exercise — walking, swimming, yoga — keeps your vestibular system engaged and your neck mobile without overloading it. And if you have a known history of vertigo, treating it as an ongoing health priority rather than waiting for the next attack tends to produce better outcomes.
Vertigo Care in Sarasota and Surrounding Areas
Lavender Family Chiropractic serves vertigo patients from across Southwest Florida. Our office at 5899 Whitfield Avenue is positioned conveniently for patients coming from Sarasota, Lakewood Ranch, Bradenton, University Park, Palmer Ranch, Siesta Key, Longboat Key, Osprey, Nokomis, Venice, Parrish, Ellenton, Myakka City, Ruskin, Palmetto, and the surrounding communities. Whether you’re a few minutes away or making the drive from further down the coast, we make the consultation and care process as straightforward as possible.
Sarasota patients in particular often appreciate the combination of beach-town pace and access to specialized care. You shouldn’t have to drive to Tampa or Orlando to get proper upper cervical evaluation, and you don’t. Everything we do — the 3D CBCT imaging, the nervous system scans, the personalized care plans — happens right here in our Whitfield Avenue office.
Top 15 Frequently Asked Questions About Vertigo Types
1. How do I know which type of vertigo I have?
Pattern matters more than you’d think. Brief spinning triggered by position changes points toward BPPV. Episodes lasting hours with hearing changes point toward Meniere’s. Vertigo with headache, light sensitivity, or visual aura points toward vestibular migraine. Constant low-grade unsteadiness worse with neck movement points toward cervicogenic vertigo. A thorough consultation and proper imaging help confirm.
2. Can I have more than one type of vertigo at the same time?
Yes, and it’s more common than people realize. Patients can have BPPV layered on top of a cervicogenic component, or vestibular migraine alongside Meniere’s, or post-traumatic vertigo with elements of multiple types. This is one reason single-treatment approaches often partially help but don’t fully resolve symptoms.
3. Is BPPV permanent?
The crystal displacement itself is treatable — usually with repositioning maneuvers like the Epley. But BPPV recurs in a significant percentage of patients within a few years. Recurrence is much more likely when underlying cervical dysfunction goes unaddressed.
4. Does upper cervical chiropractic work for Meniere’s disease?
It doesn’t cure Meniere’s, but published case reports and clinical experience suggest many Meniere’s patients with coexisting cervical involvement experience reduced episode frequency or severity with upper cervical care. The 2021 study reframing Meniere’s as part of a “cervicogenic spectrum” is worth reading if this applies to you.
5. How is the Lavender Family Chiropractic approach different from a regular chiropractor?
We focus specifically on the upper cervical spine — the atlas and axis — using 3D CBCT imaging and functional nervous system scans rather than relying on general adjustments. The corrections are gentle, precise, and calculated from your imaging. There’s no twisting, cracking, or popping.
6. What does a vertigo adjustment feel like?
Most patients describe it as anticlimactic. You lie comfortably on a specialized table while a precise, gentle force is applied to correct the misalignment. There’s no force you’d describe as “manipulation” in the traditional sense.
7. How quickly will I notice changes?
It varies. Some patients notice changes within the first few visits — fewer episodes, less intensity, more steadiness. Others need a longer arc of care, especially if the dysfunction is long-standing. We monitor progress closely and reassess regularly.
8. Is upper cervical chiropractic safe?
Upper cervical care performed by trained doctors using imaging guidance has an excellent safety profile. The gentle, precise nature of the correction is fundamentally different from the high-velocity manipulations that have raised safety questions in the past.
9. Can vertigo come from whiplash or a car accident?
Absolutely, and often does. Post-traumatic vertigo can show up immediately or develop weeks to months later. Both inner ear involvement and upper cervical injury can contribute, sometimes simultaneously.
10. Why does my vertigo get worse with stress?
Stress increases sympathetic nervous system tone, which heightens muscle tension throughout the neck and shoulders. That mechanical load on the upper cervical spine can amplify pre-existing dysfunction. Stress also increases sensitivity within the vestibular system itself.
11. Will I need to come in forever?
No. We work toward stability — getting your spine holding its corrections and your nervous system functioning normally. Many patients move to occasional maintenance visits once they’ve reached that point.
12. Can I exercise with vertigo?
Usually yes, with adjustments. Walking, swimming, and gentle movement help most vertigo patients. High-impact activities or anything involving rapid head movement may need to wait until symptoms stabilize.
13. Do I need a referral to see you?
No referral needed. You can call us directly at (941) 243-3729 to schedule a consultation.
14. Is upper cervical chiropractic covered by insurance?
Coverage varies by plan. We can verify your benefits before your first visit so you know exactly what to expect.
15. What if my vertigo turns out not to be cervical?
Then we tell you. Part of our evaluation process is determining whether upper cervical care is genuinely indicated. If it’s not, we’ll point you toward the right resource — an ENT, a neurologist, a vestibular physical therapist, whoever fits the picture.
Take the Next Step Toward Real Vertigo Relief
Vertigo is one of those conditions where most people accept far less function and far more episodes than they need to, simply because no one has fully explained their options. Now you’ve seen the major types, the mechanisms behind them, and the research connecting upper cervical care to relief.
If any of this resonates — if you have BPPV that keeps coming back, Meniere’s that controls your calendar, vestibular migraines that ambush you, cervicogenic dizziness no one has named, or post-traumatic vertigo from an injury years ago — we’d genuinely like to help.
Call (941) 243-3729 to schedule your consultation, or book your appointment online. Our office is at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243, at the corner of University and Whitfield.
For the full overview of how we approach vertigo, head back to our main resource: Vertigo Doctor Sarasota: Proven Relief with Upper Cervical Chiropractic at Lavender Family Chiropractic.
Related Articles
Why Vertigo Happens: Our #1 Guide to Resolving the Spinning
Vestibular Therapy and Upper Cervical Chiropractic Care for Vertigo and Dizziness