Hyperacusis: If you live in Sarasota, Lakewood Ranch, Bradenton, or anywhere along the Suncoast, you already know what it sounds like here. The drone of cicadas on a humid August evening. The clank of dishes at a packed brunch on Main Street. Pickleball paddles at Bobby Jones. The roar of a leaf blower across the street. Thunder rolling in off the Gulf at 4 p.m. like clockwork.
For most people, these are just the everyday sounds of Florida life. But for a growing number of our patients, they are something else entirely — they are painful. A normal volume conversation feels like someone is shouting in your ear. A clattering fork sets your teeth on edge. A car horn makes you flinch and want to cry. A child’s laugh feels like it’s piercing your skull. You find yourself wearing earplugs in restaurants. You avoid grocery stores. You can’t sit through a movie. You dread family gatherings.
This is hyperacusis — an abnormally reduced tolerance to ordinary sound. And while most patients are sent down the road to audiologists and ENTs (which is often a great first step), there is a piece of the puzzle that is almost universally missed: the upper cervical spine — the very top of your neck, where your skull meets your spinal cord.
In this guide we are going to walk through, in plain English, what hyperacusis actually is, why the published neurology research keeps pointing back to the neck, what we see on 3D imaging here in our Sarasota office, what to expect at a visit at Lavender Family Chiropractic, and how a gentle, specific correction to the atlas (C1) and axis (C2) can change the entire trajectory of someone’s sound sensitivity.
If you have been suffering, please keep reading. There is hope, and there is a logical reason it has been so hard to find.
What Is Hyperacusis, Really?
Hyperacusis is the medical term for a decreased tolerance to sounds that the average person finds completely normal. It is not the same thing as having sharp hearing or “good ears.” In fact, many people with hyperacusis have totally normal hearing on a standard audiogram. The volume coming in is the same as it is for everyone else — but the brain’s interpretation of that volume is turned up far too high.
People describe it in different ways:
- “It feels like everything has been cranked up to 11.”
- “Forks scraping plates is physically painful.”
- “I can’t be in Publix without earplugs.”
- “My own voice sounds too loud.”
- “Running water in the sink is unbearable.”
- “I dread the air conditioner kicking on.”
Hyperacusis often travels with other unwelcome companions. The same patient who has sound sensitivity will frequently also report tinnitus (ringing or buzzing in the ears), ear fullness, light sensitivity, headaches or migraines, dizziness, jaw tension, brain fog, anxiety in noisy environments, and difficulty sleeping. There is a reason for that pattern, and we will get there.
The most accepted neurological explanation is something called central gain — the idea that the brain progressively amplifies sound signals as they travel up from the ear to the higher centers. When that gain knob gets stuck in the “up” position, ordinary sound becomes overwhelming, and in some cases physically painful. Published reviews of hyperacusis describe this as a process where neural signals are progressively amplified as they ascend through the classical auditory pathway and through non-auditory regions involved in emotion, memory, and stress. Translation: hyperacusis is not just an “ear problem.” It is a brain and nervous system problem.
And once you understand that, the door opens to talking about the upper neck.
The Neurology Connection: Why the Brain’s “Volume Knob” Lives Right Next to Your Atlas
This is the part the lay person almost never gets explained to them, and it is the part that changes everything.
Deep inside your brainstem — the part of your nervous system that sits right behind and just above the atlas (C1) vertebra at the top of your neck — there is a small structure called the dorsal cochlear nucleus, or DCN for short. Think of the DCN as one of the brain’s first relay stations for sound. Signals from the ear arrive here, get processed, and then get passed up the chain to the auditory cortex where you actually “hear.”
Here is the part nobody tells you in the ENT office: the dorsal cochlear nucleus does not only listen to your ears. It also listens to your neck and jaw.
Researchers have repeatedly shown that the DCN receives direct input from the cervical nerves of the upper neck (especially the C2 dorsal root ganglion) and from the trigeminal system that supplies the face and jaw. A 2024 narrative review in the medical literature put it bluntly: the pathophysiology of cervicogenic somatic tinnitus and related sound disorders involves “complex interactions between the cervical spine’s somatosensory inputs and central auditory pathways, particularly affecting the dorsal cochlear nucleus (DCN) in the brainstem, leading to enhanced excitability and synaptic reorganization.” That is medical language for: when your neck sends abnormal signals upstairs, the brain’s sound-processing center gets jacked up and stays jacked up.
In simpler terms — imagine a sound mixing board with two main sliders feeding into the master volume:
- Slider 1: Input from the ear (the cochlea)
- Slider 2: Input from the neck and jaw (the somatosensory system)
When the upper cervical spine is misaligned, irritated, or sending chaotic mechanoreceptor signals, that second slider is shoved up — and the master volume rises with it. The result is a brain that is constantly being told the world is too loud, even when it isn’t.
This is not a fringe theory. The same mechanism has been demonstrated for somatosensory tinnitus, where patients can actually change the loudness and pitch of their ringing simply by moving their neck or clenching their jaw. A study reviewed in the medical literature reported that the prevalence of somatosensory tinnitus — tinnitus that responds to neck or jaw movement — is around 29.5% in individuals with hyperacusis. That is not a coincidence. That is the upper neck talking directly to the auditory brainstem.
A 2023 clinical study from the University Hospital of Antwerp went even further. Researchers tested whether isolated movements of the cervical spine and jaw could change the perceived loudness of sound in hyperacusis patients. The fact that this study was even designed tells you where the field is heading: the upper neck is being recognized as a modulator of hyperacusis, not just an unrelated bystander.
There is also growing research that hyperacusis is associated with structural changes in non-auditory parts of the brain — including the supplementary motor area, the anterior cingulate cortex, and the orbitofrontal cortex. Why does this matter to a neck-focused doctor? Because these are exactly the regions whose function depends on a healthy, calm, well-regulated brainstem — and the brainstem depends on a properly aligned upper cervical spine to do its job without interference.
So when somebody says, “How could my neck possibly affect how loud the world sounds?” — there is now a clean, published, scientific neurological pathway that answers that question.
The Upper Neck: Where Hearing, Balance, and the Nervous System All Meet
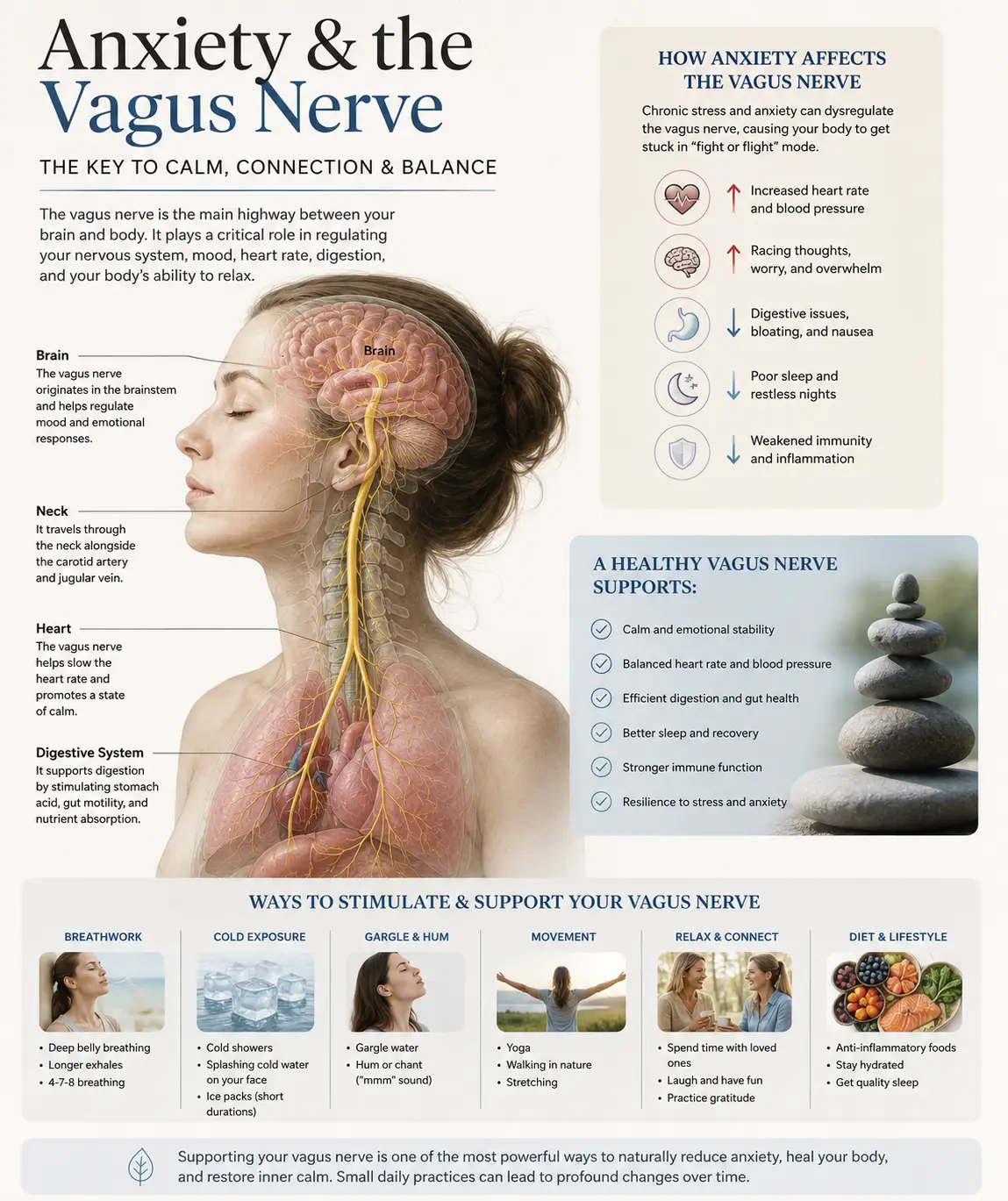
The atlas (C1) and axis (C2) are the top two bones of the spine, and they are unlike any other vertebrae in the body. They have to be — they have to hold up an 11-pound head, allow your skull to nod and rotate, and leave room for the brainstem and spinal cord to pass through them without being compressed.
Sitting in and around this small area are some of the most important structures in your entire body:
- The brainstem, which controls heart rate, breathing, blood pressure, sleep, and the volume gain of incoming sensory information (including sound).
- The dorsal cochlear nucleus, the auditory relay we just discussed.
- The vagus nerve, the main highway of the parasympathetic (“rest and digest”) nervous system.
- The trigeminal nucleus, which handles sensation from the face, jaw, and inner ear muscles.
- The vertebral arteries, which supply roughly 20% of your brain’s blood flow.
- The upper cervical nerve roots (C1, C2, C3) that share processing space with the trigeminal system and the auditory system.
When the atlas or axis becomes misaligned — from a fall as a child, a car accident, a sports injury, a difficult birth, repetitive postural strain, or even a hard hit while playing pickleball — the chaos doesn’t just stay local. The neck doesn’t just hurt (and sometimes it doesn’t hurt at all). Instead, that misalignment sends a steady stream of confused mechanoreceptor signals into the brainstem.
And those signals land directly on the same neurons that process sound, balance, and pain.
This is the part of the conversation people in Sarasota tell us they have never heard before. They have seen the audiologist, the ENT, the neurologist, the primary care doctor. They have tried sound therapy, antidepressants, white noise machines, hearing aid–style devices. Sometimes those help — and sometimes they don’t, because nobody has addressed the upstream signal coming from the neck.
Vascular and Blood Flow Component
There is one more layer to this, and it gets brushed past too often. The vertebral arteries travel up through small holes in the sides of the C1 and C2 vertebrae before entering the skull. If the upper cervical alignment is off, those arteries can be subjected to abnormal mechanical stress, which over time can influence blood flow into the brainstem and inner ear.
The inner ear is one of the most metabolically demanding tissues in the entire body and is exquisitely sensitive to reductions in blood supply. When blood flow gets dialed back even a little — through vertebral artery tortuosity, sympathetic over-activation from a stressed upper neck, or both — the cells of the cochlea and the auditory brainstem become less stable. And unstable auditory neurons are exactly the kind that produce hyperacusis, tinnitus, and “central gain” amplification.
Combine the mechanical mis-signaling (slider #2) with the vascular compromise, and you have a perfect recipe for a brain that thinks every sound is too loud.
Upper Cervical Chiropractic Care: A Different Kind of Adjustment
When most people picture chiropractic care, they picture the dramatic neck twist and the loud crack. That is not what we do at Lavender Family Chiropractic, and it is especially not what we do for someone whose nervous system is already on fire.
Upper cervical chiropractic is a specialized branch of chiropractic that focuses exclusively on the alignment of the atlas (C1) and axis (C2). Our office uses a specific technique called AHKC (Advanced HIO Knee-Chest), performed on a knee-chest table that supports the head, neck, and chest in a neutral position. There is no twisting, no popping, no cracking, no yanking. The correction itself is a quick, light, mathematically pre-calculated impulse — most patients are surprised at how gentle it is.
That gentleness is not a marketing line. It is a clinical necessity. The hyperacusis patient’s nervous system is already over-amplified — the last thing it needs is a high-force, generalized adjustment that floods the brainstem with even more sensory noise. Our entire approach is built around: correct the exact bone, in the exact direction, with the exact amount of force, and then get out of the way and let the nervous system reorganize itself.
What to Expect at Lavender Family Chiropractic
When you come in, here is the process we walk every patient through:
Consultation. We sit down and listen — really listen — to your full health story. Old injuries, car accidents, falls, concussions, birth history, when your sound sensitivity started, what makes it worse, what other symptoms travel with it (tinnitus, ear pressure, dizziness, headaches, jaw tension, anxiety). The detail matters because we are reconstructing the timeline of when your upper cervical spine was first compromised.
3D CBCT Imaging. We take a Cone Beam CT scan of your upper cervical spine. Unlike a flat 2D X-ray, the CBCT lets us see the atlas and axis from every angle and measure the misalignment down to one-hundredth of a millimeter. This is critical, because every patient’s anatomy is different — your atlas does not look like anyone else’s.
Functional Nervous System Scans. We use paraspinal infrared thermography (Tytron) to map how your nervous system is currently functioning along the spine. Hyperacusis patients almost always show asymmetric thermal patterns and elevated sympathetic (“fight or flight”) output — objective evidence that the nervous system is dysregulated.
Custom Correction Plan. Using the CBCT measurements and the scan data, we build a correction formula that is specific to your spine. Then we make the adjustment — gently, on the knee-chest table — and re-scan to confirm the correction held.
Tracking & Re-Care. Hyperacusis didn’t develop in a day, and it doesn’t resolve in a day either. The goal of upper cervical care is to hold the correction long enough for the nervous system to recalibrate — to let that “central gain” turn back down. Some patients notice changes in days; for many, it is a gradual quieting of the world over weeks and months.
For a deeper look at the specific technique, technology, and step-by-step process we use, you can read our full breakdown on the Atlas Chiropractic blog page.
Ready to Stop Suffering Through Every Loud Restaurant?
If you are tired of wearing earplugs to dinner, dreading the school pickup line, and avoiding social events because the world is just too loud — we want to help. Call (941) 243-3729 or schedule a complimentary consultation at our Sarasota office today.
What Does the Research Say About Manual Care of the Upper Neck and Sound Disorders?
A fair question, and one we get asked all the time: “Is there actual research on this, or is this just a chiropractor’s pet theory?”
Here is what the published literature shows:
- Cervicogenic somatic tinnitus is now a recognized clinical entity in the medical literature, with a clear pathway from cervical somatosensory input → dorsal cochlear nucleus → tinnitus and sound perception abnormalities (PMC, 2024).
- Somatosensory modulation of sound tolerance has been studied directly in hyperacusis patients. The 2020–2021 Antwerp clinical trial specifically used cervical spine and jaw modulations to see whether they could change the loudness and intrusiveness of sound in hyperacusis. The fact that researchers are testing upper neck input as a hyperacusis intervention tells you exactly which way the science is moving.
- The C2 dorsal root ganglion projects directly to the cochlear nucleus in animal models (Zhan et al., J Comp Neurol, 2006). That is the anatomical hardware that connects your upper neck to your auditory processing.
- Upper cervical instability is associated with sensory hypersensitivity syndromes including hyperacusis, photophobia, and trigeminal-mediated facial pain (Caring Medical, 2024–2025 reviews).
- Hyperacusis has measurable brain changes, including altered gray matter in the supplementary motor area and abnormal beta-wave activity in non-auditory cortex (Koops et al., 2023) — evidence that this is a whole-nervous-system problem, not just an ear problem.
We are not claiming upper cervical chiropractic is a cure for hyperacusis. What we are claiming — supported by an increasingly clear body of neurology — is that the upper neck is a meaningful, addressable input into the brain’s volume control system, and that for a large subset of hyperacusis sufferers, correcting that input is the missing piece.
If you also struggle with ringing in the ears alongside the sound sensitivity, our companion article on tinnitus and upper cervical care walks through the very same neurological pathways in more depth.
Lifestyle Pieces That Either Help or Hurt the Recovery
The adjustment is the foundation. But what you do between visits matters too — and a lot of it overlaps with calming an over-amplified nervous system.
Sleep posture. Stomach-sleeping forces the upper neck into a sustained rotation for 6–8 hours a night. We see this on imaging constantly. Side or back sleeping, with a pillow that supports (not pushes) the neck, helps the correction hold.
Hydration. The brain and brainstem do not function well dehydrated. The inner ear is essentially a fluid-filled organ. In our Florida heat, even mild dehydration can magnify both tinnitus and sound sensitivity. Aim for half your body weight in ounces of water daily.
Slow, gentle resensitization — not “toughing it out.” The instinct with hyperacusis is to either hide in earplugs all day or, swinging the other way, force yourself into loud environments to “get used to it.” Both extremes backfire. Complete sound avoidance actually increases central gain (the brain compensates by turning the volume even higher). Forced overload retraumatizes the system. The sweet spot is gentle, gradual exposure to comfortable everyday sound — and that becomes much easier once the upstream cervical signal is corrected.
Stress and the vagus nerve. Hyperacusis lives in a sympathetic-dominant (“fight or flight”) nervous system. Slow nasal breathing, gentle walks, time outdoors, and limiting stimulants like caffeine all support the parasympathetic side. The upper cervical correction supports vagus nerve function from the top down; lifestyle supports it from the rest of the body up.
Avoiding repetitive forceful neck manipulation. If you have hyperacusis, we strongly recommend against high-force, rotational, “crack the neck” type adjustments. They can temporarily aggravate the very brainstem irritation we are trying to calm. Gentle, specific, low-force care is the right tool for this job.
If you also experience that maddening clogged, popping, “airplane” feeling in your ears as part of your sound sensitivity picture, we go very deep into that mechanism in our Ear Pressure and Eustachian Tube Dysfunction article — it shares a lot of root-cause DNA with hyperacusis.
Serving Sarasota and Beyond
Our office is conveniently located at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243, right at the corner of University and Whitfield. We proudly serve patients from across the Suncoast and beyond — Sarasota, Lakewood Ranch, Bradenton, Parrish, Ellenton, Palmetto, Venice, Osprey, Siesta Key, Longboat Key, Lido Key, Myakka City, North Port, Ruskin, St. Pete, and Tampa. We have patients fly in from out of state for upper cervical care, because there are only so many offices in the country doing it at this level of precision.
If you would like to learn more about what we do day-to-day and the conditions we work with, our main Upper Cervical Care in Sarasota & Lakewood Ranch page is a great place to dig in. To meet the doctors and see what makes our process different, the home page of chiropractorsarasotaflorida.com has video walkthroughs and patient testimonials.
If you have already explored ENT care, you may also be interested in how upper cervical care works alongside your existing ENT — we dive into that on our Integrative Care with ENT page. And for anyone whose sound sensitivity comes with dizziness, our Vertigo page with Dr. Jacob Temple explains how the same upper cervical mechanism drives both. For a comprehensive look at every condition we work with and what to expect as a new patient, see our Chiropractor Near Me deep-dive.
Top 15 Frequently Asked Questions About Hyperacusis and Upper Cervical Chiropractic
1. Is hyperacusis the same thing as misophonia?
No. Misophonia is an emotional reaction (anger, disgust, anxiety) to specific trigger sounds — chewing, sniffing, tapping. Hyperacusis is a physical intolerance to the volume of ordinary sound, even sounds that don’t bother you emotionally. They can overlap, and the upper cervical connection appears to apply primarily to hyperacusis, though the central gain mechanism is relevant to both.
2. Will upper cervical chiropractic cure my hyperacusis?
We do not promise cures, and we are skeptical of anyone in healthcare who does. What we can say is that for patients whose hyperacusis has a meaningful upper cervical and somatosensory component — which the research suggests is a sizeable portion of cases — correcting the atlas and axis often produces significant, measurable, lasting improvement. The only way to know whether you are one of those patients is a thorough exam and imaging.
3. Why doesn’t my ENT mention the neck?
Because most ENT training is focused on the structures of the ear itself — the eardrum, ossicles, cochlea, and auditory nerve. The dorsal cochlear nucleus and the cervical somatosensory inputs sit in the brainstem, which is technically neurology territory. It is a gap in conventional care, not a failing of any one specialist.
4. Does this only help if I have neck pain?
No. In fact, many of our hyperacusis patients have no neck pain at all. The upper cervical spine can be significantly misaligned without producing local pain, because the joints there are designed for mobility, not load-bearing. Imaging tells the truth, not symptoms.
5. How long until I see changes?
It varies. Some patients notice softening of sound sensitivity within the first few visits. Others — particularly those with longstanding hyperacusis, prior head/neck trauma, or significant central gain — see a slower, layered improvement over weeks to months. Holding the correction is what allows the brain to recalibrate.
6. Is the adjustment safe for someone whose nervous system is already overstimulated?
Yes — when done with the right technique. Our AHKC approach is gentle, low-force, and specific. There is no twisting, popping, or general manipulation. We see hyperacusis patients regularly, and the gentleness of the correction is one of the reasons they tolerate care so well.
7. Can a car accident from years ago cause this?
Absolutely. Whiplash injuries are one of the most common upper cervical traumas we see, and they can produce symptoms that don’t fully express themselves for months or years. Hyperacusis, tinnitus, dizziness, and brain fog are all on the list of post-whiplash chronic complaints.
8. What about a concussion or sports injury?
Same answer. Any significant impact to the head or neck — including concussions that didn’t seem “that bad” at the time — can leave the upper cervical spine compromised. Many of our hyperacusis patients trace their onset to an injury they had partly forgotten about.
9. Do I need to stop using my earplugs or noise-cancelling headphones?
Not abruptly. The goal long term is to need them less, not to white-knuckle through painful sound. As care progresses and central gain comes down, most patients naturally reach for them less. Don’t force the transition — let it happen.
10. Will this help my tinnitus too?
Often, yes. Hyperacusis and tinnitus share so much underlying neurology (both involve the dorsal cochlear nucleus, both involve central gain, both respond to somatosensory modulation) that addressing the upper cervical input frequently helps both at the same time.
11. I have hyperacusis AND migraines. Connection?
Strongly so. Migraines, hyperacusis, photophobia (light sensitivity), and osmophobia (smell sensitivity) all share a hyperexcitable trigeminal-brainstem network — exactly the network most affected by upper cervical alignment. It is extremely common to see all of these improve together when the upper neck is corrected.
12. Do you take insurance?
We offer complimentary consultations so you can sit down with us before making any financial decisions. Coverage varies widely by plan, and we will walk you through the specifics during your visit. Most importantly — we want money never to be the reason someone doesn’t get the care they need, so we work with people to find a path forward.
13. Can children get upper cervical care for hyperacusis?
Yes. We see pediatric patients regularly, and many children with sensory processing issues, including sound sensitivity, have upper cervical findings dating back to birth or early childhood falls. The technique is gentle enough for infants.
14. Is this covered by clinical research enough for me to feel comfortable trying it?
The research linking cervical input to sound processing in the brainstem is robust and growing every year. The research specifically on chiropractic adjustment for hyperacusis is younger and smaller — that is honest. What we can offer you is the neurological mechanism, the clinical experience of hundreds of patients we have personally worked with, and a thorough exam to determine whether your case is a good fit. We will tell you if it isn’t.
15. How do I get started at Lavender Family Chiropractic?
Easy. Call (941) 243-3729 to schedule a complimentary consultation, or book online through our website. We’ll sit down, listen to your full story, and from there decide together whether imaging and care make sense for you.
You Don’t Have to Live This Way
If there is one thing we want anyone reading this to take away, it is that hyperacusis is not a character flaw, not “being too sensitive,” and not something you have to white-knuckle through for the rest of your life. There is real, repeatable neurology behind what is happening to you — and there is a real, repeatable input from the upper cervical spine that, in many people, is keeping the volume knob jammed in the up position.
You deserve a meal out without earplugs. You deserve a quiet morning where the coffee grinder doesn’t make you cry. You deserve to sit on Lido Key and listen to the waves instead of dreading them. You deserve to be present at your grandchild’s birthday party.
At Lavender Family Chiropractic, our entire mission is to find the root cause and address it gently, precisely, and with the best technology available. Dr. Rusty Lavender and Dr. Jacob Temple would be honored to sit down with you and figure out whether your upper neck is part of your story.
📍 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 (corner of University & Whitfield) 📞 (941) 243-3729 🌐 www.chiropractorsarasotaflorida.com 📲 Instagram: @lavenderfamilysrq | TikTok: @drrustylavender
Book your complimentary consultation today — your nervous system has been waiting for somebody to look in the right place.
Related Articles
- Tinnitus Sarasota: Find Hope For Ringing Here at LFC — A deep dive into how the same dorsal cochlear nucleus pathways that drive hyperacusis also produce ringing, buzzing, and pulsatile tinnitus, and how upper cervical care addresses both at the root.
- Ear Pressure, Eustachian Tube Dysfunction, and Proven Relief at Upper Cervical Chiropractic Care in Sarasota — If your sound sensitivity comes packaged with chronic ear fullness, popping, or that “airplane” feeling, this article walks through the shared upper cervical mechanism.
- Atlas Chiropractic: Understanding the C1 Vertebra and Why It Matters — A comprehensive look at the atlas vertebra itself, why misalignment in this one tiny bone produces such widespread symptoms, and how our specific technique restores it.
- “Pilot study on the role of somatic modulation in hyperacusis” Authors: Sara Demoen, Sarah Michiels, Annick Gilles, Hanne Vermeersch, Iris Joossen, Olivier M. Vanderveken, Marc J. W. Lammers, Annick Timmermans, Vincent Van Rompaey, David Baguley, Laure Jacquemin Journal: European Archives of Oto-Rhino-Laryngology, Vol. 280, Issue 3, pages 1425–1435 (March 2023; published online October 13, 2022) DOI: 10.1007/s00405-022-07695-y PubMed ID: 36224398 Clinical trial registration: NCT04693819 Link: https://pubmed.ncbi.nlm.nih.gov/36224398/
Author’s note: This article is for educational purposes only and is not a substitute for individualized medical evaluation. If you are experiencing severe or sudden changes in hearing, sound tolerance, or neurological symptoms, please also consult an audiologist, ENT, or neurologist. We work alongside — not in place of — your medical team.