Ménière’s Disease: If you found this article, there is a good chance you have already been down the rabbit hole. You have spent hours typing symptoms into a search bar at 2 a.m. — “ear feels full and ringing,” “world spinning when I turn my head,” “dizzy and nauseous for hours.” You have been to your primary care doctor, maybe to urgent care, possibly to an ENT in Sarasota or Lakewood Ranch. You have had your ears looked into, your blood pressure checked, your blood drawn. And someone, somewhere along the way, said two words that you cannot stop thinking about: Ménière’s disease.
Or maybe no one has said those words yet. Maybe you read our main vertigo article and something clicked — but your story doesn’t quite match the classic positional vertigo description. Yours is louder. Heavier. There’s pressure in one ear. There’s a roar like a seashell that won’t go away. The attacks come out of nowhere and steal entire afternoons from you.
If that sounds familiar, please keep reading. This article is here to help you understand what Ménière’s disease actually is, why so many people who think they have “just vertigo” are really dealing with a much bigger neurological and vascular puzzle, and — most importantly — why the upper neck is one of the most overlooked players in this entire condition.
At Lavender Family Chiropractic in Sarasota, our doctors, Dr. Rusty Lavender and Dr. Jacob Temple, have spent years working with patients across Sarasota, Bradenton, Lakewood Ranch, Venice, and Siesta Key who walked in feeling exactly the way you might be feeling right now. Hopeless. Exhausted. Tired of being told everything looks “normal” on the scans. This is for you.
What Is Ménière’s Disease, Really?
Ménière’s disease is an inner ear disorder that produces a very specific four-symptom cluster that, taken together, can absolutely upend a person’s life. The classic textbook description includes:
- Episodes of spontaneous vertigo lasting from 20 minutes to several hours
- Fluctuating sensorineural hearing loss, often in one ear
- Tinnitus — a roaring, ringing, or buzzing sound, usually low-pitched
- Aural fullness — the unmistakable feeling that your ear is plugged, pressurized, or filled with water
It was first described in 1861 by a French physician named Prosper Ménière, who proposed something radical for his time: that vertigo could originate from a problem inside the ear itself, not from the brain. He was right. And we have spent the last century and a half trying to figure out exactly what that “problem inside the ear” actually is.
The leading theory today is something called endolymphatic hydrops — a buildup of fluid inside the membranous labyrinth of the inner ear. Inside your inner ear, there are two fluids: endolymph and perilymph. They are carefully separated, and they exist in a delicate balance that allows your vestibular system to detect motion and your cochlea to translate sound waves into electrical signals your brain can interpret. When endolymph builds up in excess — when pressure rises and the membranes stretch — the system breaks down. The result is the vertigo, the hearing changes, the ringing, and the fullness that define Ménière’s.
But here is where things get genuinely interesting, and where most articles you read online stop short. The cause of that fluid buildup is still considered “unknown” in most medical literature. Theories range from autoimmune reactions, to viral inflammation, to allergies, to genetic predisposition, to migraine variants, to circulatory problems. And buried in that list — almost never highlighted — is one of the most clinically relevant possibilities for the people we see every single week in our Sarasota office: upper cervical spine dysfunction affecting nervous system regulation, vascular drainage, and brainstem function.
The Nerve and Vascular Pathways That Connect Your Neck to Your Inner Ear
To understand why a chiropractor in Sarasota would write a 4,000-word article about an inner ear disorder, you have to understand a piece of anatomy that very few people, including many physicians, fully appreciate.
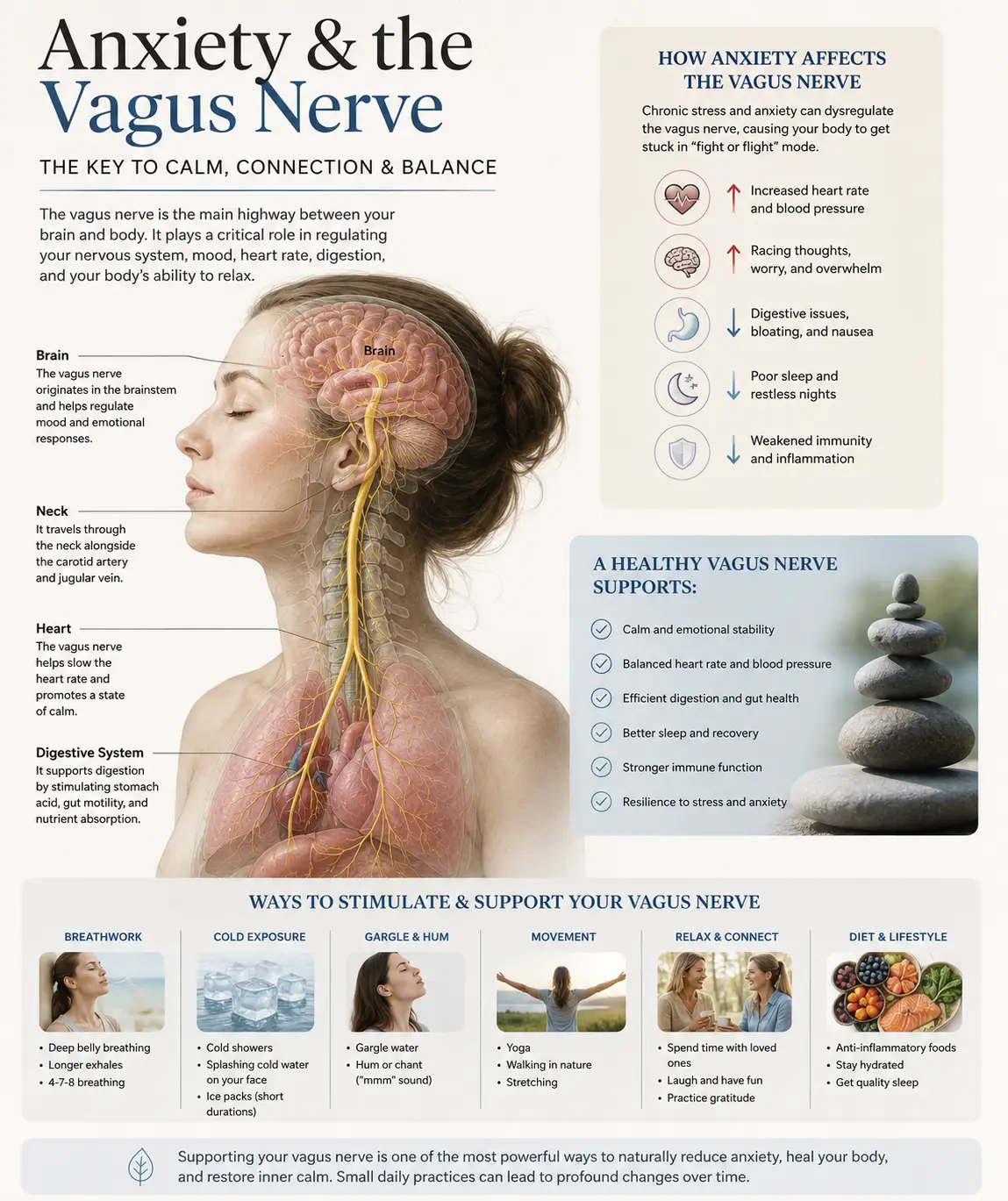
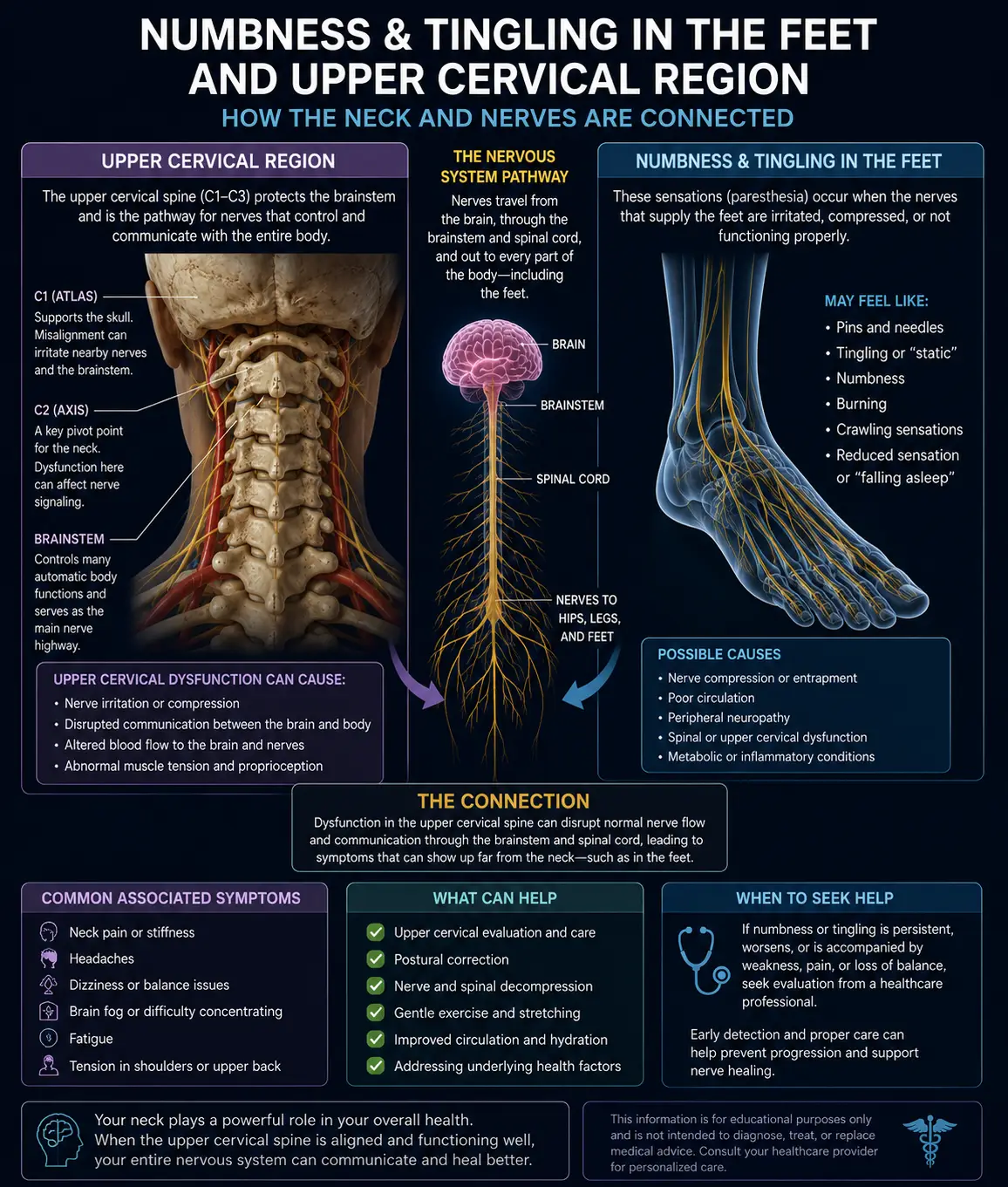
Your inner ear does not float in space. It is not a self-contained, isolated system. It is intimately wired into your brainstem — specifically, the lower brainstem and the cervicomedullary junction. The vestibulocochlear nerve (cranial nerve VIII), which carries balance and hearing information into your brain, enters the brainstem at the level of the pontomedullary junction. That junction sits inches — sometimes less — from your atlas vertebra (C1) and axis vertebra (C2).
The vagus nerve (cranial nerve X), which regulates so much of your autonomic function, including aspects of inner ear blood flow, also emerges from this region. Your glossopharyngeal nerve (CN IX), which contributes to swallowing and middle ear pressure regulation through its connection to the Eustachian tube, lives there too. Your accessory nerve (CN XI), your hypoglossal nerve (CN XII), and the upper cervical nerves themselves all converge in the same small, crowded neighborhood at the base of your skull.
Now add the vascular component. Your vertebral arteries travel up through the transverse foramina of your cervical vertebrae, looping in a complex path around C1 before entering the skull through the foramen magnum to form the basilar artery — which supplies blood to your brainstem and, by extension, your inner ear via the labyrinthine artery (a branch of the anterior inferior cerebellar artery in most people).
On the way out, your internal jugular veins drain blood from the brain back down through the neck, passing right alongside the upper cervical structures. There is also a less-discussed but increasingly studied cerebrospinal fluid (CSF) drainage pathway that runs along the upper cervical spine through both the lymphatic system and venous plexuses.
Now imagine — and we see this in our 3D CBCT imaging in our office every day — that the top two bones of your spine are slightly out of alignment. Maybe it happened in a car accident on I-75 ten years ago. Maybe it was a fall off a paddleboard in Sarasota Bay. Maybe it was a sports injury in high school. Maybe it was a difficult birth. The misalignment may be small — just a few degrees, just a few millimeters — but it sits in the most neurologically dense and vascularly important real estate in your entire body.
The result can be irritation of the cranial nerves and upper cervical nerves, altered blood flow into the brainstem, impaired venous and lymphatic drainage from the head, and disruption of the autonomic regulation that keeps your inner ear fluid balance, well, balanced. Is it any wonder that some patients with chronic inner ear problems start to improve dramatically when this area is corrected?
The Upper Neck: The Most Overlooked Piece of the Ménière’s Puzzle
Let’s be very clear about something. We are not telling you that Ménière’s disease is a chiropractic condition or that a misaligned vertebra is the only possible cause. That would be irresponsible. Ménière’s is genuinely complex, and we believe in working alongside ENT physicians, neurologists, audiologists, and primary care doctors — not against them.
What we are saying is this: in our experience seeing patients in Sarasota for more than a decade, the upper cervical spine is the most consistently overlooked structure in the workup of Ménière’s disease and Ménière-like conditions. When it is misaligned and interfering with the brainstem, the inner ear, and the surrounding vascular and lymphatic structures, we frequently see a corresponding pattern of symptoms — and we frequently see those symptoms improve when the alignment is restored.
There are a few specific mechanisms that may explain this:
Brainstem irritation and the vestibular nuclei. Your vestibular nuclei — the brainstem hubs that process inner ear signals — sit at the floor of the fourth ventricle, directly behind the upper cervical region. Even subtle mechanical irritation in this area can alter how those nuclei interpret incoming balance information, contributing to chronic dizziness, motion sensitivity, and a heightened sense of imbalance between attacks.
Autonomic dysregulation. The vagus nerve and the upper cervical sympathetic chain both influence vascular tone and fluid regulation. Disruption here may contribute to the fluid pressure changes inside the inner ear that we see in endolymphatic hydrops. We have written extensively about this in our page on Vagus Nerve Dysfunction, and it is one of the most underappreciated systems in chronic illness.
Eustachian tube dysfunction. The Eustachian tube, which equalizes pressure between the middle ear and the back of your throat, is influenced by muscles and nerves that arise from this region. Persistent dysfunction here can mimic or worsen the aural fullness that defines Ménière’s. (For more, see our page on Eustachian Tube Dysfunction.)
Venous and lymphatic drainage. Newer research is showing that fluid drainage from the head matters enormously in conditions ranging from migraine to multiple sclerosis to vestibular disorders. When the upper neck is misaligned, drainage can be physically restricted.
What Upper Cervical Chiropractic Care at Lavender Family Chiropractic Actually Looks Like
If you have been to a traditional chiropractor before, please understand that what we do at Lavender Family Chiropractic is fundamentally different. There is no twisting. No cracking. No popping. No general spinal manipulation.
Our doctors, Dr. Rusty Lavender and Dr. Jacob Temple, are specifically trained in the Advanced HIO Knee Chest Upper Cervical Technique (AHKC) — one of the most precise and gentle forms of chiropractic care in existence. We focus exclusively on the relationship between the top two bones of your spine (C1 and C2) and the brainstem they protect.
Before we ever touch your spine, we use 3D Cone Beam CT (CBCT) imaging to measure the position of your upper cervical vertebrae down to one one-hundredth of a millimeter. This is not guesswork. This is engineering. We calculate a specific correction formula tailored to your unique anatomy and the precise nature of your misalignment.
We also use paraspinal infrared thermography to objectively measure how your nervous system is functioning, and we re-measure regularly so we can prove — to you and to ourselves — that the corrections are holding and that your body is healing.
The correction itself is so gentle that many patients say they barely feel it happen. There is no force. There is no torque. Just a precise, low-impact touch designed to restore proper alignment and let your body do what it was always designed to do: heal itself.
What to Expect on Your First Visit
If you decide to come see us, here is what your journey looks like:
Step 1: Complimentary Consultation. This is a no-pressure conversation where we listen to your story, review what you have already been through, and tell you honestly whether we think we can help. If we don’t think we can, we will tell you that too.
Step 2: Full Examination and 3D Imaging. If we agree to move forward, we perform a detailed neurological exam, postural assessment, and 3D CBCT imaging to see exactly what is happening in your upper cervical spine.
Step 3: Report of Findings. We sit down with you and walk you through your scans, your findings, and a customized care plan designed for your specific situation.
Step 4: First Correction and Follow-Up. Your first correction is gentle, precise, and based on the unique formula calculated from your imaging. We monitor your progress carefully with scans, thermography, and ongoing assessment.
You can read more about this entire process on our What To Expect page.
Ready to See If Upper Cervical Care Can Help Your Ménière’s?
If you are tired of the spinning, the roaring, the fullness, and the fear of when the next attack will hit — we want to talk with you. Schedule your complimentary consultation today by calling (941) 243-3729 or booking online here. There is hope, and healing starts here.
What Does the Research Say About Upper Cervical Care and Inner Ear Conditions?
We want to be transparent: large-scale randomized controlled trials on upper cervical chiropractic care for Ménière’s disease specifically are still limited. But the existing case series, pilot studies, and clinical reports are extremely encouraging, and they line up beautifully with what we see in practice every single week.
In one of the most-referenced case series in the field, Dr. Michael Burcon documented dozens of patients with Ménière’s disease who had a history of head or neck trauma and who showed significant improvement in vertigo episodes, tinnitus, and hearing function after upper cervical correction. The pattern was striking: many of these patients had been suffering for years, had tried multiple medications and interventions, and had been told nothing more could be done — and yet they got better after addressing the upper cervical spine.
Other research has examined cerebrospinal fluid flow and venous drainage in relation to inner ear function, and there is growing recognition in vascular neurology that the upper neck plays a meaningful role in head and ear physiology. The pieces are coming together.
We always tell our patients the truth: we cannot promise outcomes, and not every person with Ménière’s will respond to upper cervical care. But the people who do respond often respond dramatically — and we have seen many of them. The only way to know if you are one of them is to be properly evaluated.
Lifestyle Factors That Make Ménière’s Worse (or Better)
Even as we work to address the structural side of things, there are lifestyle factors that matter enormously in Ménière’s disease. Most patients we see have already heard some of this from their ENT, but here is a synthesis of what tends to actually help:
Sodium intake. This is the most consistent recommendation across all of Ménière’s care. Excess sodium can worsen fluid retention in the inner ear, so most clinicians recommend keeping daily intake under 1,500 mg. This often means cooking at home, reading labels carefully, and being especially mindful of restaurant meals and packaged foods — even ones that don’t taste particularly salty.
Caffeine. Caffeine is a vasoconstrictor and a stimulant, and many Ménière’s patients find that even modest amounts can trigger attacks. We generally recommend trying a complete elimination for a few weeks to see what happens.
Alcohol. Alcohol affects inner ear fluid dynamics and is a known trigger for vertigo episodes in susceptible individuals. Most Ménière’s patients do better avoiding it entirely.
Stress and sleep. The autonomic nervous system plays a huge role in inner ear regulation, and chronic stress is one of the most powerful disruptors of autonomic function we know. Building in real recovery — sleep, time outdoors, deep breathing, gentle movement — can make an enormous difference.
Hydration. Counterintuitive, perhaps, but consistent hydration helps stabilize fluid balance throughout the body, including the inner ear.
MSG, aspartame, and processed foods. Many patients report that artificial additives, particularly MSG and aspartame, can trigger or worsen attacks. Whole food diets tend to work best.
Weather and barometric pressure. Living in Sarasota, you already know how dramatically the pressure can shift, especially around summer storms and hurricane season. If you find your symptoms get worse with weather changes, you are not imagining it — and you may also want to read our blog The World Won’t Stop Spinning: PPPD and the Upper Neck Connection for related insights on persistent dizziness conditions that share some of the same neurological pathways.
Why Sarasota Patients Choose Lavender Family Chiropractic
Our office is located at 5899 Whitfield Avenue, Suite 107, in Sarasota, FL 34243 — right at the corner of University and Whitfield. We are easily accessible from across the region, and we proudly serve patients from Sarasota, Bradenton, Lakewood Ranch, Venice, Osprey, Nokomis, Siesta Key, Longboat Key, Palmetto, Parrish, Ellenton, Myakka, North Port, and beyond. For a full list of the communities we serve, please visit our Areas We Service page.
Patients come to us because we offer something genuinely different in the world of healthcare:
- Precision. We don’t guess. Every correction is based on measurable, repeatable data from 3D imaging and thermography.
- Gentleness. No twisting, no popping, no force.
- Specialty Training. Our doctors are AHKC-trained and continually pursue ongoing education in upper cervical care.
- Compassion. We have walked alongside thousands of patients who came in feeling hopeless. We listen, we educate, and we genuinely care about your story.
We don’t believe in the “one-size-fits-all” approach. We believe your body is incredibly intelligent and has an extraordinary capacity to heal when the interference is removed.
The Top 15 Questions We Get About Ménière’s Disease and Upper Cervical Care
How is Ménière’s disease officially diagnosed?
Ménière’s is diagnosed primarily by clinical history. The current criteria from the American Academy of Otolaryngology–Head and Neck Surgery require at least two spontaneous episodes of vertigo lasting 20 minutes to 12 hours, audiometrically documented fluctuating low-to-mid frequency sensorineural hearing loss in the affected ear, and fluctuating aural symptoms (hearing changes, tinnitus, or fullness) in the affected ear, with other causes ruled out. An ENT and an audiologist typically lead this diagnostic workup.
Is Ménière’s disease the same thing as vertigo?
No. Vertigo is a symptom — the sensation that you or the world is spinning — and it can be caused by many different conditions. Ménière’s is one specific cause of vertigo, defined by the combination of vertigo plus hearing changes, tinnitus, and aural fullness. Other causes of vertigo include BPPV, vestibular neuritis, vestibular migraine, PPPD, MdDS, and craniocervical instability. Our main vertigo blog walks through these distinctions in more detail.
Can Ménière’s disease go away on its own?
The natural history is variable. Some patients have a few attacks and then improve. Others have decades of fluctuating symptoms. Many eventually develop progressive hearing loss in the affected ear. There is no reliable way to predict which path a given patient will follow, which is part of why early, comprehensive care matters.
Will I lose my hearing permanently?
Hearing loss in Ménière’s is often fluctuating at first but tends to become more permanent over time, particularly if attacks are frequent and uncontrolled. Protecting your hearing is one of the strongest reasons to seek thorough care early and to address every contributing factor — including the structural ones.
Can stress trigger Ménière’s attacks?
Yes. Stress is one of the most commonly reported triggers, and the connection makes biological sense: stress profoundly affects autonomic nervous system regulation, vascular tone, and fluid balance — all of which are central to inner ear function.
What’s the difference between Ménière’s disease and vestibular migraine?
This is one of the most common diagnostic challenges in vestibular medicine. Both conditions cause episodic vertigo, both can include auditory symptoms, and they can even occur together in the same patient. Vestibular migraine typically lacks the persistent unilateral hearing loss and aural fullness of Ménière’s and tends to follow migraine patterns more closely. We have a dedicated page on Vestibular Migraine if you want to dig deeper.
Can a car accident cause Ménière’s disease?
It is not officially classified as a cause, but there is strong clinical and case-series evidence that head and neck trauma can either trigger or worsen Ménière’s-like symptoms, likely through the upper cervical mechanism we have discussed in this article. Many of our Ménière’s patients can identify a specific traumatic event — sometimes years before symptoms began.
Is upper cervical chiropractic safe?
Yes. The Advanced HIO Knee Chest technique we use is one of the gentlest forms of chiropractic care in existence. There is no twisting, no popping, no general manipulation. Corrections are precise and low-force, and they are guided by detailed imaging.
How long before I notice improvement?
This varies tremendously from patient to patient. Some people notice improvements within the first few visits. Others take weeks or months. The body heals at its own pace, and chronic conditions like Ménière’s often require patience and a true care plan, not a quick fix.
Will I have to come forever?
No. We design care plans with the goal of getting you healthy and helping you maintain that health. Many patients transition to a maintenance schedule once they are stable.
Do you accept insurance?
We do not bill insurance directly, but we keep our care affordable and transparent, and we offer customized care plans designed to fit different budgets. Please call our office at (941) 243-3729 to discuss specifics.
What if I’ve already tried other treatments and they didn’t work?
You are exactly the kind of patient we see most. Many of our patients have already tried medications, vestibular rehabilitation, dietary changes, and even more invasive interventions before they find us. We are honest about whether we can help, and we welcome a conversation.
Can children develop Ménière’s disease?
It is rare in children, but pediatric vertigo and dizziness do exist and can have their own causes, including upper cervical issues from birth trauma or sports injuries. We do see pediatric patients, and we adapt our approach accordingly.
Is Ménière’s hereditary?
There is some genetic component identified in research, but most cases appear sporadic. Family history may be a factor, but it is not destiny.
What’s the first step if I want to see if you can help me?
Call our office at (941) 243-3729 or schedule a complimentary consultation online. We will listen to your story, answer your questions, and tell you honestly whether we believe upper cervical care can help your specific case.
Final Thoughts: There Is Hope
If you have read this far, we want you to know something important.
You are not crazy. You are not making it up. You are not weak for being exhausted by this. Ménière’s disease is a real, debilitating, life-altering condition that has stolen too much from too many people in our community. And the conventional approach — medications, low-salt diets, and waiting it out — is not the only path forward.
The upper cervical spine is one of the most overlooked structures in modern medicine, and yet it sits at the precise crossroads of nervous system function, brainstem integrity, vascular flow, and inner ear regulation. When it is restored to proper alignment, the body can finally do what it was designed to do — heal.
We would be honored to be part of your story. Whether you ultimately become a patient or not, we hope this article has given you a clearer picture of what may be happening and what is possible.
Call us today at (941) 243-3729 or book your complimentary consultation online. Your healing journey can start now.
Related Articles
Lavender Family Chiropractic 5899 Whitfield Avenue, Suite 107 Sarasota, FL 34243 Phone: (941) 243-3729 Book Your Complimentary Consultation