Published by Lavender Family Chiropractic | Sarasota, Florida | Upper Cervical Care
PPPD: You wake up and the ground feels like it’s moving. You walk into a grocery store and the fluorescent lights and busy aisles make your brain feel like it’s short-circuiting. You drive across the Ringling Bridge and the visual motion of the water, the road, and the sky sends your nervous system into a tailspin. You’ve had every scan, every test, every specialist appointment — and they all come back normal. But you don’t feel normal. You feel like your body is permanently stuck in a state of motion, even when you’re completely still.
If this sounds familiar, you may be living with Persistent Postural-Perceptual Dizziness — a chronic vestibular condition known in the medical community as PPPD. At Lavender Family Chiropractic in Sarasota, Florida, we see patients from throughout the Gulf Coast who have been suffering for months or even years with this deeply disorienting condition, often without ever receiving a clear explanation for what is happening inside their nervous system. What most of these patients haven’t been told — and what most of their doctors haven’t explored — is that the upper cervical spine may be playing a central role in why their brain cannot find its footing.
This blog is for anyone in Sarasota, Bradenton, The Meadows, Palm Aire, University Park, or anywhere in between who is tired of being dizzy, tired of being dismissed, and tired of being told everything looks fine when nothing feels fine. There is a neurological explanation for what you’re experiencing, and there is a precise, gentle form of care that may finally give your brain and body the stability they’ve been searching for.
What Is Persistent Postural-Perceptual Dizziness (PPPD)?
Persistent Postural-Perceptual Dizziness is a chronic functional vestibular disorder characterized by ongoing dizziness, unsteadiness, and/or non-spinning vertigo that lasts for three months or more. The condition was formally defined and named by the Bárány Society in 2017, which means that for many years before that, patients were either misdiagnosed, told their symptoms were anxiety-related, or given no diagnosis at all. Even today, the condition remains widely underrecognized, and many patients spend years cycling through neurologists, ENTs, cardiologists, and therapists before receiving a clear explanation for what they’re experiencing.
The hallmark features of this condition are distinctive. The dizziness is persistent — present on most days for at least three months — and it is not the spinning sensation most people associate with vertigo. Instead, it tends to be a constant sense of rocking, swaying, floating, or unsteadiness, as though the ground beneath you is unreliable. This feeling may be mild on some days and debilitating on others, but it rarely goes away completely.
Two specific factors reliably worsen symptoms, and both are central to understanding the condition. The first is upright posture and active movement. Simply being on your feet, walking, turning your head, or changing positions tends to amplify dizziness significantly. The second is exposure to complex visual environments — busy patterns, moving crowds, scrolling on screens, driving, grocery stores with their endless visual stimulation, or even watching television. These environments overwhelm a nervous system that has lost its ability to integrate sensory information accurately, and the result is a spike in dizziness, brain fog, anxiety, and disorientation.
This type of persistent dizziness typically begins after a triggering event. The trigger is most commonly an inner ear disorder such as benign paroxysmal positional vertigo (BPPV), vestibular neuritis, or Ménière’s disease. But it can also be triggered by a concussion, a prolonged illness, a panic attack, a period of extreme stress, or even a car accident. The acute event resolves — or is treated — but the nervous system never fully resets. Instead, it becomes locked in a state of heightened vigilance, perpetually scanning for danger signals that have long since passed. This is not a disease of the inner ear. It is a disorder of how the brain processes and integrates balance and spatial information — and that distinction matters enormously when it comes to treatment.
Persistent Dizziness Is a Nerve and Sensory Processing Condition
To understand why upper cervical chiropractic care can be deeply relevant to chronic dizziness and sensory overload, we need to understand the neurological machinery underlying the condition — and why the upper neck sits at the very center of that machinery.
How the Brain Maintains Balance
Your sense of balance and spatial orientation is not produced by a single organ. It is the result of three interlocking sensory systems working in constant communication with each other and with the brainstem. The first system is the vestibular system — the semicircular canals and otolith organs of the inner ear, which detect rotational movement, head tilt, and linear acceleration.
The second is the visual system, which provides moment-to-moment information about your position relative to the environment. The third — and most frequently overlooked in discussions of dizziness — is the proprioceptive system, the network of mechanoreceptors in your joints, muscles, and particularly your neck and upper spine, which tell the brain where your body is in space.
Under normal circumstances, these three systems agree with each other, and the brain synthesizes their signals into a seamless, stable experience of being oriented and grounded. When there is conflict or inconsistency between these signals — or when one of the systems is damaged or disrupted — the brain struggles to make sense of the contradictions.
In chronic functional dizziness, the brain has developed a maladaptive strategy for dealing with this conflict: it becomes hypervigilant, over-relying on visual input while simultaneously becoming hypersensitive to any motion or sensory stimulation. The result is a nervous system that is stuck in a state of perpetual alarm.
The Role of the Cervical Spine in Balance and Spatial Orientation
Here is where the upper cervical spine becomes critically important. The neck — and particularly the upper cervical region spanning the atlas (C1) and axis (C2) — contains the highest concentration of proprioceptive nerve endings of any segment of the spinal column. The facet joints, muscles, and ligaments at the craniocervical junction are densely packed with mechanoreceptors that feed a continuous stream of positional and movement information directly to the brainstem and cerebellum.
This input is not peripheral or supplementary. It is foundational. The cervical proprioceptive system works in close coordination with the vestibular system — so much so that researchers have identified direct neural pathways between the cervical mechanoreceptors and the vestibular nuclei in the brainstem. When the upper cervical spine is misaligned, these proprioceptive signals become distorted or dysregulated.
The brain receives faulty positional information from the neck while simultaneously receiving accurate signals from the inner ear and eyes — and the resulting mismatch is precisely the kind of sensory conflict that drives persistent dizziness and sensory overload.
This connection is further supported by the well-documented phenomenon of cervicogenic dizziness — dizziness that originates from dysfunction in the cervical spine rather than the inner ear. Research has shown that cervical dysfunction, particularly at the upper cervical levels, can produce dizziness, unsteadiness, visual disturbance, and postural instability that closely mimics vestibular disorders. In many chronic dizziness patients, cervicogenic dysfunction is not just a contributing factor — it may be the primary driver that prevented the nervous system from resetting after the original triggering event.
The Brainstem Connection
The brainstem is the command center for everything related to balance, spatial orientation, autonomic function, and sensory integration. It houses the vestibular nuclei, the cerebellum’s relay stations, and the neural pathways that coordinate the interaction between your inner ear, your eyes, and your proprioceptive system. The brainstem also plays a key role in regulating the autonomic nervous system — the system that governs your body’s threat response, arousal level, and stress reactivity.
The atlas and axis sit in direct anatomical relationship with the brainstem. A misalignment at C1 or C2 — even a subtle one that would not show up as anything dramatic on a standard MRI — can create mechanical pressure or irritation at the craniocervical junction that disrupts brainstem function. For a patient whose brainstem is already operating in a state of dysregulated hypervigilance, this additional structural stress can be the difference between a nervous system that can gradually recalibrate and one that simply cannot find its way back to equilibrium.
To learn more about how dysfunction at the upper cervical spine contributes to dizziness and vestibular symptoms, visit our dedicated Vertigo page — the neurology overlaps significantly with chronic functional dizziness and sensory processing disorders.
The Upper Neck: Your Body’s Most Critical Junction
The upper cervical spine is unlike any other region of the body. The atlas — the first cervical vertebra — has no disc above it and sits in direct articulation with the base of the skull, allowing the head to nod. The axis below it features the odontoid process, a bony projection around which the atlas rotates, enabling you to turn your head left and right. This extraordinary design allows for unparalleled range of motion. But that same design makes the upper cervical region exceptionally vulnerable to misalignment.
Falls, whiplash injuries, concussions, birth trauma, contact sports, poor sleep posture, and years of looking down at phones and screens can all shift the atlas or axis out of their optimal position. When this happens — an upper cervical subluxation — the structural distortion affects not just the bones themselves but the soft tissues, nerve pathways, and vascular structures in their immediate vicinity.
The vertebral arteries, which pass through the transverse foramina of the cervical vertebrae on their way to supply blood to the brainstem and cerebellum, can be affected by upper cervical misalignment. So can the vagus nerve, which exits near the atlas and carries parasympathetic signals throughout the body.
For patients with persistent dizziness and sensory overload, the significance of all of this is hard to overstate. If the proprioceptive signals from the upper neck are distorted due to a structural misalignment, the sensory mismatch that the brain is trying to resolve will never fully resolve — because the faulty input is still being generated at every moment.
The brain cannot recalibrate based on signals it cannot trust. Correcting the atlas misalignment removes that source of faulty input, giving the brainstem the accurate proprioceptive data it needs to begin the process of genuine neurological reorganization.
Why Traditional Care Often Misses This
Chronic functional dizziness is most commonly managed through a combination of vestibular rehabilitation therapy, cognitive behavioral therapy, and medication — typically SSRIs or SNRIs, which modulate the central sensitization underlying the condition. All of these approaches have merit and can be genuinely helpful. But none of them address the possibility that the brainstem is receiving structurally distorted proprioceptive signals from a misaligned upper cervical spine.
Vestibular rehabilitation works to retrain the brain’s balance processing through specific exercises and movement patterns. But if the upper neck is generating inaccurate input throughout the rehabilitation process, the brain is essentially trying to recalibrate using corrupted data. Progress may be slow, incomplete, or easily undone. This is a frustrating pattern that many patients recognize — they improve somewhat with vestibular therapy, then regress, then improve again, never quite achieving the stable baseline they’re hoping for.
Upper cervical chiropractic care offers something that no other treatment for chronic dizziness currently addresses: the correction of structural dysfunction at the craniocervical junction that may be perpetuating the sensory mismatch at the root of the condition.
It does not replace vestibular rehabilitation or psychological support — but for many patients, it is the missing piece that allows those other therapies to finally work as intended. You can read more about the upper cervical approach and why it’s different from conventional chiropractic on our Why Upper Cervical page.
Upper Cervical Chiropractic Care: What Makes It Different
Upper cervical chiropractic is a highly specialized field within chiropractic medicine that focuses exclusively on the relationship between the atlas, the axis, and the brainstem. It is fundamentally different from general chiropractic care in its philosophy, its diagnostic precision, and its treatment approach.
General chiropractic care often involves manipulation of multiple spinal segments with audible adjustments — the familiar cracking sound that most people associate with chiropractic. Upper cervical care involves none of that. There is no twisting, no cracking, no forceful manipulation of the neck.
Instead, the practitioner uses precise, low-force corrections calculated based on detailed imaging of the individual patient’s craniocervical anatomy. The adjustment is so gentle that many patients barely feel it — and yet the neurological effects can be profound, because the correction is delivered with pinpoint accuracy to the most neurologically significant region of the spine.
At Lavender Family Chiropractic, we use the Advanced HIO Knee Chest Upper Cervical Technique (AHKC), a specific and highly refined upper cervical protocol that allows us to deliver precise corrections based on each patient’s unique anatomy and misalignment pattern. No two patients receive the same adjustment — because no two patients have the same spine.
What to Expect at Lavender Family Chiropractic
When you come to Lavender Family Chiropractic with persistent dizziness and sensory overload symptoms, your first visit begins with a comprehensive consultation and health history. We want to understand your full story — when your dizziness began, what triggered it, what makes it better or worse, what treatments you’ve already tried, and how it is affecting your daily life here in Sarasota. For many of our patients, this is the first time a healthcare provider has asked them to describe all of these factors together, and it often produces important clinical insights.
We then conduct a neurological and postural assessment, looking for objective signs of upper cervical involvement. This includes evaluating leg length discrepancy in the prone position, postural imbalance, ranges of cervical motion, and paraspinal temperature asymmetry using infrared thermography — a highly sensitive tool for detecting neurological interference at the spinal level. These findings help us determine whether upper cervical subluxation is present and whether your presentation is consistent with a structural contribution to your symptoms.
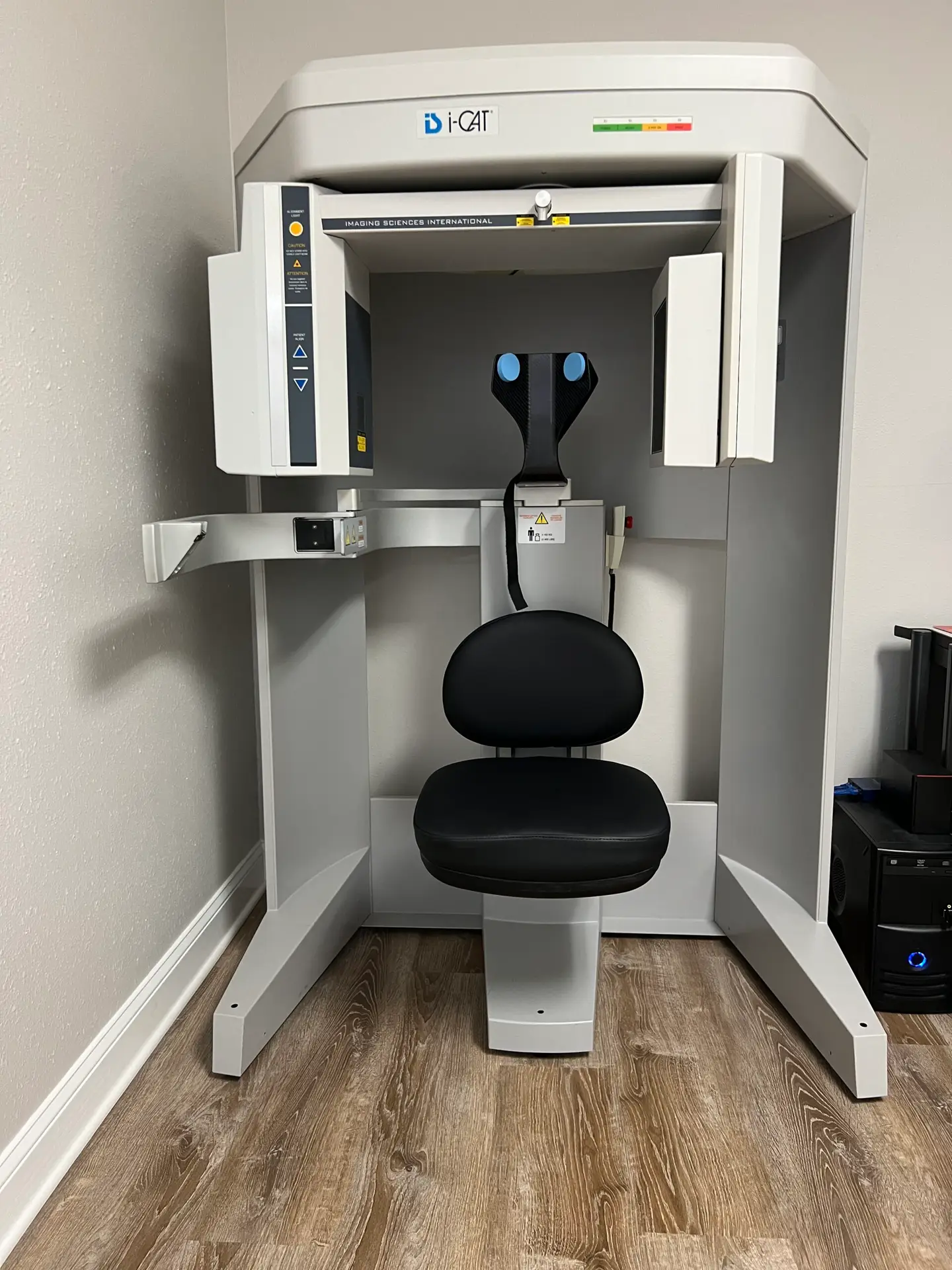
If the assessment indicates upper cervical involvement, we obtain precision 3D cone beam CT imaging of your upper cervical spine. This technology allows us to see the exact three-dimensional geometry of your atlas and axis — their precise position, angle, and relationship to each other and to the skull — in a level of detail that standard X-rays simply cannot provide. From this imaging, we calculate a correction formula that is specific to your anatomy, not a general protocol. Every adjustment is built from your images.
After your first correction, we allow time for your nervous system to begin responding. Chronic functional dizziness involves central sensitization — a rewiring of the brain’s threat-detection system — and meaningful improvement takes time. Most patients begin noticing subtle shifts within the first few weeks of care: perhaps the dizziness is slightly less constant, the bad days are less severe, or the visual sensitivity is beginning to ease. Over a course of several months, as the atlas holds its corrected position and the brainstem receives consistent, accurate proprioceptive input, many patients experience significant and lasting improvement in their symptoms.
We want to be honest with you: upper cervical care is not a quick fix, and it is most effective as part of a broader care plan that may include vestibular rehabilitation and psychological support. But for patients who have been stuck in the cycle of chronic dizziness without sustained improvement, it may be the structural piece that finally allows everything else to work. You can find out exactly what to expect as a new patient on our What to Expect page.
Are You Ready to Take a Different Approach?
If you’ve been living with persistent dizziness, rocking sensations, visual sensitivity, and the exhausting unpredictability of chronic vestibular dysfunction — and you haven’t had your upper cervical spine evaluated — we’d love to have that conversation with you. A complimentary consultation at Lavender Family Chiropractic costs you nothing but an hour of your time, and it may change your understanding of why your nervous system has been struggling to find its balance.
Schedule Your Free Consultation at Lavender Family Chiropractic
Evidence and Emerging Research
The evidence base for upper cervical chiropractic care in vestibular and balance disorders has grown meaningfully in recent years. Research connecting cervical proprioception, brainstem function, and chronic dizziness is well-established and continues to develop.
Studies examining cervicogenic dizziness have consistently demonstrated that dysfunction in the upper cervical spine produces measurable disturbances in balance, spatial orientation, and gaze stabilization. Research published in journals including the Journal of Vestibular Research and Manual Therapy has shown that cervical manipulation — particularly at the upper cervical levels — produces significant improvements in dizziness, postural stability, and associated headache. These effects are attributed to the normalization of cervical proprioceptive input and the reduction of mechanical tension on brainstem structures.
Research on central sensitization — the neurological mechanism at the heart of chronic functional dizziness — has demonstrated that spinal manipulation can reduce central sensitization indices, modulate pain and threat-processing pathways in the brain, and shift the autonomic nervous system toward parasympathetic dominance. For a patient whose nervous system is chronically over-activated, this shift toward parasympathetic tone is precisely what is needed to begin unwinding the hypervigilance that sustains the condition.
Case reports from upper cervical practices across the country have documented meaningful improvement in chronic vestibular dysfunction following atlas correction — including reductions in dizziness frequency and severity, improved tolerance for visually complex environments, decreased sensitivity to motion, and improved overall quality of life. While individual case reports do not constitute clinical proof, they are consistent with the neuroanatomical reasoning described throughout this blog and with what our team observes clinically at Lavender Family Chiropractic.
It is important to acknowledge that chronic functional dizziness is a complex, multifactorial condition, and that results vary significantly between individuals. Patients with a clear structural component — measurable atlas misalignment on imaging, cervicogenic features in their presentation, or a history of trauma that could plausibly have created upper cervical dysfunction — tend to respond most favorably to upper cervical care. This is why a thorough evaluation is so important before beginning any treatment plan.
Lifestyle Factors That Complement Upper Cervical Care
While upper cervical corrections address the structural driver of sensory mismatch at the craniocervical junction, there are lifestyle and self-care strategies that can meaningfully support your recovery as your nervous system recalibrates.
Gradually expose yourself to challenging environments rather than avoiding them.Avoidance is one of the key mechanisms that perpetuates chronic dizziness. When you avoid busy stores, driving, or screens because they trigger symptoms, the brain learns that these environments are dangerous and becomes even more sensitized to them over time. Working with a vestibular rehabilitation therapist on gradual, structured exposure is one of the most evidence-based approaches for breaking this cycle, and it complements upper cervical care beautifully once the structural component has been addressed.
Prioritize consistent, restorative sleep. The brain’s ability to recalibrate sensory processing is heavily dependent on sleep quality. During deep sleep, the brain consolidates new movement patterns, processes residual sensory conflict, and regulates the autonomic nervous system. Poor sleep — which is extremely common in chronic dizziness patients due to the anxiety and hyperarousal the condition creates — significantly slows neurological recovery. Maintaining a consistent sleep schedule, reducing screen exposure before bed, and optimizing your sleep position to minimize upper cervical tension all support the recovery process.
Manage screen time and visual load thoughtfully. Scrolling on phones, working at computers, and watching fast-moving content are among the most common triggers for sensory overload. This doesn’t mean eliminating screens — which is neither practical nor necessary — but it does mean taking regular breaks, using blue-light filtering settings, and being intentional about how much visual stimulation you expose yourself to during periods of symptom flare.
Support your nervous system with breathing and mindfulness practices. The anxiety and chronic dizziness connection is real — not because the dizziness is imagined, but because the autonomic dysregulation driving the condition overlaps significantly with the physiological state of chronic stress.
Slow, diaphragmatic breathing activates the vagus nerve and shifts the nervous system toward parasympathetic dominance, directly counteracting the hypervigilance that sustains chronic dizziness. Even five to ten minutes of intentional breathing practice daily can produce measurable changes in autonomic tone over time.
Stay active with low-provocation movement. Walking — particularly in calm outdoor environments like the trails at Myakka River State Park, the quieter paths through The Meadows neighborhood, or along the calmer stretches of Siesta Key Beach — provides gentle vestibular and proprioceptive input without the overwhelming visual complexity of indoor environments. Regular low-impact movement supports neurological recovery and helps prevent the deconditioning that worsens symptoms over time.
Many of our patients with chronic dizziness are surprised to discover that their vestibular symptoms coexist with other upper cervical patterns they hadn’t connected — persistent headaches at the base of the skull, neck tension, or a history of vestibular migraines. If that resonates with you, our blog on Natural Migraine Relief in Sarasota explores how these conditions share a common neurological root and why addressing the upper cervical spine helps across all of them.
Serving Sarasota and the Surrounding Gulf Coast
At Lavender Family Chiropractic, we serve patients with chronic dizziness, vestibular disorders, and sensory processing dysfunction from communities throughout the Sarasota region and the broader Gulf Coast. Our location on Whitfield Avenue puts us conveniently close to some of the most established neighborhoods in the area, and we see patients from across a wide geographic range every single week.
Right here close to our office, we regularly see patients from The Meadows, Palm Aire, University Park, University Country Club, DeSoto Acres, and Whitfield Estates — neighborhoods that are just minutes from our front door. From a bit further out we welcome patients from Lakewood Ranch, Waterside, Lorraine Lakes, and the growing communities of northeast Sarasota County. We also see patients from Gulf Gate Estates, Siesta Key, Palmer Ranch, South Gate, and Bee Ridge throughout Sarasota proper, as well as from Osprey, Nokomis, Venice, Englewood, Bradenton, and Longboat Key across the broader region.
Living with chronic dizziness in Sarasota presents its own unique challenges. The Gulf Coast lifestyle — driving across bridges with expansive water views, navigating the visual busyness of St. Armands Circle, walking the bright open spaces of downtown Sarasota, or simply getting through a trip to the UTC mall — can be genuinely overwhelming for a nervous system in this state. We understand this, and we work with our patients to build a care plan that fits their real daily lives in this community.
Our practice is located at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243. A full list of the communities we serve is available on our Areas We Service page.
We know that getting to a new provider can feel daunting when every car ride and every unfamiliar environment is a potential trigger. We want you to know that our office is calm, low-stimulation, and designed with exactly that in mind. From the moment you walk in, you’re in a space built for people whose nervous systems need gentleness and care.
Is Upper Cervical Care Right for You?
Chronic persistent dizziness can steal your life in ways that are difficult to explain to anyone who hasn’t experienced it. It’s not dramatic in the way a spinning vertigo attack is dramatic — but its relentless, day-after-day presence, the way it makes ordinary environments feel threatening and ordinary activities feel exhausting, is a profound burden. Many of our patients describe it as lonelier than any condition they’ve ever dealt with, because it’s invisible, often dismissed, and deeply misunderstood.
You deserve a healthcare team that takes your symptoms seriously, investigates them thoroughly, and offers you more than symptom management as a long-term plan. At Lavender Family Chiropractic, we approach chronic vestibular dysfunction with genuine curiosity about what is driving your individual presentation — and a specific, evidence-informed tool for addressing one of the most commonly missed structural drivers of the condition.
We have seen patients who had all but given up on feeling better begin to reclaim their lives after upper cervical care — walking into grocery stores without dreading the experience, driving without white-knuckling the wheel, sitting in bright restaurants without feeling like the room is moving. We would love to be part of that journey for you.
Schedule Your Free Consultation | (941) 243-3729
Related Articles from Our Blog
Natural Migraine Relief in Sarasota, Florida Vestibular migraine is one of the most common triggers for chronic persistent dizziness, and the two conditions frequently co-exist. This post explores the neurological overlap between migraine, dizziness, and upper cervical dysfunction — and how addressing the atlas provides relief for both.
Head Pressure Relief in Sarasota Florida: The Craniocervical Junction, CSF Flow, and Proven Results Many patients with chronic dizziness also experience a persistent sense of pressure or fullness in the head alongside their vestibular symptoms. This blog dives deep into the craniocervical junction, cerebrospinal fluid dynamics, and how upper cervical corrections restore normal flow and function at this critical crossroads.
Natural Chiropractic Care in Sarasota and Lakewood Ranch: A Root-Cause Approach to Healing If chronic dizziness has you searching for a natural, non-pharmaceutical path forward, this is the place to start. We explain what root-cause chiropractic care actually means, how it differs from managing symptoms indefinitely, and why so many patients across the Gulf Coast are choosing this approach.
This blog is for informational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider for diagnosis and treatment of any health condition. Lavender Family Chiropractic | 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 | (941) 243-3729