Chiari Malformation: If you live in Sarasota, Lakewood Ranch, Bradenton, or anywhere along Florida’s Gulf Coast and you’ve been diagnosed with Chiari malformation, atlantoaxial instability (AAI), or both — you already know how isolating it can feel. The headaches that get worse when you cough or strain. The neck pain that no one can fully explain. The dizziness, the brain fog, the tingling in your hands, the feeling that your head is somehow “too heavy” for your neck. You’ve likely been told that surgery is the only real answer — or worse, that “nothing shows up on imaging” so there must not be a problem.
At Lavender Family Chiropractic, located at 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 (at the corner of University and Whitfield), we meet patients with these exact stories every week. Many of them have already seen neurologists, ENTs, vestibular therapists, and sometimes even neurosurgeons. Some have had decompression surgery and still don’t feel “right.” Others are trying to avoid surgery and want to know whether anything else could help.
This blog is for you. We’re going to walk through what Chiari malformation actually is, what atlantoaxial instability is, why the two are increasingly being recognized as overlapping conditions in the neurosurgical literature, what the research shows about correcting alignment at the craniocervical junction, and how gentle, precise upper cervical chiropractic care may serve as a meaningful piece of your healing puzzle.
This is also a companion piece to our most in-depth resource on the topic — When Your Head Feels Too Heavy: The Hidden Story of Craniocervical Instability, Vertigo, Neck Pain, and Migraines (and Why Upper Cervical Care May Be the Missing Link). If you haven’t read that yet, we strongly recommend it as the foundation for everything that follows here.
What Is Chiari Malformation?
Chiari malformation is a structural condition in which the lower portion of the cerebellum — specifically the cerebellar tonsils — descends below the foramen magnum, the large opening at the base of your skull where your brainstem becomes your spinal cord. In a normal anatomy, the cerebellum sits comfortably inside the posterior cranial fossa, and the foramen magnum is wide open for cerebrospinal fluid (CSF), the brainstem, and blood vessels to pass cleanly into the spinal canal.
In Chiari, that space is crowded. The tonsils herniate downward, and they can interfere with three critically important things:
- CSF circulation — the clear fluid that bathes the brain and spinal cord
- Brainstem function — the master control panel for autonomic regulation, balance, and cranial nerves
- Blood flow — including the vertebral arteries that supply the back of the brain
Chiari is classically divided into types. Chiari Type I is by far the most common and the one we see most often in our Sarasota office. It involves tonsillar descent (typically more than 3–5 mm below the foramen magnum) without other major brain malformations. Type II, III, and IV are progressively more severe and often diagnosed in infancy. According to a published case report and systematic review on Chiari pathogenesis, Type I involves displacement of the cerebellar tonsils caudally below the foramen magnum into the upper cervical canal without associated defects of the brainstem or supratentorial regions, while Types III and IV are associated with high morbidity and mortality (Mendis et al., Cureus, 2023 — PMC10656570).
Common symptoms of Chiari Type I include:
- Occipital headaches (back of the head), especially with coughing, sneezing, straining, or exertion
- Neck pain at the base of the skull
- Dizziness, vertigo, and balance problems
- Visual disturbances and ocular issues
- Ringing in the ears (tinnitus)
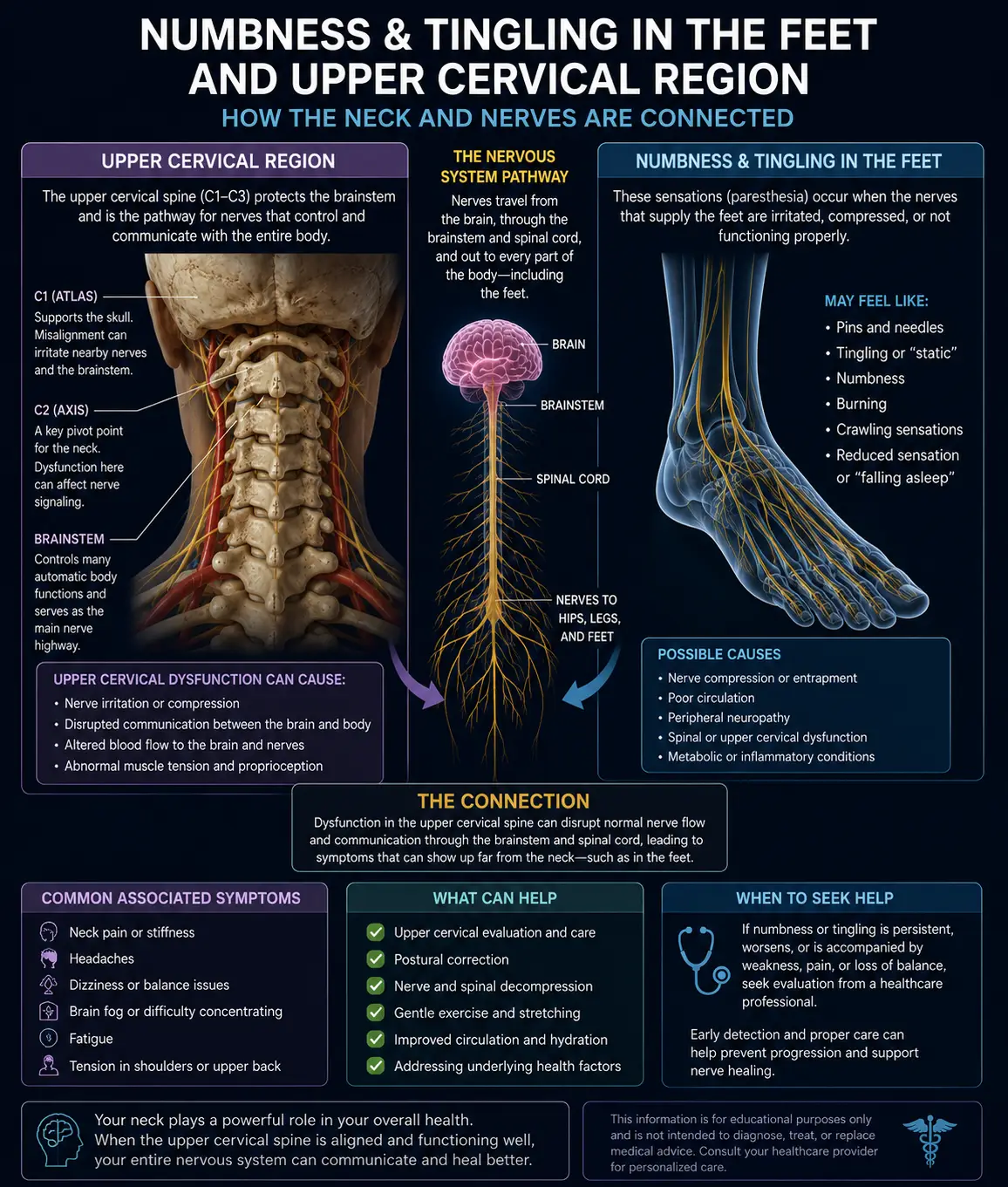
- Numbness or tingling in the hands or feet
- Difficulty swallowing
- Brain fog and cognitive complaints
- Sleep apnea and unrefreshing sleep
- Chronic fatigue
Approximately 80% of individuals with a Type I Chiari malformation have a chief complaint of neck pain, along with cerebellar dysfunction and ocular and otoneurologic disturbances (Lutter et al., Cureus — PMC10149087).
What Is Atlantoaxial Instability?
Now let’s look at the second piece of this puzzle. Atlantoaxial instability (AAI) refers to abnormal, excessive movement between the atlas (C1) and axis (C2) — the top two vertebrae of your spine. These two bones are unlike any others in your body. The atlas is a ring-shaped vertebra with no body and no spinous process. It cradles the skull. The axis sits directly below it and has a peg-shaped projection called the dens (or odontoid process) that fits up into the atlas, acting as a pivot for rotational movement.
Together, the atlas and axis form the atlantoaxial joint, which is responsible for about 50% of the rotation of your head. This region is held together not by interlocking bony architecture (like the rest of the spine) but by a complex network of ligaments — the transverse ligament, the alar ligaments, and the apical ligament being the most important. When those ligaments are stretched, torn, or congenitally lax, the joint can move more than it should, creating instability.
Common causes of atlantoaxial instability include:
- Trauma (whiplash, falls, sports injuries, head-first impacts)
- Congenital connective tissue disorders such as Ehlers-Danlos syndrome (EDS)
- Rheumatoid arthritis
- Down syndrome
- Congenital odontoid abnormalities
- Repetitive micro-trauma over a lifetime
Symptoms of AAI overlap heavily with Chiari and include occipital headaches, neck pain, dizziness, autonomic dysfunction, visual disturbances, dysphagia, “heavy head” sensation, and a host of cranial nerve symptoms.
The Hidden Overlap: Why Chiari and Atlantoaxial Instability Are Increasingly Being Studied Together
Here is where the conversation gets really interesting — and where modern neurosurgical research is challenging old assumptions.
For decades, the standard treatment for symptomatic Chiari malformation was posterior fossa decompression — a surgery in which the surgeon removes a portion of the back of the skull and the back of the C1 vertebra to create more room for the herniated tonsils. The theory: if the tonsils are crowded, make more space.
But here’s the problem. Posterior fossa decompression is unsuccessful in resolving headaches in 26-46% of cases (Cousins et al., medRxiv preprint, 2025). Nearly half of patients don’t get the relief they hoped for. Why?
A growing body of neurosurgical research suggests that in many Chiari patients, the real driver isn’t the tonsillar descent itself — it’s instability at the craniocervical junction, particularly atlantoaxial instability and basilar invagination. The tonsillar descent may be a consequence of underlying instability rather than the root cause.
Dr. Atul Goel’s Landmark Research
The most influential voice in this conversation has been Dr. Atul Goel, a neurosurgeon at King Edward VII Memorial Hospital in Mumbai, India. In a landmark study published in the Journal of Neurosurgery: Spine in 2015, Goel treated 65 patients with Chiari malformation using atlantoaxial fixation alone — no posterior fossa decompression. He proposed that atlantoaxial instability is the actual cause of Chiari malformation in many cases (Goel A., J Neurosurg Spine, 2015 — PMID: 25415487).
His findings were striking. Of the 65 patients, 55 had associated syringomyelia (a fluid-filled cyst in the spinal cord) and 46 had associated basilar invagination. After atlantoaxial stabilization — without ever opening the skull — patients showed meaningful clinical improvement. This work has been replicated and debated extensively in the neurosurgical literature, with the Pediatric Craniocervical Society publishing a formal response examining the relationship between Chiari Type 1 and atlantoaxial instability (Bollo et al., J Neurosurg Pediatr, 2015 — PMID: 26340380).
Co-Existence of Chiari and AAI
A 2019 review in Child’s Nervous System directly examined the co-existence of Chiari and atlantoaxial instability. In a series of 86 pediatric cases of atlantoaxial subluxation, 12 (13.95%) had a Chiari malformation. Conversely, of 76 children operated on for Chiari, 11 (14.47%) had associated atlantoaxial subluxation (Salunke et al., Childs Nerv Syst, 2019 — PMID: 31302728). That is far higher than chance would predict, and it strongly suggests these two conditions share underlying mechanisms.
Connective Tissue Disorders and the Hypermobile Patient
A particularly important paper for our patients came out of Dr. Fraser Henderson’s group, examining the syndrome of occipitoatlantoaxial hypermobility, cranial settling, and Chiari Type I in patients with hereditary connective tissue disorders like Ehlers-Danlos syndrome. The authors found morphometric evidence — including cranial settling, posterior gliding of the occipital condyles, and reduction of the clivus-axis angle in the upright position — suggesting that hypermobility of the occipitoatlantal and atlantoaxial joints contributes to symptoms referable to basilar impression (Milhorat et al., J Neurosurg Spine, 2007 — PMID: 18074684).
A 5-year follow-up by Henderson and colleagues in Neurosurgical Review (2019) confirmed that cervical medullary syndrome secondary to craniocervical instability and ventral brainstem compression in patients with hereditary hypermobility disorders responds meaningfully to craniocervical reduction, fusion, and stabilization (Henderson et al., Neurosurg Rev, 2019 — PMID: 30627832).
Translation: when alignment and stability at the top of the neck are restored, the brainstem decompresses and symptoms improve — even in patients who had previously been told their problem was purely structural.
Why the Upper Cervical Spine Is at the Center of It All
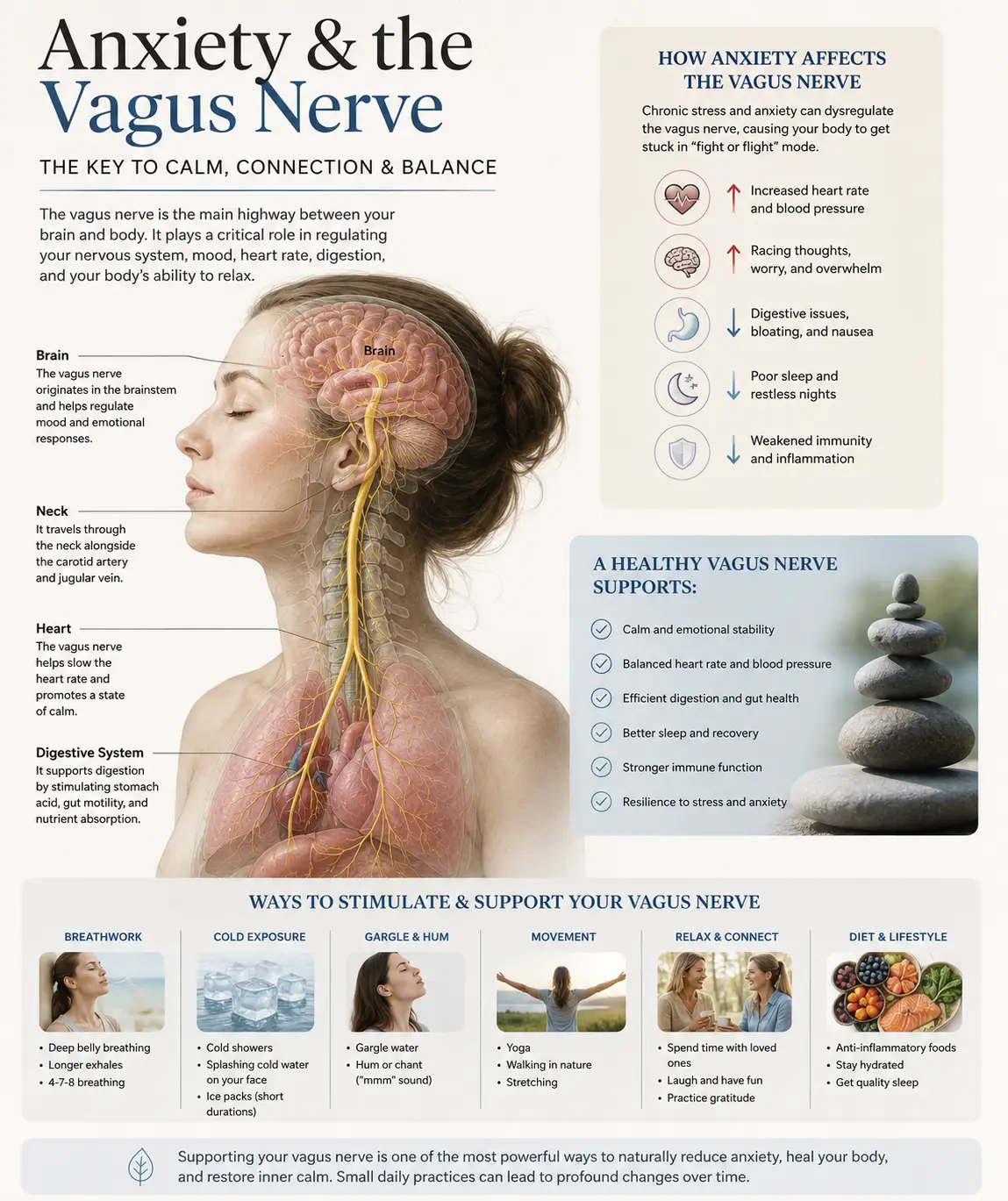
The atlas and axis aren’t just two vertebrae among many. They are the architectural foundation of your entire nervous system. Consider what passes through this tiny region:
- Your brainstem — controlling heart rate, blood pressure, respiration, digestion, balance, swallowing, and consciousness itself
- Cranial nerves IX through XII — including the vagus nerve, the master regulator of the parasympathetic nervous system
- The vertebral arteries — supplying the brainstem, cerebellum, and posterior brain
- Cerebrospinal fluid pathways — the cisterna magna and the foramen magnum
- Proprioceptive input — your upper neck has more proprioceptors per square inch than almost any other region of your body, and that input is essential for balance, eye movement coordination, and postural control
When the atlas and axis lose their normal alignment — whether from trauma, connective tissue laxity, congenital variation, or decades of compensation — every one of those structures can be affected.
In a patient with Chiari malformation, the cerebellar tonsils are already taking up space that should be free. Now add atlas misalignment or atlantoaxial instability on top of that, and you have a system under double strain. This is why patients with Chiari often feel dramatically worse after a whiplash, a fall, or even a strenuous chiropractic manipulation done by a general practitioner who didn’t understand the anatomy. The margin for error at this junction is incredibly small.
What the Research Says About Upper Cervical Care, CSF Flow, and Symptom Improvement
Let’s be honest and direct here. The neurosurgical research on Chiari and atlantoaxial instability is robust and growing. The research specifically on upper cervical chiropractic care for Chiari is smaller in scale — primarily case reports, case series, and imaging studies — but what exists is intriguing.
CSF Flow Studies with FONAR Upright MRI
Dr. Scott Rosa, working in collaboration with Dr. Raymond Damadian (the inventor of the MRI), has produced a series of imaging studies using FONAR Upright MRI to examine how upper cervical alignment affects cerebrospinal fluid flow at the craniocervical junction. His work, “Craniocervical Junction Realignment and Cerebrospinal Fluid Flow” (Rosa et al., 2013), documented measurable changes in CSF flow dynamics following gentle upper cervical correction in patients with craniocervical instability and Chiari-related conditions.
Engineering research has supported the importance of CSF flow at this junction. A computational fluid dynamics study published in the Journal of Biomechanical Engineering characterized hydrodynamic parameters of CSF at the craniovertebral junction in Type I Chiari patients before and after decompression surgery, confirming that localized obstruction at the upper cervical level meaningfully alters CSF dynamics (Pahlavian et al., PMC3794956).
Case Reports in the Chiropractic Literature
The Journal of Upper Cervical Chiropractic Research (May 2017) published a case study of a 6-year-old boy with Arnold-Chiari Malformation whose headaches and motion sickness resolved under specific upper cervical chiropractic care, with thermographic and radiographic confirmation of corrected subluxation. The authors appropriately noted that a single case cannot draw definitive conclusions, but documented a potential link between removing upper cervical vertebral subluxation and reduction of ACM symptoms.
Additional case reports in the broader chiropractic literature have documented improvement in vertigo, ataxic gait, nystagmus, and arm pain in adult patients with imaging-confirmed Chiari Type I following careful upper cervical care, with no adverse events when adjustments were skillfully and gently delivered.
What We Tell Our Patients Honestly
We are not surgeons. We do not — and cannot — surgically reduce a herniated cerebellar tonsil. What we can do is identify and correct the upper cervical misalignment that, in many patients, is layering symptoms on top of the underlying Chiari anatomy. When that alignment is restored, the system has a chance to calm down, CSF flow may improve, vagal tone may normalize, and many patients experience meaningful symptom relief.
For some patients, that means avoiding or delaying surgery. For others — particularly those who have already had decompression but still feel awful — it means finally addressing the upper cervical component that the surgery did not directly correct.
What to Expect at Lavender Family Chiropractic
Because Chiari and AAI are sensitive, complex conditions, our entire approach at Lavender Family Chiropractic / NeckWise North Sarasota is built around precision, gentleness, and measurable outcomes. Here’s what your care looks like:
Step 1: Complimentary consultation. We sit down with you, listen to your full history, and review your imaging. We want to understand exactly what you’re experiencing and what’s been tried.
Step 2: 3D Cone-Beam CT (CBCT) imaging. Standard 2D X-rays cannot adequately visualize the upper cervical junction. Our in-office CBCT measures your atlas and axis alignment in three dimensions, down to one-hundredth of a millimeter. This is critical when the margin for error is small.
Step 3: Functional nervous system scanning. Using paraspinal infrared thermography (Tytron), we assess how your autonomic nervous system is functioning. This gives us objective data — not guesswork.
Step 4: A personalized correction plan. We use the AHKC (Advanced Head-Knee-Chest) upper cervical technique, which is gentle, precise, and involves no popping, twisting, or cracking. The correction is calculated mathematically from your CBCT and delivered with sub-millimeter precision.
Step 5: Re-scans and re-imaging. We measure your progress objectively. We don’t ask you to take our word for it — we show you the data.
Step 6: Collaboration with your medical team. We are not a replacement for your neurologist or neurosurgeon. We work alongside them. If your case requires surgical evaluation, we’ll say so. If conservative care is appropriate, we’ll provide the most precise version of it available.
📞 If you’d like to schedule your complimentary consultation, call (941) 243-3729 or visit chiropractorsarasotaflorida.com to book online.
More Research: A Quick Reference List
For patients and providers who want to dive deeper into the literature, here are the key studies cited above:
- Goel A. Is atlantoaxial instability the cause of Chiari malformation? Outcome analysis of 65 patients treated by atlantoaxial fixation. J Neurosurg Spine. 2015. PMID: 25415487
- Salunke P, et al. Chiari malformation and atlantoaxial instability: problems of co-existence. Childs Nerv Syst. 2019. PMID: 31302728
- Milhorat TH, et al. Syndrome of occipitoatlantoaxial hypermobility, cranial settling, and Chiari malformation type I in patients with hereditary disorders of connective tissue. J Neurosurg Spine. 2007. PMID: 18074684
- Henderson FC Sr, et al. Cervical medullary syndrome secondary to craniocervical instability and ventral brainstem compression in hereditary hypermobility connective tissue disorders. Neurosurg Rev. 2019. PMID: 30627832
- Bollo RJ, et al. Chiari malformation Type 1 and atlantoaxial instability: a letter from the Pediatric Craniocervical Society. J Neurosurg Pediatr. 2015. PMID: 26340380
- Salunke P, et al. Is Cervical Stabilization for All Cases of Chiari-I Malformation an Overkill? Evidence Speaks Louder Than Words! 2019. PMID: 31261453
- Pahlavian SH, et al. Hydrodynamic and Longitudinal Impedance Analysis of Cerebrospinal Fluid Dynamics at the Craniovertebral Junction in Type I Chiari Malformation. PMC3794956
- Mendis A, et al. The Pathogenesis of Chiari Malformation and Syringomyelia: A Case Report and Systematic Review of Current Theories. PMC10656570
Sarasota, Lakewood Ranch, and the Communities We Serve
Lavender Family Chiropractic / NeckWise North Sarasota is proud to serve patients from across the Gulf Coast — including Sarasota, Lakewood Ranch, Bradenton, Parrish, Ellenton, Venice, Osprey, Punta Gorda, St. Petersburg, Siesta Key, Longboat Key, Lido Key, and Myakka City. We also regularly see patients traveling from across Manatee and Sarasota counties — and from as far as Tampa, Naples, and Fort Myers — for upper cervical care for Chiari and craniocervical instability.
Our office is located at the corner of University and Whitfield, just minutes from I-75, making it accessible from anywhere in the region.
Top 15 FAQs About Chiari Malformation, Atlantoaxial Instability, and Upper Cervical Care
1. Can upper cervical chiropractic care cure Chiari malformation?
No. Chiari malformation is a structural condition — the tonsils are anatomically positioned where they are, and no chiropractic adjustment can move them. However, upper cervical care may significantly improve the symptoms associated with Chiari by correcting overlying atlas/axis misalignment, improving CSF flow dynamics, and reducing brainstem irritation. Many patients experience meaningful relief without surgery.
2. Is upper cervical chiropractic safe if I have Chiari malformation?
When delivered by a properly trained upper cervical chiropractor using gentle, instrument-assisted or low-force techniques (like AHKC, NUCCA, or Atlas Orthogonal), the published case reports show no adverse events. Traditional high-velocity neck manipulation is generally not recommended in Chiari patients — which is exactly why our technique involves no popping, twisting, or cracking.
3. What is the difference between Chiari malformation and atlantoaxial instability?
Chiari involves the cerebellar tonsils descending below the foramen magnum. AAI involves excessive movement between the atlas (C1) and axis (C2). The two often coexist, and growing research suggests AAI may actually drive or worsen Chiari symptoms in many patients.
4. Do I need surgery for Chiari?
That depends on the severity of your symptoms, your imaging findings, and whether you have associated syringomyelia, basilar invagination, or progressive neurological deficits. Many patients with mild-to-moderate Chiari symptoms do well with conservative care. Always work with your neurosurgeon to make this decision.
5. Can atlantoaxial instability be diagnosed on a standard MRI?
Often it cannot. AAI is a dynamic instability that may only show up on flexion-extension imaging, upright MRI, or rotational CT scans. Many AAI patients have “normal” supine MRIs and remain undiagnosed for years.
6. I’ve already had decompression surgery and I still feel terrible. Can you help?
This is one of the most common scenarios we see. Decompression addresses the bony space at the foramen magnum but does not correct atlas/axis alignment. If upper cervical misalignment is contributing to your remaining symptoms, gentle correction may help. Many post-decompression patients have found relief at our office.
7. How does CBCT imaging compare to a standard MRI for evaluating my upper neck?
They show different things. MRI shows soft tissue (brain, spinal cord, ligaments, CSF). CBCT shows bony alignment in three dimensions with sub-millimeter precision. For planning a precise upper cervical correction, CBCT is invaluable. We use both as needed.
8. Are Chiari and Ehlers-Danlos syndrome related?
Yes — there is a well-documented overlap. Patients with EDS and other hereditary connective tissue disorders have a much higher rate of craniocervical instability, atlantoaxial instability, and Chiari-spectrum findings. The Milhorat and Henderson papers cited above are essential reading on this topic.
9. Will my insurance cover upper cervical care?
Our office is out of network with insurance. We provide superbills you can submit to your insurance for potential reimbursement based on your plan. We also offer multiple payment and financing options to make care accessible.
10. How long until I feel better?
Every case is different. Some patients report improvement within the first few visits as the nervous system begins to calm down. Others — especially those with longstanding instability or post-trauma cases — take longer. We measure your progress objectively with follow-up scans so you don’t have to guess.
11. Can children with Chiari benefit from upper cervical care?
In appropriate cases, yes. We provide gentle, age-appropriate care for pediatric patients and always coordinate with the child’s pediatrician and neurologist. The 2017 case report mentioned above documented improvement in a 6-year-old with Arnold-Chiari malformation.
12. What if my Chiari is “borderline” — only 3 or 4 mm of tonsillar descent?
Many “borderline” Chiari patients have significant symptoms driven primarily by upper cervical misalignment or AAI rather than the tonsillar position itself. This group often responds especially well to upper cervical correction.
13. Can a whiplash or car accident cause or worsen Chiari symptoms?
Yes. Trauma is a well-documented trigger for symptom onset in previously asymptomatic Chiari patients and a major cause of acquired atlantoaxial instability. If your symptoms started after a trauma, the upper cervical evaluation is especially important.
14. Do you work with my neurologist or neurosurgeon?
Absolutely. We routinely communicate with our patients’ medical teams. We see our role as complementary, not adversarial. If your case needs surgical evaluation, we will say so clearly.
15. How do I get started?
Call us at (941) 243-3729 or visit chiropractorsarasotaflorida.com to schedule your complimentary consultation. We’ll review your history, examine your spine and nervous system function, and let you know honestly whether we believe we can help.
Final Thoughts
If you’ve been diagnosed with Chiari malformation, atlantoaxial instability, or both — please know that you are not alone, and you are not without options. The neurosurgical literature has shifted dramatically over the past two decades, and we now understand that the craniocervical junction is one of the most important regions in the entire human body. When it works, everything downstream works better. When it doesn’t, the consequences ripple through your whole nervous system.
At Lavender Family Chiropractic / NeckWise North Sarasota, Dr. Rusty Lavender and Dr. Jacob Temple are committed to providing the most precise, gentlest, most measurable upper cervical care available — backed by 3D CBCT imaging, functional nervous system scans, and the AHKC technique. We’ve seen patients with Chiari and AAI go from years of suffering to genuine, measurable improvement. We would be honored to evaluate your case.
📍 5899 Whitfield Avenue, Suite 107, Sarasota, FL 34243 (corner of University and Whitfield) 📞 (941) 243-3729 🌐 chiropractorsarasotaflorida.com 📅 Book your complimentary consultation
You deserve answers. You deserve a plan. You deserve a team that takes the top of your neck as seriously as you do.
Related Articles
- When Your Head Feels Too Heavy: The Hidden Story of Craniocervical Instability, Vertigo, Neck Pain, and Migraines (and Why Upper Cervical Care May Be the Missing Link)
- Atlas Chiropractic and Upper Cervical Care: A Deep Dive into Lavender Family Chiropractic
- Vagus Nerve Dysfunction, Craniocervical Instability, and Upper Cervical Chiropractic Care in Sarasota, Florida for Proven Results
By Dr. Rusty Lavender and Dr. Jacob Temple — Lavender Family Chiropractic / NeckWise North Sarasota